| Revision as of 03:45, 12 October 2008 view sourceCostelld (talk | contribs)278 editsm →Genetic variability← Previous edit | Latest revision as of 20:56, 31 December 2024 view source Omnipaedista (talk | contribs)Autopatrolled, Extended confirmed users, Pending changes reviewers242,331 edits style fix per MOS:SECTIONORDER | ||
| Line 1: | Line 1: | ||
| {{short description|Human retrovirus, cause of AIDS}} | |||
| {{pp-semi-protected|small=yes}} | |||
| {{cs1 config|name-list-style=vanc}}{{Use mdy dates|date=December 2024}} | |||
| {{Taxobox | color=violet | |||
| {{About|the virus|the infection caused by the virus|HIV/AIDS|other uses}} | |||
| | name = ''Human immunodeficiency virus'' | |||
| {{Redirect|AIDS virus|the computer virus|AIDS (computer virus)}} | |||
| {{Good article}} | |||
| {{pp|small=yes}} | |||
| {{pp-move}} | |||
| {{Use mdy dates|date=June 2013}} | |||
| {{Paraphyletic group | |||
| | name = Human immunodeficiency viruses | |||
| | image = HIV-budding-Color.jpg | | image = HIV-budding-Color.jpg | ||
| | image_alt = Scanning electron micrograph of HIV-1 (in green) budding from cultured lymphocyte. Multiple round bumps on cell surface represent sites of assembly and budding of virions. | |||
| | image_width = 190px | |||
| | image_caption = Scanning electron micrograph of HIV-1 (in green) budding from cultured lymphocyte. Multiple round bumps on cell surface represent sites of assembly and budding of virions. | | image_caption = ] of HIV-1 (in green) budding from cultured ]. Multiple round bumps on cell surface represent sites of assembly and budding of virions. | ||
| | |
| auto = virus | ||
| | parent = Lentivirus | |||
| | familia = '']'' | |||
| | includes = | |||
| | genus = '']'' | |||
| *'']'' | |||
| | subdivision_ranks = Species | |||
| *'']'' | |||
| | subdivision = | |||
| | excludes_text = Other lentiviruses | |||
| * '''''Human immunodeficiency virus 1''''' | |||
| | excludes = | |||
| * '''''Human immunodeficiency virus 2''''' | |||
| *'']'' | |||
| *'']'' | |||
| *'']'' | |||
| *'']'' | |||
| *'']'' | |||
| *'']'' | |||
| *'']'' | |||
| *'']'' | |||
| }} | }} | ||
| {{DiseaseDisorder infobox | | |||
| Name = International Statistical Classification of Diseases and Related Health Problems Codes | | |||
| ICD10 = B20-B24 | | |||
| ICD9 = {{ICD9|042}}-{{ICD9|044}} | | |||
| }} | |||
| '''Human immunodeficiency virus''' ('''HIV''') is a ] (a member of the ] family) that can lead to '']'' (AIDS), a condition in ]s in which the ] begins to fail, leading to life-threatening ]s. Previous names for the ] include '''human T-lymphotropic virus-III''' ('''HTLV-III'''), '''lymphadenopathy-associated virus''' ('''LAV'''), and '''AIDS-associated retrovirus''' ('''ARV''').<ref>{{cite web| author=Rick Sowadsky| year=1999 |date = 1999-02-24 |url=http://www.thebody.com/Forums/AIDS/safesex/Archive/origins/Q8777.html |title=What is HTLV-III?| accessdate=2008-04-03}}</ref><ref name=Coffin>{{cite journal | |||
| | author=Coffin, J., Haase, A., Levy, J. A., Montagnier, L., Oroszlan, S., Teich, N., Temin, H., Toyoshima, K., Varmus, H., Vogt, P. and Weiss, R. A. | title=What to call the AIDS virus? | journal=Nature | year=1986 | pages=10 | volume=321 | issue=6065 | pmid=3010128| doi=10.1038/321010a0}}</ref> | |||
| The '''human immunodeficiency viruses''' ('''HIV''') are two species of '']'' (a subgroup of ]) that infect humans. Over time, they cause ] (AIDS),<ref name="pmid8493571">{{cite journal | vauthors = Weiss RA | title = How does HIV cause AIDS? | journal = Science | volume = 260 | issue = 5112 | pages = 1273–9 | date = May 1993 | pmid = 8493571 | doi = 10.1126/science.8493571 | bibcode = 1993Sci...260.1273W }}</ref><ref name="pmid18947296">{{cite journal | vauthors = Douek DC, Roederer M, Koup RA | title = Emerging Concepts in the Immunopathogenesis of AIDS | journal = Annual Review of Medicine | volume = 60 | pages = 471–84 | year = 2009 | pmid = 18947296 | pmc = 2716400 | doi = 10.1146/annurev.med.60.041807.123549 }}</ref> a condition in which progressive failure of the ] allows life-threatening ]s and ]s to thrive.<ref name="pmid27611681">{{cite journal | vauthors = Powell MK, Benková K, Selinger P, Dogoši M, Kinkorová Luňáčková I, Koutníková H, Laštíková J, Roubíčková A, Špůrková Z, Laclová L, Eis V, Šach J, Heneberg P | title = Opportunistic Infections in HIV-Infected Patients Differ Strongly in Frequencies and Spectra between Patients with Low CD4+ Cell Counts Examined Postmortem and Compensated Patients Examined Antemortem Irrespective of the HAART Era | journal = PLOS ONE | volume = 11 | issue = 9 | pages = e0162704 | year = 2016 | pmid = 27611681 | pmc = 5017746 | doi = 10.1371/journal.pone.0162704 | bibcode = 2016PLoSO..1162704P | doi-access = free }}</ref> Without treatment, the average survival time after infection with HIV is estimated to be 9 to 11 years, depending on the ].<ref name=UNAIDS2007>{{cite web| date = December 2007| title = 2007 AIDS epidemic update| url=https://data.unaids.org/pub/epislides/2007/2007_epiupdate_en.pdf#page16 | author1 = UNAIDS| author2 = WHO | page=16}}</ref> | |||
| Infection with HIV occurs by the transfer of ], ], ], ], or ]. Within these bodily fluids, HIV is present as both free virus particles and virus within infected immune cells. The four major routes of transmission are ], contaminated needles, breast milk, and transmission from an infected mother to her baby at ]. Screening of blood products for HIV has largely eliminated transmission through blood transfusions or infected blood products in the ]. | |||
| In most cases, HIV is a ] and ] by contact with or transfer of ], ], ], and ].<ref name="PARTNER2-2019">{{cite journal |display-authors=6 |vauthors=Rodger AJ, Cambiano V, Bruun T, Vernazza P, Collins S, Degen O, Corbelli GM, Estrada V, Geretti AM, Beloukas A, Raben D, Coll P, Antinori A, Nwokolo N, Rieger A, Prins JM, Blaxhult A, Weber R, Van Eeden A, Brockmeyer NH, Clarke A, Del Romero Guerrero J, Raffi F, Bogner JR, Wandeler G, Gerstoft J, Gutiérrez F, Brinkman K, Kitchen M, Ostergaard L, Leon A, Ristola M, Jessen H, Stellbrink HJ, Phillips AN, Lundgren J |date=June 2019 |title=Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): final results of a multicentre, prospective, observational study |journal=Lancet |volume=393 |issue=10189 |pages=2428–2438 |doi=10.1016/S0140-6736(19)30418-0 |pmc=6584382 |pmid=31056293 |doi-access=free}}</ref><ref name="Fauci-JAMA">{{cite journal |author-link3=Anthony S. Fauci |vauthors=Eisinger RW, Dieffenbach CW, Fauci AS |date=February 2019 |title=HIV Viral Load and Transmissibility of HIV Infection: Undetectable Equals Untransmittable |journal=JAMA |volume=321 |issue=5 |pages=451–452 |doi=10.1001/jama.2018.21167 |pmid=30629090 |s2cid=58599661}}</ref> Non-sexual transmission can occur from an infected mother to her infant during ], during ] by exposure to her blood or vaginal fluid, and through ].<ref>{{cite journal | vauthors = Mabuka J, Nduati R, Odem-Davis K, Peterson D, Overbaugh J | title = HIV-Specific Antibodies Capable of ADCC Are Common in Breastmilk and Are Associated with Reduced Risk of Transmission in Women with High Viral Loads | journal = PLOS Pathogens | volume = 8 | issue = 6 | pages = e1002739 | year = 2012 | pmid = 22719248 | pmc = 3375288 | doi = 10.1371/journal.ppat.1002739 | veditors = Desrosiers RC | doi-access = free }}</ref><ref>{{Cite book |title=Anthropology and public health : bridging differences in culture and society |date=2009 |publisher=Oxford University Press | veditors = Hahn RA, Inhorn MC |isbn=978-0-19-537464-3 |edition=2nd |location=Oxford |pages = 449 |oclc=192042314}}</ref><ref name="Mead">{{cite journal |author = Mead MN |title = Contaminants in human milk: weighing the risks against the benefits of breastfeeding |journal = Environmental Health Perspectives |volume = 116 |issue = 10 |pages = A426–34 |year = 2008 |pmid = 18941560 |pmc = 2569122 |doi = 10.1289/ehp.116-a426 |url = http://www.ehponline.org/members/2008/116-10/focus.html |url-status = dead |archive-url = https://web.archive.org/web/20081106182431/http://www.ehponline.org/members/2008/116-10/focus.html |archive-date = 6 November 2008 |df = dmy-all }}</ref><ref>{{citation-attribution|1={{cite web|url=https://www.hiv.gov/hiv-basics/hiv-prevention/reducing-mother-to-child-risk/preventing-mother-to-child-transmission-of-hiv|title=Preventing Mother-to-Child Transmission of HIV|website=HIV.gov|access-date=2017-12-08|date=2017-05-15}}}}</ref> Within these bodily fluids, HIV is present as both free ] particles and virus within infected ]. | |||
| HIV infection in humans is now ]. As of January 2006, the ] (UNAIDS) and the ] (WHO) estimate that AIDS has killed more than 25 million people since it was first recognized on December 1, 1981. It is estimated that about 0.6 percent of the world's population is infected with HIV.<ref name=UNAIDS2006>{{cite book | |||
| Research has shown (for both same-sex and opposite-sex couples) that HIV is not contagious during sexual intercourse without a condom if the HIV-positive partner has a consistently undetectable ].<ref name = PARTNER2-2019 /><ref name = Fauci-JAMA /> | |||
| | author =] | |||
| | year = 2006 | |||
| | title = 2006 Report on the global AIDS epidemic | |||
| | chapter = Overview of the global AIDS epidemic | |||
| | chapterurl = http://data.unaids.org/pub/GlobalReport/2006/2006_GR_CH02_en.pdf | |||
| | accessdate = 2006-06-08 | |||
| | format= ] | |||
| }}</ref> In 2005 alone, AIDS claimed an estimated 2.4–3.3 million lives, of which more than 570,000 were children. A third of these deaths are occurring in ]n ], retarding ] and increasing ].<ref name=Greener>{{cite book | |||
| | author =Greener, R. | |||
| | year = 2002 | |||
| | title = State of The Art: AIDS and Economics | |||
| | chapter = AIDS and macroeconomic impact | |||
| | chapterurl = http://www.popline.org/docs/285428 | |||
| | editor = S, Forsyth (ed.) | |||
| | edition = | |||
| | pages = 49-55 | |||
| | publisher = IAEN | |||
| }}</ref> According to current estimates, HIV is set to infect 90 million people in ], resulting in a minimum estimate of 18 million ]s.<ref name=UNAIDS>{{cite web | |||
| | author=] | |||
| | publisher= | |||
| | publishyear= 2005 | |||
| | url=http://www.unaids.org/epi/2005/doc/EPIupdate2005_pdf_en/epi-update2005_en.pdf | |||
| | title=AIDS epidemic update, 2005 | |||
| | accessdate=2006-02-28|format=] | |||
| }}</ref> ] treatment reduces both the ] and the ] of HIV infection, but routine access to antiretroviral medication is not available in all countries.<ref name=Palella>{{cite journal | |||
| | author=Palella, F. J. Jr, Delaney, K. M., Moorman, A. C., Loveless, M. O., Fuhrer, J., Satten, G. A., Aschman and D. J., Holmberg, S. D. | |||
| | title=Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection. HIV Outpatient Study Investigators | |||
| | journal=N. Engl. J. Med | |||
| | year=1998 | |||
| | pages=853–860 | |||
| | volume=338 | |||
| | issue=13 | |||
| | pmid=9516219 | |||
| | doi=10.1056/NEJM199803263381301 | |||
| }}</ref> | |||
| HIV |
HIV infects vital cells in the human immune system, such as ] (specifically ]<SUP>+</SUP> T cells), ]s, and ]s.<ref>{{cite journal | vauthors = Cunningham AL, Donaghy H, Harman AN, Kim M, Turville SG | title = Manipulation of dendritic cell function by viruses | journal = Current Opinion in Microbiology | volume = 13 | issue = 4 | pages = 524–9 | date = August 2010 | pmid = 20598938 | doi = 10.1016/j.mib.2010.06.002 }}</ref> HIV infection leads to low levels of CD4<SUP>+</SUP> T cells through a number of mechanisms, including ] of abortively infected T cells,<ref name="pmid24356306">{{cite journal | vauthors = Doitsh G, Galloway NL, Geng X, Yang Z, Monroe KM, Zepeda O, Hunt PW, Hatano H, Sowinski S, Muñoz-Arias I, Greene WC | display-authors = 6 | title = Cell death by pyroptosis drives CD4 T-cell depletion in HIV-1 infection | journal = Nature | volume = 505 | issue = 7484 | pages = 509–14 | date = January 2014 | pmid = 24356306 | pmc = 4047036 | doi = 10.1038/nature12940 | bibcode = 2014Natur.505..509D }}</ref> ] of uninfected bystander cells,<ref>{{cite journal | vauthors = Garg H, Mohl J, Joshi A | title = HIV-1 induced bystander apoptosis | journal = Viruses | volume = 4 | issue = 11 | pages = 3020–43 | date = November 2012 | pmid = 23202514 | pmc = 3509682 | doi = 10.3390/v4113020 | doi-access = free }}</ref> direct viral killing of infected cells, and killing of infected CD4<SUP>+</SUP> T cells by ]s that recognize infected cells.<ref>{{cite book | vauthors = Kumar V |title=Robbins Basic Pathology |year=2012 |isbn=978-1-4557-3787-1 |pages = 147 |publisher=Elsevier Health Sciences |url=https://books.google.com/books?id=jheBzf17C7YC&pg=PA147 |edition=9th }}</ref> When CD4<SUP>+</SUP> T cell numbers decline below a critical level, ] is lost, and the body becomes progressively more susceptible to opportunistic infections, leading to the development of AIDS. | ||
| {{TOC limit|3}} | |||
| ==Virology== | |||
| Eventually most HIV-infected individuals develop ]. These individuals mostly die from ]s or ] associated with the progressive failure of the immune system.<ref name=Lawn>{{ | |||
| {| class="wikitable" style="float:center; font-size:85%; margin-left:15px;" | |||
| cite journal | |||
| | author=Lawn SD | |||
| | title=AIDS in Africa: the impact of coinfections on the pathogenesis of HIV-1 infection | |||
| | journal=J. Infect. Dis. | year=2004 | pages=1–12 | volume=48 | issue=1 | |||
| | pmid=14667787 | |||
| }}</ref> Without treatment, about 9 out of every 10 persons with HIV will progress to AIDS after 10-15 years. Many progress much sooner.<ref name=Buchbinder>{{cite journal | |||
| | author=Buchbinder SP, Katz MH, Hessol NA, O'Malley PM, Holmberg SD. | |||
| | title=Long-term HIV-1 infection without immunologic progression | |||
| | journal=AIDS | |||
| | year=1994 | |||
| | pages=1123–8 | |||
| | volume=8 | |||
| | issue=8 | |||
| | pmid=7986410 | |||
| | doi=10.1097/00002030-199408000-00014 | |||
| }}</ref> Treatment with anti-retrovirals increases the life expectancy of people infected with HIV. Even after HIV has progressed to diagnosable AIDS, the average survival time with antiretroviral therapy (as of 2005) is estimated to be more than 5 years.<ref name=Schneider>{{ | |||
| cite journal | |||
| | author=Schneider MF, Gange SJ, Williams CM, Anastos K, Greenblatt RM, Kingsley L, Detels R, Munoz A | |||
| | title=Patterns of the hazard of death after AIDS through the evolution of antiretroviral therapy: 1984–2004 | |||
| | journal=AIDS | year=2005 | pages=2009–18 | volume=19 | issue=17 | |||
| | pmid=16260908 | |||
| }}</ref> Without antiretroviral therapy, death normally occurs within a year.<ref name=Morgan2>{{ | |||
| cite journal | |||
| | author=Morgan D, Mahe C, Mayanja B, Okongo JM, Lubega R, Whitworth JA | |||
| | title=HIV-1 infection in rural Africa: is there a difference in median time to AIDS and survival compared with that in industrialized countries? | |||
| | journal=AIDS | year=2002 | pages=597–632 | volume=16 | issue=4 | pmid=11873003 | |||
| }}</ref> It is hoped that current and future treatments may allow HIV-infected individuals to achieve a life expectancy approaching that of the general public. | |||
| ==Classification== | |||
| HIV is a member of the ] ],<ref name=ICTV61.0.6>{{cite web | |||
| | author=] | |||
| | publisher=] | |||
| | publishyear=2002 | |||
| | url=http://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/61060000.htm | |||
| | title=61.0.6. Lentivirus | |||
| | accessdate=2006-02-28 | |||
| }}</ref> part of the family of ].<ref name=ICTV61.>{{cite web | |||
| | author=] | |||
| | publisher=] | |||
| | publishyear=2002 | |||
| | url=http://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/61000000.htm | |||
| | title=61. Retroviridae | |||
| | accessdate=2006-02-28 | |||
| }}</ref> Lentiviruses have many common ] and ] properties. Many species are infected by lentiviruses, which are characteristically responsible for long-duration illnesses with a long ] period.<ref name=Levy>{{cite journal | |||
| | author=Lévy, J. A. | |||
| | title=HIV pathogenesis and long-term survival | |||
| | journal=AIDS | |||
| | year=1993 | |||
| | pages=1401–10 | |||
| | volume=7 | |||
| | issue=11 | |||
| | pmid=8280406 | |||
| | doi=10.1097/00002030-199311000-00001 | |||
| }}</ref> Lentiviruses are transmitted as single-stranded, positive-], enveloped ]es. Upon entry of the target cell, the viral ] ] is converted to double-stranded ] by a virally encoded ] that is present in the virus particle. This viral DNA is then integrated into the cellular DNA by a virally encoded ], along with host cellular co-factors,<ref name="JASmith">{{cite journal | author= Smith, Johanna A.; Daniel, René (Division of Infectious Diseases, Center for Human Virology, Thomas Jefferson University, Philadelphia) |title= Following the path of the virus: the exploitation of host DNA repair mechanisms by retroviruses |journal=ACS Chem Biol|volume=1|issue=4 |pages= 217–26 | year= 2006 |pmid= 17163676 |doi=10.1021/cb600131q |url= }}</ref> so that the genome can be ]. Once the virus has infected the cell, two pathways are possible: either the virus becomes ] and the infected cell continues to function, or the virus becomes active and replicates, and a large number of virus particles are liberated that can then infect other cells. | |||
| There are two strains of HIV known to exist: HIV-1 and HIV-2. HIV-1 is the virus that was initially discovered and termed LAV. It is more virulent, relatively easily transmitted, and is the cause of the majority of HIV infections globally. HIV-2 is less transmittable and is largely confined to ].<ref name=Reeves>{{cite journal | |||
| | author=Reeves, J. D. and Doms, R. W | |||
| | title=Human Immunodeficiency Virus Type 2 | |||
| | journal=J. Gen. Virol. | year=2002 | pages=1253–65 | volume=83 | issue=Pt 6 | |||
| | pmid=12029140 | |||
| }}</ref> | |||
| {|class="wikitable" | |||
| |+Comparison of HIV species | |+Comparison of HIV species | ||
| |- | |- | ||
| ! Species !! ] !! |
! Species !! ] !! ] !! Prevalence !! Inferred origin | ||
| |- | |- | ||
| ! HIV-1 | ! HIV-1 | ||
| | High || High || Global || ] | | High || High || Global || ] | ||
| |- | |- | ||
| ! HIV-2 | ! HIV-2 | ||
| | Lower || Low || West Africa || ] | | Lower || Low || West Africa || ] | ||
| |} | |} | ||
| ===Classification=== | |||
| {{see also|Subtypes of HIV}} | |||
| HIV is a member of the ] '']'',<ref name="ICTV61.0.6">{{cite web |author=International Committee on Taxonomy of Viruses |author-link=International Committee on Taxonomy of Viruses |year=2002 |title=61.0.6. Lentivirus |url=https://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/61060000.htm |url-status=usurped |archive-url=https://web.archive.org/web/20061014181406/https://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/61060000.htm |archive-date=October 14, 2006 |access-date=February 28, 2006 |publisher=]}}</ref> part of the family '']''.<ref name="ICTV61.">{{cite web |author=International Committee on Taxonomy of Viruses |year=2002 |title=61. Retroviridae |url=https://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/61000000.htm |url-status=usurped |archive-url=https://web.archive.org/web/20061002234645/https://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/61000000.htm |archive-date=October 2, 2006 |access-date=February 28, 2006 |publisher=National Institutes of Health}}</ref> Lentiviruses have many ] and ] properties in common. Many species are infected by lentiviruses, which are characteristically responsible for long-duration illnesses with a long ].<ref name=Levy>{{cite journal | vauthors = Levy JA | title = HIV pathogenesis and long-term survival | journal = AIDS | volume = 7 | issue = 11 | pages = 1401–10 | date = November 1993 | pmid = 8280406 | doi = 10.1097/00002030-199311000-00001 }}</ref> Lentiviruses are transmitted as ], positive-], ] ]es. Upon entry into the target cell, the viral ] ] is converted (reverse transcribed) into double-stranded ] by a virally encoded enzyme, ], that is transported along with the viral genome in the virus particle. The resulting viral DNA is then imported into the ] and integrated into the cellular DNA by a virally encoded enzyme, ], and host ].<ref name="JASmith">{{cite journal | vauthors = Smith JA, Daniel R | title = Following the path of the virus: the exploitation of host DNA repair mechanisms by retroviruses | journal = ACS Chemical Biology | volume = 1 | issue = 4 | pages = 217–26 | date = May 2006 | pmid = 17163676 | doi = 10.1021/cb600131q }}</ref> Once integrated, the virus may become ], allowing the virus and its host cell to avoid detection by the immune system, for an indeterminate amount of time.<ref name="HIV Latency">{{cite journal | vauthors = Siliciano RF, Greene WC | title = HIV latency | journal = Cold Spring Harbor Perspectives in Medicine | volume = 1 | issue = 1 | pages = a007096 | date = September 2011 | pmid = 22229121 | pmc = 3234450 | doi = 10.1101/cshperspect.a007096 }}</ref> The virus can remain dormant in the human body for up to ten years after primary infection; during this period the virus does not cause symptoms. Alternatively, the integrated viral DNA may be ], producing new RNA genomes and viral proteins, using host cell resources, that are packaged and released from the cell as new virus particles that will begin the replication cycle anew. | |||
| Two types of HIV have been characterized: HIV-1 and HIV-2. HIV-1 is the virus that was initially discovered and termed both lymphadenopathy associated virus (LAV) and human T-lymphotropic virus 3 (HTLV-III). HIV-1 is more ] and more ] than HIV-2,<ref>{{cite journal | vauthors = Gilbert PB, McKeague IW, Eisen G, Mullins C, Guéye-NDiaye A, Mboup S, Kanki PJ | title = Comparison of HIV-1 and HIV-2 infectivity from a prospective cohort study in Senegal | journal = Statistics in Medicine | volume = 22 | issue = 4 | pages = 573–593 | date = February 28, 2003 | pmid = 12590415 | doi = 10.1002/sim.1342 | s2cid = 28523977 }}</ref> and is the cause of the majority of HIV infections globally. The lower infectivity of HIV-2, compared to HIV-1, implies that fewer of those exposed to HIV-2 will be infected per exposure. Due to its relatively poor capacity for transmission, HIV-2 is largely confined to ].<ref name=Reeves>{{cite journal | vauthors = Reeves JD, Doms RW | title = Human Immunodeficiency Virus Type 2 | journal = ] | volume = 83 | issue = Pt 6 | pages = 1253–65 | year = 2002 | pmid = 12029140 | doi = 10.1099/0022-1317-83-6-1253 | doi-access = free }}</ref> | |||
| ==History== | |||
| ===Origin=== | |||
| {{Main|AIDS origin}} | |||
| HIV is thought to have originated in non-human ]s in sub-Saharan Africa and transferred to humans early in the 20th century.<ref name="urlAccess : : Nature">{{cite web |url=http://www.nature.com/nature/journal/v455/n7213/full/nature07390.html |title=Worobey et al : : Nature |format= |work= |accessdate=}}</ref> The first paper recognizing a pattern of opportunistic infections was published on 4 June 1981.<ref name=MMWR2>{{cite web |url=http://www.cdc.gov/MMWR/preview/mmwrhtml/00043494.htm |title=Pneumocystis Pneumonia -- Los Angeles |format= |work= |accessdate=2008-05-05}}</ref> | |||
| ===Structure and genome=== | |||
| Two species of HIV infect humans: HIV-1 and HIV-2. Both species of the virus are believed to have originated in West-Central Africa and jumped species (]) from a non-human primate to humans. HIV-1 is thought to have originated in southern ] after jumping from wild ]s (''Pan troglodytes troglodytes'') to humans during the twentieth century.<ref name=Gao>{{cite journal | |||
| {{Main|Structure and genome of HIV}} | |||
| | author=Gao, F., Bailes, E., Robertson, D. L., Chen, Y., Rodenburg, C. M., Michael, S. F., Cummins, L. B., Arthur, L. O., Peeters, M., Shaw, G. M., Sharp, P. M., and Hahn, B. H. | |||
| ] | |||
| | title=Origin of HIV-1 in the Chimpanzee Pan troglodytes troglodytes | |||
| HIV is similar in structure to other retroviruses. It is roughly spherical<ref name=McGovern>{{cite journal | vauthors = McGovern SL, Caselli E, Grigorieff N, Shoichet BK | title = A common mechanism underlying promiscuous inhibitors from virtual and high-throughput screening | journal = Journal of Medicinal Chemistry | volume = 45 | issue = 8 | pages = 1712–22 | year = 2002 | pmid = 11931626 | doi = 10.1021/jm010533y | hdl = 11380/977912 }}</ref> with a diameter of about 120 ], around 100,000 times smaller in volume than a ].<ref name=Microbiology3>Compared with overview in: {{cite book | vauthors = Fisher B, Harvey RP, Champe PC |title=Lippincott's Illustrated Reviews: Microbiology |publisher=Lippincott Williams & Wilkins |location=Hagerstown, MD |year=2007 |pages = 3 |isbn=978-0-7817-8215-9 }}</ref> It is composed of two copies of positive-] ] ] that codes for the virus' nine ]s enclosed by a conical ] composed of 2,000 copies of the viral protein ].<ref name=compendia>{{cite book | author = Various | year = 2008 | title = HIV Sequence Compendium 2008 Introduction | url = http://www.hiv.lanl.gov/content/sequence/HIV/COMPENDIUM/2008/frontmatter.pdf | access-date = March 31, 2009 }}</ref> The single-stranded RNA is tightly bound to nucleocapsid proteins, p7, and enzymes needed for the development of the virion such as ], ]s, ] and ]. A matrix composed of the viral protein p17 surrounds the capsid ensuring the integrity of the virion particle.<ref name=compendia /> | |||
| | journal=Nature | |||
| | year=1999 | |||
| | pages=436–441 | |||
| | volume=397 | |||
| | issue=6718 | |||
| | pmid=9989410 | |||
| | doi=10.1038/17130 | |||
| }}</ref><ref name=Keele>{{cite journal | |||
| | author=Keele, B. F., van Heuverswyn, F., Li, Y. Y., Bailes, E., Takehisa, J., Santiago, M. L., Bibollet-Ruche, F., Chen, Y., Wain, L. V., Liegois, F., Loul, S., Mpoudi Ngole, E., Bienvenue, Y., Delaporte, E., Brookfield, J. F. Y., Sharp, P. M., Shaw, G. M., Peeters, M., and Hahn, B. H. | |||
| | title=Chimpanzee Reservoirs of Pandemic and Nonpandemic HIV-1 | |||
| | journal=Science | year=2006 | pages= 523| volume=Online ] | issue= | |||
| | url= http://www.sciencemag.org/cgi/content/abstract/1126531 | |||
| | doi = 10.1126/science.1126531 | |||
| | format= | |||
| | pmid=16728595 | |||
| }} | |||
| </ref> It evolved from a ] (SIV<sub><small>cpz</small></sub>)<ref></ref> HIV-2, on the other hand, may have originated from the ] (''Cercocebus atys''), an Old World monkey of ], ], and ].<ref name=Reeves>{{cite journal | |||
| | author=Reeves, J. D. and Doms, R. W | |||
| | title=Human Immunodeficiency Virus Type 2 | |||
| | journal=J. Gen. Virol. | year=2002 | pages=1253–1265 | volume=83 | issue=Pt 6 | |||
| | pmid= 12029140 | |||
| }}</ref> | |||
| ] are an interesting exception to the transmission of HIV. Their ] is believed to be caused by ] of the ] gene into an ] of ]. The result is fusion gene that provides the ] with resistance to ] infection. | |||
| <ref name=Goodier>{{cite journal | |||
| | author=Goodier, J., and Kazazian, H. | |||
| | title=Retrotransposons Revisited: The Restraint and Rehabilitation of Parasites | |||
| | journal=Cell | year=2008 | pages=23-35 | volume=135 | issue=1 | |||
| | url = http://www.sciencedirect.com/science/article/B6WSN-4TK9636-8/2/2af3e1e709ed15939505cf676ce4957c | |||
| | doi = 10.1016/j.cell.2008.09.022 |accessdate=2008-10-10 | |||
| }}</ref> | |||
| ===Early history=== | |||
| :''See ] for early cases of HIV / AIDS'' | |||
| ===Discovery=== | |||
| Controversy surrounding the discovery of HIV was intense after ] scientist ] and ] researcher ] both claimed to have discovered it, in 1983 and 1984 respectively.<ref name="Phyllida1991">{{cite journal|last=Brown|first=Phyllida|date=25 May 1991|title=The strains of the HIV war|journal=]|url=http://www.newscientist.com/channel/health/mg13017703.800-the-strains-of-the-hiv-war.html}}</ref> In 1987 the dispute was initially settled on a political level with both teams receiving equal credit.<ref name="Phyllida1991"/> In 1991 a study confirmed that the samples in Gallo's laboratory had in fact originated in Montagnier's.<ref name="Phyllida1991"/> In 1994 the US Government conceded that the French should receive the lion's share of the credit.<ref>{{cite web | |||
| |url=http://www.latimes.com/news/nationworld/nation/la-sci-nobel7-2008oct07,0,4512963.story | |||
| |title=Nobel Prize awarded for AIDS, cervical cancer research - | |||
| |publisher=Los Angeles Times | |||
| |format= | |||
| |work= | |||
| |accessdate=2008-10-06 | |||
| }}</ref> | |||
| The ] awarded half of the 2008 ] to Montagnier and his colleague ] 'for their discovery of "human immunodeficiency virus"'. The other half went to ] for unrelated work on ].<ref name="karolinskaOct6"> | |||
| {{cite press release |url=http://nobelprize.org/nobel_prizes/medicine/laureates/2008/press.html |title=The Nobel Prize in Physiology or Medicine 2008|date=2008-10-06|publisher=]|accessdate=2008-10-07}}</ref> Gallo was reported to have said that it was "a disappointment" not to have been included, but that all three of the award's recipients deserved the honor. <ref name="nobelAp">{{ | |||
| cite news | |||
| | author=Ritter, K and Moore, M | |||
| | title=3 European scientists share Nobel medicine prize | |||
| | date=October 6, 2008 | |||
| | url=http://news.yahoo.com/s/ap/20081006/ap_on_re_eu/eu_sweden_nobel_medicine | |||
| | agency= | |||
| | accessdate = 2008-10-06 | |||
| }}</ref> The Karolinska Institute's press release stated "Soon after the discovery of the virus, several groups contributed to the definitive demonstration of HIV as the cause of acquired human immunodeficiency syndrome (AIDS)."<ref name="karolinskaOct6"/> | |||
| ==Transmission== | |||
| {| class="prettytable" style="float:right; font-size:85%; margin-left:15px;" | |||
| |- bgcolor="#efefef" | |||
| |+ Estimated per act risk for acquisition<br/>of HIV by exposure route<ref name=MMWR3>{{ | |||
| cite journal | author=Smith DK, Grohskopf LA, Black RJ, et al | title=Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug Use, or Other Nonoccupational Exposure to HIV in the United States | journal=MMWR | year=2005 | pages=1–20 | volume=54 | issue=RR02 | url=http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5402a1.htm#tab1 | |||
| }}</ref> | |||
| |- bgcolor="#efefef" | |||
| ! style="width: 100px" abbr="Route" | Exposure Route | |||
| ! style="width: 130px" abbr="Infections" | Estimated infections<br/>per 10,000 exposures<br/>to an infected source | |||
| |- | |||
| ! style="text-align:left"| Blood Transfusion | |||
| | 9,000<ref name=Donegan>{{ | |||
| cite journal | author=Donegan E, Stuart M, Niland JC, et al | title=Infection with human immunodeficiency virus type 1 (HIV-1) among recipients of antibody-positive blood donations | journal=Ann. Intern. Med. | year=1990 | pages=733–739 | volume=113 | issue=10 | |||
| | pmid=2240875 | |||
| }}</ref> | |||
| |- | |||
| ! style="text-align:left"| Childbirth | |||
| | 2,500<ref name=Coovadia>{{ | |||
| cite journal | author=Coovadia H | title=Antiretroviral agents—how best to protect infants from HIV and save their mothers from AIDS | journal=N. Engl. J. Med. | year=2004 | pages=289–292 | volume=351 | issue=3 | pmid=15247337 | |||
| }}</ref> | |||
| |- | |||
| ! style="text-align:left"| Needle-sharing injection drug use | |||
| | 67<ref name=Kaplan>{{ | |||
| cite journal | author=Kaplan EH, Heimer R | title=HIV incidence among New Haven needle exchange participants: updated estimates from syringe tracking and testing data | journal=J. Acquir. Immune Defic. Syndr. Hum. Retrovirol. | year=1995 | pages=175–176 | volume=10 | issue=2 | |||
| | pmid=7552482 | |||
| }}</ref> | |||
| |- | |||
| ! style="text-align:left"| Percutaneous needle stick | |||
| | 30<ref name=Bell>{{ | |||
| cite journal | author=Bell DM | title=Occupational risk of human immunodeficiency virus infection in healthcare workers: an overview. | journal=Am. J. Med. | year=1997 | pages=9–15 | volume=102 | issue=5B | pmid=9845490 | |||
| }}</ref> | |||
| |- | |||
| ! style="text-align:left"| Receptive anal intercourse<sup>*</sup> | |||
| | 50<ref name=ESG>{{ | |||
| cite journal | author=European Study Group on Heterosexual Transmission of HIV | title=Comparison of female to male and male to female transmission of HIV in 563 stable couples | journal=BMJ. | year=1992 | pages=809–813 | volume=304 | issue=6830 | pmid=1392708 | |||
| }}</ref><ref name=Varghese>{{ | |||
| cite journal | author=Varghese B, Maher JE, Peterman TA, Branson BM,Steketee RW | title=Reducing the risk of sexual HIV transmission: quantifying the per-act risk for HIV on the basis of choice of partner, sex act, and condom use | journal=Sex. Transm. Dis. | year=2002 | pages=38–43 | volume=29 | issue=1 | pmid=11773877 | |||
| }}</ref> | |||
| |- | |||
| ! style="text-align:left"| Insertive anal intercourse<sup>*</sup> | |||
| | 6.5<ref name=ESG /><ref name=Varghese /> | |||
| |- | |||
| ! style="text-align:left"| Receptive penile-vaginal intercourse<sup>*</sup> | |||
| | 10<ref name=ESG /><ref name=Varghese /><ref name=Leynaert>{{ | |||
| cite journal | author=Leynaert B, Downs AM, de Vincenzi I | title=Heterosexual transmission of human immunodeficiency virus: variability of infectivity throughout the course of infection. European Study Group on Heterosexual Transmission of HIV | journal=Am. J. Epidemiol. | year=1998 | pages=88–96 | volume=148 | issue=1 | pmid=9663408 | |||
| }}</ref> | |||
| |- | |||
| ! style="text-align:left"| Insertive penile-vaginal intercourse<sup>*</sup> | |||
| | 5<ref name=ESG /><ref name=Varghese /> | |||
| |- | |||
| ! style="text-align:left"| Receptive oral intercourse<sup>*§</sup> | |||
| | 1<ref name=Varghese /> | |||
| |- | |||
| ! style="text-align:left"| Insertive oral intercourse<sup>*§</sup> | |||
| | 0.5<ref name=Varghese /> | |||
| |- bgcolor="#efefef" | |||
| ! colspan=5 style="border-right:0px;";| <sup>*</sup> assuming no condom use </br> <sup>§</sup> source refers to oral intercourse<br/>performed on a man | |||
| |} | |||
| Three main transmission routes for HIV have been identified. HIV-2 is transmitted much less frequently by the mother-to-child and sexual route than HIV-1. | |||
| ===Sexual=== | |||
| The majority of HIV infections are acquired through unprotected sexual relations. Sexual transmission can occur when infected sexual secretions of one partner come into contact with the ], ], or ] ] of another. | |||
| The correct and consistent use of ] ]s reduces the risk of sexual transmission of HIV by about 85%.<ref name="workshop">{{cite conference |last=National Institute of Allergy and Infectious Diseases | authorlink = National Institute of Allergy and Infectious Diseases | coauthors = National Institutes of Health, Department of Health and Human Services |title=Workshop Summary: Scientific Evidence on Condom Effectiveness for Sexually Transmitted Disease (STD) Prevention |pages=pp.13-15 |date=] |location=Hyatt Dulles Airport, Herndon, Virginia |url=http://www3.niaid.nih.gov/research/topics/STI/pdf/condomreport.pdf |format=PDF |accessdate=2007-04-07 }}</ref> However, ] may actually increase the male to female transmission rate due to inflammation of the vagina.<ref name="spermicide">{{cite web |url=http://www.fda.gov/oashi/aids/condom.html#should |title=Should spermicides be used with condoms? |accessdate=2006-10-23 |work=Condom Brochure, FDA OSHI HIV STDs }}</ref> | |||
| A meta-analysis of 27 observational studies conducted prior to 1999 in sub-Saharan Africa indicated that male ] reduces the risk of HIV infection.<ref>{{cite journal |last=Weiss |first=H.A. |authorlink= |coauthors=M.A. Quigley, R.J. Hayes |year=2000 |month= |title=Male circumcision and risk of HIV infection in sub-Saharan Africa: A systematic review and meta-analysis |journal=AIDS |volume=14 |issue=15 |pages=2361–70 |pmid=11089625 |quote=|doi=10.1097/00002030-200010200-00018 }}</ref> However, a subsequent review indicated that the correlation between circumcision and HIV in these observational studies may have been due to ].<ref name=Siegfred>{{cite journal | |||
| | author=Siegfried, N., Muller, M., Deeks, J., Volmink, J., Egger, M., Low, N., Walker, S. and Williamson, P. | title=HIV and male circumcision--a systematic review with assessment of the quality of studies | journal=Lancet Infect. Dis. | year=2005 | pages=165–73 | volume=5 | issue=3 | pmid=15766651}}</ref> Later trials, in which uncircumcised men were randomly assigned to be medically circumcised in sterile conditions and given counseling and other men were not circumcised, have been conducted in ],<ref name=Williams>{{cite journal | |||
| | author=Williams BG, Lloyd-Smith JO, Gouws E, Hankins C, Getz WM, Hargrove J, de Zoysa I, Dye C, Auvert B. | |||
| | title=The Potential Impact of Male Circumcision on HIV in Sub-Saharan Africa. | |||
| | journal=PLoS Med | year=2006 | pages=e262 | volume=3 | issue=7 | |||
| | pmid=16822094 | |||
| }}</ref> ]<ref>{{cite journal |author=Bailey RC, Moses S, Parker CB, ''et al'' |title=Male circumcision for HIV prevention in young men in Kisumu, Kenya: a randomised controlled trial |journal=Lancet |volume=369 |issue=9562 |pages=643–56 |year=2007 |pmid=17321310 |doi=10.1016/S0140-6736(07)60312-2}}</ref> and ]<ref>{{cite journal | |||
| | quotes = | |||
| | author = Gray RH et al | |||
| | date = 24 February 2007 | |||
| | year = 2007 | |||
| | month = February | |||
| | title = Male circumcision for HIV prevention in men in Rakai, Uganda: a randomised trial | |||
| | journal = Lancet | |||
| | volume = 369 | |||
| | issue = 9562 | |||
| | pages = 657–66 | |||
| | pmid = 17321311 | |||
| | doi = 10.1016/S0140-6736(07)60313-4 | |||
| | quote = | |||
| }}</ref> showing reductions in HIV transmission for ] sex of 60 percent, 53 percent, and 51 percent respectively. As a result, a panel of experts convened by WHO and the ] Secretariat has "recommended that male circumcision now be recognized as an additional important intervention to reduce the risk of heterosexually acquired HIV infection in men."<ref name=WHOUNAIDScircum>{{cite web | |||
| | author=WHO | publisher=WHO.int | year=2007 | |||
| | url=http://www.who.int/hiv/mediacentre/news68/en/index.html | |||
| | title=WHO and UNAIDS announce recommendations from expert consultation on male circumcision for HIV prevention | |||
| | accessdate=2007-07-13 | |||
| }}</ref> Research is clarifying whether there is a historical relationship between rates of male circumcision and rates of HIV in differing social and cultural contexts.{{Fact|date=October 2008}} | |||
| On the other hand, some South African medical experts have expressed concern that the repeated use of unsterilized blades in the ] of adolescent boys may actually be spreading HIV.<ref name=Kaisercircum>{{ | |||
| cite web | |||
| | author=Various | publisher=Kaisernetwork.org | year=2005 | |||
| | url=http://www.kaisernetwork.org/daily_reports/rep_index.cfm?DR_ID=31199 | |||
| | title=Repeated Use of Unsterilized Blades in Ritual Circumcision Might Contribute to HIV Spread in S. Africa, Doctors Say | |||
| | accessdate=2006-03-28 | |||
| }}</ref> | |||
| ===Blood or blood product=== | |||
| This transmission route can account for infections in ]rs, ]s and recipients of ]s (though most transfusions are checked for HIV in the developed world) and blood products. It is also of concern for persons receiving medical care in regions where there is prevalent substandard hygiene in the use of injection equipment, such as the reuse of needles in ] countries. ] workers such as nurses, laboratory workers, and doctors have also been infected, although this occurs more rarely. People who give and receive ]s, ], and ] procedures can also be at risk of infection. | |||
| ===Mother-to-child=== | |||
| The transmission of the virus from the mother to the child can occur '']'' during pregnancy and ''intrapartum'' at ]. In the absence of treatment, the transmission rate between the mother and child is around 25 percent.<ref name=Coovadia /> However, where combination ] drug treatment and ] are available, this risk can be reduced to as low as one percent.<ref name=Coovadia /> | |||
| ] also presents a risk of infection for the baby. | |||
| === Other routes === | |||
| HIV has been found at low concentrations in the ], ] and ] of infected individuals, but there are no recorded cases of infection by these secretions and the potential risk of transmission is negligible.<ref name="pmid2963151">{{cite journal | |||
| |author=Lifson AR | |||
| |title=Do alternate modes for transmission of human immunodeficiency virus exist? A review | |||
| |journal=JAMA | |||
| |volume=259 | |||
| |issue=9 | |||
| |pages=1353–6 | |||
| |year=1988 | |||
| |pmid=2963151 | |||
| |doi= | |||
| }}</ref> | |||
| === Multiple infection === | |||
| {{Main|HIV Superinfection}} | |||
| Unlike some other viruses, infection with HIV does not provide immunity against additional infections, particularly in the case of more genetically distant viruses. Both inter- and intra-clade multiple infections have been reported,<ref name='pmid15995957'>{{cite journal | |||
| |author=Smith D, Richman D, Little S | |||
| |title=HIV Superinfection | |||
| |journal=Journal of Infectious Diseases | |||
| |volume=192 | |||
| |pages=438–44 | |||
| |year=2005 | |||
| |pmid=15995957 | |||
| |doi=10.1086/431682 | |||
| }}</ref> and even associated with more rapid disease progression.<ref> | |||
| {{cite journal | |||
| |pmid=14987889 | |||
| |title=Dual HIV-1 infection associated with rapid disease progression | |||
| |author=Gottlieb, et al | |||
| |journal=Lancet | |||
| |year=2004 | |||
| |volume=363 | |||
| |issue=9049 | |||
| |pages=619–22 | |||
| |doi=10.1016/S0140-6736(04)15596-7 | |||
| }} | |||
| </ref> Multiple infections are divided into two categories depending on the timing of the acquisition of the second strain. ''Coinfection'' refers to two strains that appear to have been acquired at the same time (or too close to distinguish). ''Reinfection'' (or ''superinfection'') is infection with a second strain at a measurable time after the first. Both forms of dual infection have been reported for HIV in both acute and chronic infection around the world.<ref>{{cite journal | |||
| |url=http://jama.ama-assn.org/cgi/content/full/292/10/1177 | |||
| |pmid=15353529 | |||
| |title=Incidence of HIV superinfection following primary infection | |||
| |author=Smith et al | |||
| |journal=JAMA | |||
| |volume=292 | |||
| |issue=10 | |||
| |pages=1177–8 | |||
| |year=2004 | |||
| |doi=10.1001/jama.292.10.1177 | |||
| }}</ref><ref>{{cite journal | |||
| |author=Chohan B, Lavreys L, Rainwater SM, Overbaugh J |title=Evidence for frequent reinfection with human immunodeficiency virus type 1 of a different subtype |journal=J. Virol. |volume=79 |issue=16 |pages=10701–8 |year=2005 |month=Aug |pmid=16051862 |pmc=1182664 |doi=10.1128/JVI.79.16.10701-10708.2005 | |||
| }}</ref><ref>{{cite journal | |||
| |author=Piantadosi A, Chohan B, Chohan V, McClelland RS, Overbaugh J |title=Chronic HIV-1 infection frequently fails to protect against superinfection |journal=PLoS Pathog. |volume=3 |issue=11 |pages=e177 |year=2007 |month=Nov |pmid=18020705 |pmc=2077901 |doi=10.1371/journal.ppat.0030177 | |||
| }}</ref><ref> | |||
| {{cite journal | |||
| |author=Hu DJ, Subbarao S, Vanichseni S, ''et al'' |title=Frequency of HIV-1 dual subtype infections, including intersubtype superinfections, among injection drug users in Bangkok, Thailand |journal=AIDS |volume=19 |issue=3 |pages=303–8 |year=2005 |month=Feb |pmid=15718841 |doi= |url=http://meta.wkhealth.com/pt/pt-core/template-journal/lwwgateway/media/landingpage.htm?an=00002030-200502180-00009 | |||
| }} | |||
| </ref> | |||
| ==Structure and genome== | |||
| {{main|HIV structure and genome}} | |||
| ] | |||
| HIV is different in structure from other retroviruses. It is roughly spherical<ref name=McGovern>{{ | |||
| cite journal | author=McGovern SL, Caselli E, Grigorieff N, Shoichet BK | title=A common mechanism underlying promiscuous inhibitors from virtual and high-throughput screening | journal=J Med Chem | year=2002 | pages=1712–22 | volume=45 | issue=8 | |||
| | pmid=11931626 | |||
| }}</ref> | |||
| with a diameter of about 120 ], around 60 times smaller than a red blood cell, yet large for a virus.<ref name=Microbiology3> Compared with overview in: {{cite book |author=Fisher, Bruce; Harvey, Richard P.; Champe, Pamela C. |title=Lippincott's Illustrated Reviews: Microbiology (Lippincott's Illustrated Reviews Series) |publisher=Lippincott Williams & Wilkins |location=Hagerstown, MD |year= |pages= |isbn=0-7817-8215-5 |oclc= |doi=}} Page 3 </ref> It is composed of two copies of positive single-stranded ] that codes for the virus's nine ]s enclosed by a conical ] composed of 2,000 copies of the viral protein ].<ref name=compendia>{{ | |||
| cite book | |||
| | author = Various | |||
| | year = 2008 | |||
| | title = HIV Sequence Compendium 2008 Introduction | url = http://www.hiv.lanl.gov/content/sequence/HIV/COMPENDIUM/2008/frontmatter.pdf | |||
| | format= ] | |||
| }}</ref> The single-stranded RNA is tightly bound to nucleocapsid proteins, p7 and enzymes needed for the development of the virion such as ], ], ] and ]. A matrix composed of the viral protein p17 surrounds the capsid ensuring the integrity of the virion particle.<ref name=compendia/> This is, in turn, surrounded by the viral envelope which is composed of two layers of fatty molecules called ]s taken from the membrane of a human cell when a newly formed virus particle buds from the cell. Embedded in the viral envelope are proteins from the host cell and about 70 copies of a complex HIV protein that protrudes through the surface of the virus particle.<ref name=compendia/> This protein, known as Env, consists of a cap made of three molecules called ], and a stem consisting of three ] molecules that anchor the structure into the viral envelope.<ref name=Chan>{{ | |||
| This is, in turn, surrounded by the ], that is composed of the ] taken from the membrane of a human host cell when the newly formed virus particle buds from the cell. The viral envelope contains proteins from the host cell and relatively few copies of the HIV envelope protein,<ref name=compendia /> which consists of a cap made of three molecules known as ], and a stem consisting of three ] molecules that anchor the structure into the viral envelope.<ref name=Chan>{{cite journal | vauthors = Chan DC, Fass D, Berger JM, Kim PS | title = Core structure of gp41 from the HIV envelope glycoprotein | journal = Cell | volume = 89 | issue = 2 | pages = 263–73 | date = April 1997 | pmid = 9108481 | doi = 10.1016/S0092-8674(00)80205-6 | url = http://www.its.caltech.edu/~chanlab/PDFs/Chan_Cell_1997.pdf | s2cid = 4518241 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Klein JS, Bjorkman PJ | title = Few and far between: how HIV may be evading antibody avidity | journal = PLOS Pathogens | volume = 6 | issue = 5 | pages = e1000908 | date = May 2010 | pmid = 20523901 | pmc = 2877745 | doi = 10.1371/journal.ppat.1000908 | doi-access = free }}</ref> The envelope protein, encoded by the HIV ] gene, allows the virus to attach to target cells and fuse the viral envelope with the target ] releasing the viral contents into the cell and initiating the infectious cycle.<ref name=Chan /> | |||
| cite journal | |||
| | author=Chan, DC., Fass, D., Berger, JM., Kim, PS. | title=Core Structure of gp41 from the HIV Envelope Glycoprotein | journal=Cell | year=1997 | pages=263–73 | volume=89 | pmid=9108481 |format=pdf |url=http://www.its.caltech.edu/~chanlab/PDFs/Chan_Cell_1997.pdf | |||
| ] | |||
| }}</ref> This glycoprotein complex enables the virus to attach to and fuse with target cells to initiate the infectious cycle.<ref name=Chan/> | |||
| As the sole viral protein on the surface of the virus, the envelope protein is a major target for ] efforts.<ref name="nih1998">{{cite press release | author=National Institute of Health | title=Crystal structure of key HIV protein reveals new prevention, treatment targets | date=June 17, 1998 |url=http://www3.niaid.nih.gov/news/newsreleases/1998/hivprotein.htm | access-date = September 14, 2006 |archive-url=https://web.archive.org/web/20060219112450/http://www3.niaid.nih.gov/news/newsreleases/1998/hivprotein.htm |archive-date=February 19, 2006}}</ref> Over half of the mass of the trimeric envelope spike is N-linked ]s. The density is high as the glycans shield the underlying viral protein from neutralisation by antibodies. This is one of the most densely glycosylated molecules known and the density is sufficiently high to prevent the normal maturation process of glycans during biogenesis in the endoplasmic and Golgi apparatus.<ref>{{cite journal | vauthors = Behrens AJ, Vasiljevic S, Pritchard LK, Harvey DJ, Andev RS, Krumm SA, Struwe WB, Cupo A, Kumar A, Zitzmann N, Seabright GE, Kramer HB, Spencer DI, Royle L, Lee JH, Klasse PJ, Burton DR, Wilson IA, Ward AB, Sanders RW, Moore JP, Doores KJ, Crispin M | display-authors = 6 | title = Composition and Antigenic Effects of Individual Glycan Sites of a Trimeric HIV-1 Envelope Glycoprotein | journal = Cell Reports | volume = 14 | issue = 11 | pages = 2695–706 | date = March 2016 | pmid = 26972002 | pmc = 4805854 | doi = 10.1016/j.celrep.2016.02.058 }}</ref><ref>{{cite journal | vauthors = Pritchard LK, Spencer DI, Royle L, Bonomelli C, Seabright GE, Behrens AJ, Kulp DW, Menis S, Krumm SA, Dunlop DC, Crispin DJ, Bowden TA, Scanlan CN, Ward AB, Schief WR, Doores KJ, Crispin M | display-authors = 6 | title = Glycan clustering stabilizes the mannose patch of HIV-1 and preserves vulnerability to broadly neutralizing antibodies | journal = Nature Communications | volume = 6 | pages = 7479 | date = June 2015 | pmid = 26105115 | pmc = 4500839 | doi = 10.1038/ncomms8479 | bibcode = 2015NatCo...6.7479P }}</ref> The majority of the glycans are therefore stalled as immature 'high-mannose' glycans not normally present on human glycoproteins that are secreted or present on a cell surface.<ref>{{cite journal | vauthors = Pritchard LK, Harvey DJ, Bonomelli C, Crispin M, Doores KJ | title = Cell- and Protein-Directed Glycosylation of Native Cleaved HIV-1 Envelope | journal = Journal of Virology | volume = 89 | issue = 17 | pages = 8932–44 | date = September 2015 | pmid = 26085151 | pmc = 4524065 | doi = 10.1128/JVI.01190-15 }}</ref> The unusual processing and high density means that almost all broadly neutralising antibodies that have so far been identified (from a subset of patients that have been infected for many months to years) bind to, or are adapted to cope with, these envelope glycans.<ref>{{cite journal | vauthors = Crispin M, Doores KJ | title = Targeting host-derived glycans on enveloped viruses for antibody-based vaccine design | journal = Current Opinion in Virology | volume = 11 | pages = 63–9 | date = April 2015 | pmid = 25747313 | pmc = 4827424 | doi = 10.1016/j.coviro.2015.02.002 | author-link2 = Katie Doores }}</ref> | |||
| Both these surface proteins, especially gp120, have been considered as targets of future treatments or vaccines against HIV.<ref name=nih1998>{{ | |||
| The molecular structure of the viral spike has now been determined by ]<ref>{{cite journal | vauthors = Julien JP, Cupo A, Sok D, Stanfield RL, Lyumkis D, Deller MC, Klasse PJ, Burton DR, Sanders RW, Moore JP, Ward AB, Wilson IA | display-authors = 6 | title = Crystal structure of a soluble cleaved HIV-1 envelope trimer | journal = Science | volume = 342 | issue = 6165 | pages = 1477–83 | date = December 2013 | pmid = 24179159 | pmc = 3886632 | doi = 10.1126/science.1245625 | bibcode = 2013Sci...342.1477J }}</ref> and ].<ref>{{cite journal | vauthors = Lyumkis D, Julien JP, de Val N, Cupo A, Potter CS, Klasse PJ, Burton DR, Sanders RW, Moore JP, Carragher B, Wilson IA, Ward AB | display-authors = 6 | title = Cryo-EM structure of a fully glycosylated soluble cleaved HIV-1 envelope trimer | journal = Science | volume = 342 | issue = 6165 | pages = 1484–90 | date = December 2013 | pmid = 24179160 | pmc = 3954647 | doi = 10.1126/science.1245627 | bibcode = 2013Sci...342.1484L }}</ref> These advances in structural biology were made possible due to the development of stable ] forms of the viral spike by the introduction of an intersubunit ] and an ] to ] ] (] of an amino acid) in gp41.<ref>{{cite journal | vauthors = Sanders RW, Derking R, Cupo A, Julien JP, Yasmeen A, de Val N, Kim HJ, Blattner C, de la Peña AT, Korzun J, Golabek M, de Los Reyes K, Ketas TJ, van Gils MJ, King CR, Wilson IA, Ward AB, Klasse PJ, Moore JP | display-authors = 6 | title = A next-generation cleaved, soluble HIV-1 Env trimer, BG505 SOSIP.664 gp140, expresses multiple epitopes for broadly neutralizing but not non-neutralizing antibodies | journal = PLOS Pathogens | volume = 9 | issue = 9 | pages = e1003618 | date = September 2013 | pmid = 24068931 | pmc = 3777863 | doi = 10.1371/journal.ppat.1003618 | doi-access = free }}</ref> The so-called SOSIP ] not only reproduce the antigenic properties of the native viral spike, but also display the same degree of immature glycans as presented on the native virus.<ref>{{cite journal | vauthors = Pritchard LK, Vasiljevic S, Ozorowski G, Seabright GE, Cupo A, Ringe R, Kim HJ, Sanders RW, Doores KJ, Burton DR, Wilson IA, Ward AB, Moore JP, Crispin M | display-authors = 6 | title = Structural Constraints Determine the Glycosylation of HIV-1 Envelope Trimers | journal = Cell Reports | volume = 11 | issue = 10 | pages = 1604–13 | date = June 2015 | pmid = 26051934 | pmc = 4555872 | doi = 10.1016/j.celrep.2015.05.017 }}</ref> Recombinant trimeric viral spikes are promising vaccine candidates as they display less non-neutralising ]s than recombinant monomeric gp120, which act to suppress the immune response to target epitopes.<ref>{{cite journal | vauthors = de Taeye SW, Ozorowski G, Torrents de la Peña A, Guttman M, Julien JP, van den Kerkhof TL, Burger JA, Pritchard LK, Pugach P, Yasmeen A, Crampton J, Hu J, Bontjer I, Torres JL, Arendt H, DeStefano J, Koff WC, Schuitemaker H, Eggink D, Berkhout B, Dean H, LaBranche C, Crotty S, Crispin M, Montefiori DC, Klasse PJ, Lee KK, Moore JP, Wilson IA, Ward AB, Sanders RW | display-authors = 6 | title = Immunogenicity of Stabilized HIV-1 Envelope Trimers with Reduced Exposure of Non-neutralizing Epitopes | journal = Cell | volume = 163 | issue = 7 | pages = 1702–15 | date = December 2015 | pmid = 26687358 | pmc = 4732737 | doi = 10.1016/j.cell.2015.11.056 }}</ref> | |||
| cite news | |||
| ] | |||
| | author=National Institute of Health | title=Crystal Structure of Key HIV Protein Reveals New Prevention, Treatment Targets | date=June 17, 1998 |url=http://www3.niaid.nih.gov/news/newsreleases/1998/hivprotein.htm | accessdate = 2006-09-14 | |||
| The RNA genome consists of at least seven structural landmarks (], ], ], PE, SLIP, CRS, and INS), and nine genes (''gag'', ''pol'', and ''env'', ''tat'', ''rev'', ''nef'', ''vif'', ''vpr'', ''vpu'', and sometimes a tenth ''tev'', which is a fusion of ''tat'', ''env'' and ''rev''), encoding 19 proteins. Three of these genes, ''gag'', ''pol'', and ''env'', contain information needed to make the structural proteins for new virus particles.<ref name=compendia /> For example, ''env'' codes for a protein called gp160 that is cut in two by a cellular protease to form gp120 and gp41. The six remaining genes, ''tat'', ''rev'', ''nef'', ''vif'', ''vpr'', and ''vpu'' (or ''vpx'' in the case of HIV-2), are regulatory genes for proteins that control the ability of HIV to infect cells, produce new copies of virus (replicate), or cause disease.<ref name=compendia /> | |||
| The two '']'' proteins (p16 and p14) are ] for the LTR ] acting by binding the TAR RNA element. The TAR may also be processed into ]s that regulate the ] genes '']'' and '']''.<ref name="pmid18299284">{{cite journal | vauthors = Ouellet DL, Plante I, Landry P, Barat C, Janelle ME, Flamand L, Tremblay MJ, Provost P | title = Identification of functional microRNAs released through asymmetrical processing of HIV-1 TAR element | journal = Nucleic Acids Research | volume = 36 | issue = 7 | pages = 2353–65 | date = April 2008 | pmid = 18299284 | pmc = 2367715 | doi = 10.1093/nar/gkn076 }}</ref><ref name="pmid19220914">{{cite journal | vauthors = Klase Z, Winograd R, Davis J, Carpio L, Hildreth R, Heydarian M, Fu S, McCaffrey T, Meiri E, Ayash-Rashkovsky M, Gilad S, Bentwich Z, Kashanchi F | title = HIV-1 TAR miRNA protects against apoptosis by altering cellular gene expression | journal = Retrovirology | volume = 6 | issue = 1 | pages = 18 | year = 2009 | pmid = 19220914 | pmc = 2654423 | doi = 10.1186/1742-4690-6-18 | doi-access = free }}</ref> The ] protein (p19) is involved in shuttling RNAs from the nucleus and the cytoplasm by binding to the ] RNA element. The ''vif'' protein (p23) prevents the action of ] (a cellular protein that ] ] to ] in the single-stranded viral DNA and/or interferes with reverse transcription<ref>{{cite journal | vauthors = Vasudevan AA, Smits SH, Höppner A, Häussinger D, Koenig BW, Münk C | title = Structural features of antiviral DNA cytidine deaminases | journal = ] | volume = 394 | issue = 11 | pages = 1357–70 | date = Nov 2013 | pmid = 23787464 | doi = 10.1515/hsz-2013-0165 | s2cid = 4151961 | url = http://juser.fz-juelich.de/search?p=id:%22FZJ-2013-05757%22 | type = Submitted manuscript }}</ref>). The '']'' protein (p14) arrests ] at ]. The ''nef'' protein (p27) down-regulates ] (the major viral receptor), as well as the ] and ] molecules.<ref name="pmid2014052">{{cite journal | vauthors = Garcia JV, Miller AD | title = Serine phosphorylation-independent downregulation of cell-surface CD4 by nef | journal = Nature | volume = 350 | issue = 6318 | pages = 508–11 | date = April 1991 | pmid = 2014052 | doi = 10.1038/350508a0 | bibcode = 1991Natur.350..508G | s2cid = 1628392 }}</ref><ref name="pmid8612235">{{cite journal | vauthors = Schwartz O, Maréchal V, Le Gall S, Lemonnier F, Heard JM | title = Endocytosis of major histocompatibility complex class I molecules is induced by the HIV-1 Nef protein | journal = Nature Medicine | volume = 2 | issue = 3 | pages = 338–42 | date = March 1996 | pmid = 8612235 | doi = 10.1038/nm0396-338 | s2cid = 7461342 }}</ref><ref name="pmid11593029">{{cite journal | vauthors = Stumptner-Cuvelette P, Morchoisne S, Dugast M, Le Gall S, Raposo G, Schwartz O, Benaroch P | title = HIV-1 Nef impairs MHC class II antigen presentation and surface expression | journal = Proceedings of the National Academy of Sciences of the United States of America | volume = 98 | issue = 21 | pages = 12144–9 | date = October 2001 | pmid = 11593029 | pmc = 59782 | doi = 10.1073/pnas.221256498 | bibcode = 2001PNAS...9812144S | doi-access = free }}</ref> | |||
| }}</ref> | |||
| ''Nef'' also interacts with ]s. The ''vpu'' protein (p16) influences the release of new virus particles from infected cells.<ref name=compendia /> The ends of each strand of HIV RNA contain an RNA sequence called a ] (LTR). Regions in the LTR act as switches to control production of new viruses and can be triggered by proteins from either HIV or the host cell. The ] is involved in viral genome packaging and recognized by ] and ] proteins. The SLIP element ({{DNA sequence|TTTTTT}}) is involved in the ] in the ''gag''-''pol'' ] required to make functional ''pol''.<ref name=compendia /> | |||
| The RNA genome consists of at least 7 structural landmarks (LTR, TAR, RRE, PE, SLIP, CRS, INS) and nine genes (''gag'', ''pol'', and ''env'', ''tat'', ''rev'', ''nef'', ''vif'', ''vpr'', ''vpu'', and ''tev'') encoding 19 proteins. Three of these genes, ''gag'', ''pol'', and ''env'', contain information needed to make the structural proteins for new virus particles.<ref name=compendia/> For example, ''env'' codes for a protein called gp160 that is broken down by a viral enzyme to form gp120 and gp41. The six remaining genes, ''tat'', ''rev'', ''nef'', ''vif'', ''vpr'', and ''vpu'' (or ''vpx'' in the case of HIV-2), are regulatory genes for proteins that control the ability of HIV to infect cells, produce new copies of virus (replicate), or cause disease.<ref name=compendia/> The two Tat proteins (p16 and p14) are ] for the LTR promoter acting by binding the TAR RNA element. The ] protein (p19) is involved in shuttling RNAs from the nucleus and the cytoplasm by binding to the RRE RNA element. The Vif protein (p23) prevents the action of ] (a cell protein which deaminates DNA:RNA hybrids and/or interferes with the Pol protein). The Vpr protein (p14) arrests cell division at G2/M. The Nef protein (p27) downregulates ] (the major viral receptor), as well as the ] and ] molecules.<ref name="pmid2014052">{{cite journal |author=Garcia JV, Miller AD |title=Serine phosphorylation-independent downregulation of cell-surface CD4 by nef |journal=Nature |volume=350 |issue=6318 |pages=508-11 |year=1991 |month=April |pmid=2014052 |doi=10.1038/350508a0 |url=}}</ref><ref name="pmid8612235">{{cite journal |author=Schwartz O, Maréchal V, Le Gall S, Lemonnier F, Heard JM |title=Endocytosis of major histocompatibility complex class I molecules is induced by the HIV-1 Nef protein |journal=Nat. Med. |volume=2 |issue=3 |pages=338-42 |year=1996 |month=March |pmid=8612235 |doi= |url=}}</ref><ref name="pmid11593029">{{cite journal |author=Stumptner-Cuvelette P, Morchoisne S, Dugast M, ''et al'' |title=HIV-1 Nef impairs MHC class II antigen presentation and surface expression |journal=Proc. Natl. Acad. Sci. U.S.A. |volume=98 |issue=21 |pages=12144-9 |year=2001 |month=October |pmid=11593029 |pmc=59782 |doi=10.1073/pnas.221256498 |url=}}</ref> Nef also interacts with SH3 domains. The Vpu protein (p16) influences the release of new virus particles from infected cells.<ref name=compendia/> The ends of each strand of HIV RNA contain an RNA sequence called the ] (LTR). Regions in the LTR act as switches to control production of new viruses and can be triggered by proteins from either HIV or the host cell. The ] is involved in viral genome packaging and recognized by Gag and Rev proteins. The SLIP element (TTTTTT) is involved in the frameshift in the Gag-Pol reading frame required to make functional Pol.<ref name=compendia/> | |||
| ==Tropism== | ===Tropism=== | ||
| {{Main|HIV tropism}} | {{Main|HIV tropism}} | ||
| ] | |||
| The term ] refers to which cell types HIV infects. HIV can infect a variety of immune cells such as ], ]s, and ]s. HIV-1 entry to macrophages and CD4<SUP>+</SUP> T cells is mediated through interaction of the virion envelope glycoproteins (gp120) with the CD4 molecule on the target cells and also with ] coreceptors.<ref name=Chan/> | |||
| The term ] refers to the cell types a virus infects. HIV can infect a variety of immune cells such as ], ]s, and ]s. HIV-1 entry to macrophages and CD4<SUP>+</SUP> T cells is mediated through interaction of the virion envelope glycoproteins (gp120) with the CD4 molecule on the target cells' membrane and also with ] ]s.<ref name=Chan /><ref>{{cite journal | vauthors = Arrildt KT, Joseph SB, Swanstrom R | title = The HIV-1 env protein: a coat of many colors | journal = Current HIV/AIDS Reports | volume = 9 | issue = 1 | pages = 52–63 | date = March 2012 | pmid = 22237899 | pmc = 3658113 | doi = 10.1007/s11904-011-0107-3 }}</ref> | |||
| Macrophage-tropic (M-tropic) strains of HIV-1, or non-]-inducing strains (NSI; now called R5 viruses<ref name="pmid9440686">{{cite journal | vauthors = Berger EA, Doms RW, Fenyö EM, Korber BT, Littman DR, Moore JP, Sattentau QJ, Schuitemaker H, Sodroski J, Weiss RA | title = A new classification for HIV-1 | journal = Nature | volume = 391 | issue = 6664 | pages = 240 | year = 1998 | pmid = 9440686 | doi = 10.1038/34571 | bibcode = 1998Natur.391..240B | s2cid = 2159146 | doi-access = free }}</ref>) use the ''β''-chemokine receptor, ], for entry and are thus able to replicate in both macrophages and CD4<SUP>+</SUP> T cells.<ref name=Coakley>{{cite journal | vauthors = Coakley E, Petropoulos CJ, Whitcomb JM | title = Assessing ch vbgemokine co-receptor usage in HIV | journal = Current Opinion in Infectious Diseases | volume = 18 | issue = 1 | pages = 9–15 | year = 2005 | pmid = 15647694 | doi = 10.1097/00001432-200502000-00003 | s2cid = 30923492 }}</ref> This CCR5 co-receptor is used by almost all primary HIV-1 isolates regardless of viral genetic subtype. Indeed, macrophages play a key role in several critical aspects of HIV infection. They appear to be the first cells infected by HIV and perhaps the source of HIV production when CD4<SUP>+</SUP> cells become depleted in the patient. Macrophages and microglial cells are the cells infected by HIV in the ]. In the ]s and ] of HIV-infected patients, macrophages fuse into multinucleated ]s that produce huge amounts of virus. | |||
| Macrophage (M-tropic) strains of HIV-1, or non-]-inducing strains (NSI) use the ''β''-chemokine receptor ] for entry and are thus able to replicate in macrophages and CD4<SUP>+</SUP> T cells.<ref name=Coakley>{{ | |||
| T-tropic strains of HIV-1, or ]-inducing strains (SI; now called X4 viruses<ref name="pmid9440686" />) replicate in primary CD4<SUP>+</SUP> T cells as well as in macrophages and use the ''α''-chemokine receptor, ], for entry.<ref name=Coakley /><ref name=Deng> | |||
| cite journal | |||
| | author=Coakley, E., Petropoulos, C. J. and Whitcomb, J. M. | title=Assessing ch vbgemokine co-receptor usage in HIV | journal=Curr. Opin. Infect. Dis. | year=2005 | pages=9–15 | volume=18 | issue=1 | pmid=15647694 |format= | |||
| }}</ref> This CCR5 coreceptor is used by almost all primary HIV-1 isolates regardless of viral genetic subtype. Indeed, macrophages play a key role in several critical aspects of HIV infection. They appear to be the first cells infected by HIV and perhaps the source of HIV production when CD4<SUP>+</SUP> cells become depleted in the patient. Macrophages and microglial cells are the cells infected by HIV in the ]. In tonsils and ] of HIV-infected patients, macrophages fuse into multinucleated giant cells that produce huge amounts of virus. | |||
| {{cite journal | vauthors = Deng H, Liu R, Ellmeier W, Choe S, Unutmaz D, Burkhart M, Di Marzio P, Marmon S, Sutton RE, Hill CM, Davis CB, Peiper SC, Schall TJ, Littman DR, Landau NR | title = Identification of a major co-receptor for primary isolates of HIV-1 | journal = Nature | volume = 381 | issue = 6584 | pages = 661–6 | year = 1996 | pmid = 8649511 | doi = 10.1038/381661a0 | bibcode = 1996Natur.381..661D | s2cid = 37973935 }}</ref><ref name=Feng> | |||
| T-tropic isolates, or ]-inducing (SI) strains replicate in primary CD4<SUP>+</SUP> T cells as well as in macrophages and use the ''α''-chemokine receptor, ], for entry.<ref name=Coakley /><ref name=Deng> | |||
| {{cite journal | vauthors = Feng Y, Broder CC, Kennedy PE, Berger EA | title = HIV-1 entry cofactor: functional cDNA cloning of a seven-transmembrane, G protein-coupled receptor | journal = Science | volume = 272 | issue = 5263 | pages = 872–7 | year = 1996 | pmid = 8629022 | doi = 10.1126/science.272.5263.872 | bibcode = 1996Sci...272..872F | s2cid = 44455027 | pmc = 3412311 }}</ref> | |||
| {{cite journal | |||
| | author=Deng H, Liu R, Ellmeier W, Choe S, Unutmaz D, Burkhart M, Di Marzio P, Marmon S, Sutton RE, Hill CM, Davis CB, Peiper SC, Schall TJ, Littman DR, Landau NR. | title=Identification of a major co-receptor for primary isolates of HIV-1 | journal=Nature | year=1996 | pages=661–6 | volume=381 | issue=6584 | pmid=8649511 | doi=10.1038/381661a0 | |||
| Dual-tropic HIV-1 strains are thought to be transitional strains of HIV-1 and thus are able to use both CCR5 and CXCR4 as co-receptors for viral entry. | |||
| }}</ref><ref name=Feng> | |||
| The ''α''-chemokine ], a ] for CXCR4, suppresses replication of T-tropic HIV-1 isolates. It does this by ] the expression of CXCR4 on the surface of HIV target cells. M-tropic HIV-1 isolates that use only the CCR5 receptor are termed R5; those that use only CXCR4 are termed X4, and those that use both, X4R5. However, the use of co-receptors alone does not explain viral tropism, as not all R5 viruses are able to use CCR5 on macrophages for a productive infection<ref name="Coakley" /> and HIV can also infect a subtype of ],<ref name="Knight">{{cite journal | vauthors = Knight SC, Macatonia SE, Patterson S | title = HIV I infection of dendritic cells | journal = ] | volume = 6 | issue = 2–3 | pages = 163–75 | year = 1990 | pmid = 2152500 | doi = 10.3109/08830189009056627 }}</ref> which probably constitute a ] that maintains infection when CD4<SUP>+</SUP> T cell numbers have declined to extremely low levels. | |||
| {{cite journal | |||
| | author=Feng Y, Broder CC, Kennedy PE, Berger EA. | title=HIV-1 entry cofactor: functional cDNA cloning of a seven-transmembrane, G protein-coupled receptor | journal=Science | year=1996 | pages=872–7 | volume=272 | issue=5263 | pmid=8629022 | doi=10.1126/science.272.5263.872 | |||
| Some people are resistant to certain strains of HIV.<ref name="Tang">{{cite journal | vauthors = Tang J, Kaslow RA | title = The impact of host genetics on HIV infection and disease progression in the era of highly active antiretroviral therapy | journal = AIDS | volume = 17 | issue = Suppl 4 | pages = S51–S60 | year = 2003 | pmid = 15080180 | doi = 10.1097/00002030-200317004-00006 | doi-access = free }}</ref> For example, people with the ] mutation are resistant to infection by the R5 virus, as the mutation leaves HIV unable to bind to this co-receptor, reducing its ability to infect target cells. | |||
| }}</ref> Dual-tropic HIV-1 strains are thought to be transitional strains of the HIV-1 virus and thus are able to use both CCR5 and CXCR4 as co-receptors for viral entry. | |||
| ] is the major mode of HIV transmission. Both X4 and R5 HIV are present in the ], which enables the virus to be transmitted from a male to his ]. The virions can then infect numerous cellular targets and disseminate into the whole organism. However, a selection process{{Explain|reason=explain the selection process|date=August 2018}} leads to a predominant transmission of the R5 virus through this pathway.<ref name="Zhu1993">{{cite journal | vauthors = Zhu T, Mo H, Wang N, Nam DS, Cao Y, Koup RA, Ho DD | title = Genotypic and phenotypic characterization of HIV-1 patients with primary infection | journal = Science | volume = 261 | issue = 5125 | pages = 1179–81 | year = 1993 | pmid = 8356453 | doi = 10.1126/science.8356453 | bibcode = 1993Sci...261.1179Z }}</ref><ref name="Wout">{{cite journal | vauthors = van't Wout AB, Kootstra NA, Mulder-Kampinga GA, Albrecht-van Lent N, Scherpbier HJ, Veenstra J, Boer K, Coutinho RA, Miedema F, Schuitemaker H | title = Macrophage-tropic variants initiate human immunodeficiency virus type 1 infection after sexual, parenteral, and vertical transmission | journal = Journal of Clinical Investigation | volume = 94 | issue = 5 | pages = 2060–7 | year = 1994 | pmid = 7962552 | pmc = 294642 | doi = 10.1172/JCI117560 }}</ref><ref name="Zhu1996">{{cite journal | vauthors = Zhu T, Wang N, Carr A, Nam DS, Moor-Jankowski R, Cooper DA, Ho DD | title = Genetic characterization of human immunodeficiency virus type 1 in blood and genital secretions: evidence for viral compartmentalization and selection during sexual transmission | journal = Journal of Virology | volume = 70 | issue = 5 | pages = 3098–107 | year = 1996 | pmid = 8627789 | pmc = 190172 | doi = 10.1128/JVI.70.5.3098-3107.1996 }}</ref> In patients infected with subtype B HIV-1, there is often a co-receptor switch in late-stage disease and T-tropic variants that can infect a variety of T cells through CXCR4.<ref name="Clevestig">{{cite journal | vauthors = Clevestig P, Maljkovic I, Casper C, Carlenor E, Lindgren S, Navér L, Bohlin AB, Fenyö EM, Leitner T, Ehrnst A | title = The X4 phenotype of HIV type 1 evolves from R5 in two children of mothers, carrying X4, and is not linked to transmission | journal = AIDS Research and Human Retroviruses | volume = 21 | issue = 5 | pages = 371–8 | year = 2005 | pmid = 15929699 | doi = 10.1089/aid.2005.21.371 }}</ref> These variants then replicate more aggressively with heightened virulence that causes rapid T cell depletion, immune system collapse, and opportunistic infections that mark the advent of AIDS.<ref name="Moore">{{cite journal | vauthors = Moore JP | title = Coreceptors: implications for HIV pathogenesis and therapy | journal = Science | volume = 276 | issue = 5309 | pages = 51–2 | year = 1997 | pmid = 9122710 | doi = 10.1126/science.276.5309.51 | s2cid = 33262844 }}</ref> HIV-positive patients acquire an enormously broad spectrum of opportunistic infections, which was particularly problematic prior to the onset of ] therapies; however, the same infections are reported among HIV-infected patients examined post-mortem following the onset of antiretroviral therapies.<ref name="pmid27611681"/> Thus, during the course of infection, viral adaptation to the use of CXCR4 instead of CCR5 may be a key step in the progression to AIDS. A number of studies with subtype B-infected individuals have determined that between 40 and 50 percent of AIDS patients can harbour viruses of the SI and, it is presumed, the X4 phenotypes.<ref name="Karlsson">{{cite journal | vauthors = Karlsson A, Parsmyr K, Aperia K, Sandström E, Fenyö EM, Albert J | title = MT-2 cell tropism of human immunodeficiency virus type 1 isolates as a marker for response to treatment and development of drug resistance | journal = The Journal of Infectious Diseases | volume = 170 | issue = 6 | pages = 1367–75 | year = 1994 | pmid = 7995974 | doi = 10.1093/infdis/170.6.1367 }}</ref><ref name="Koot">{{cite journal | vauthors = Koot M, van 't Wout AB, Kootstra NA, de Goede RE, Tersmette M, Schuitemaker H | title = Relation between changes in cellular load, evolution of viral phenotype, and the clonal composition of virus populations in the course of human immunodeficiency virus type 1 infection | journal = The Journal of Infectious Diseases | volume = 173 | issue = 2 | pages = 349–54 | year = 1996 | pmid = 8568295 | doi = 10.1093/infdis/173.2.349 | doi-access = free }}</ref> | |||
| The ''α''-chemokine, SDF-1, a ligand for CXCR4, suppresses replication of T-tropic HIV-1 isolates. It does this by down-regulating the expression of CXCR4 on the surface of these cells. HIV that use only the CCR5 receptor are termed ], those that only use CXCR4 are termed ], and those that use both, X4R5. However, the use of coreceptor alone does not explain viral tropism, as not all R5 viruses are able to use CCR5 on macrophages for a productive infection<ref name=Coakley /> and HIV can also infect a subtype of ],<ref name=Knight> | |||
| HIV-2 is much less pathogenic than HIV-1 and is restricted in its worldwide distribution to ]. The adoption of "accessory genes" by HIV-2 and its more ] pattern of co-receptor usage (including CD4-independence) may assist the virus in its adaptation to avoid innate restriction factors present in host cells. Adaptation to use normal cellular machinery to enable transmission and productive infection has also aided the establishment of HIV-2 replication in humans. A survival strategy for any infectious agent is not to kill its host, but ultimately become a ] organism. Having achieved a low pathogenicity, over time, variants that are more successful at transmission will be selected.<ref name="CheneyandMcKnight">{{cite book |vauthors=Cheney K, McKnight A |chapter=HIV-2 Tropism and Disease | year=2010 |title=Lentiviruses and Macrophages: Molecular and Cellular Interactions | publisher=] | isbn=978-1-904455-60-8 }}{{page needed|date=December 2017}}</ref> | |||
| {{cite journal | |||
| | author=Knight, S. C., Macatonia, S. E. and Patterson, S. | title=HIV I infection of dendritic cells | journal=Int. Rev. Immunol. | year=1990 | pages=163–75 | volume=6 | issue=2-3 | pmid=2152500 | doi=10.3109/08830189009056627 | |||
| ===Replication cycle=== | |||
| }}</ref> which probably constitute a reservoir that maintains infection when CD4<SUP>+</SUP> T cell numbers have declined to extremely low levels. | |||
| ] | |||
| ====Entry to the cell==== | |||
| Some people are resistant to certain strains of HIV.<ref name=Tang>{{ | |||
| ] | |||
| The HIV virion enters ]s and CD4<SUP>+</SUP> ] by the ] of ]s on its surface to receptors on the target cell followed by fusion of the ] with the target cell membrane and the release of the HIV capsid into the cell.<ref name=Chan2>{{cite journal | vauthors = Chan DC, Kim PS | title = HIV entry and its inhibition | journal = Cell | volume = 93 | issue = 5 | pages = 681–4 | year = 1998 | pmid = 9630213 | doi = 10.1016/S0092-8674(00)81430-0 | s2cid = 10544941 | doi-access = free }}</ref><ref name=Wyatt>{{cite journal | vauthors = Wyatt R, Sodroski J | title = The HIV-1 envelope glycoproteins: fusogens, antigens, and immunogens | journal = Science | volume = 280 | issue = 5371 | pages = 1884–8 | year = 1998 | pmid = 9632381 | doi = 10.1126/science.280.5371.1884 | bibcode = 1998Sci...280.1884W }}</ref> | |||
| cite journal | |||
| | author=Tang, J. and Kaslow, R. A. | |||
| | title=The impact of host genetics on HIV infection and disease progression in the era of highly active antiretroviral therapy | |||
| | journal=AIDS | year=2003 | pages=S51–S60 | volume=17 | issue=Suppl 4 | |||
| | pmid=15080180 | |||
| Entry to the cell begins through interaction of the trimeric envelope complex (] spike) on the HIV viral envelope and both ] and a chemokine co-receptor (generally either ] or ], but others are known to interact) on the target cell surface.<ref name=Chan2 /><ref name=Wyatt /> Gp120 binds to ] α<sub>4</sub>β<sub>7</sub> activating ], the central integrin involved in the establishment of ]s, which facilitate efficient cell-to-cell spreading of HIV-1.<ref name=Arthos>{{cite journal | vauthors = Arthos J, Cicala C, Martinelli E, Macleod K, Van Ryk D, Wei D, Xiao Z, Veenstra TD, Conrad TP, Lempicki RA, McLaughlin S, Pascuccio M, Gopaul R, McNally J, Cruz CC, Censoplano N, Chung E, Reitano KN, Kottilil S, Goode DJ, Fauci AS | title = HIV-1 envelope protein binds to and signals through integrin alpha(4)beta(7), the gut mucosal homing receptor for peripheral T cells | journal = Nature Immunology | volume = 9| issue = 3 | pages = 301–9 | year = 2008 | pmid = 18264102 | doi = 10.1038/ni1566 | s2cid = 205361178 }}</ref> The gp160 spike contains binding domains for both CD4 and chemokine receptors.<ref name=Chan2 /><ref name=Wyatt /> | |||
| }}</ref> One example of how this occurs is people with the ] mutation; these people are resistant to infection with R5 virus as the mutation stops HIV from binding to this coreceptor, reducing its ability to infect target cells. | |||
| The first step in fusion involves the high-affinity attachment of the CD4 binding domains of ] to CD4. Once gp120 is bound with the CD4 protein, the envelope complex undergoes a structural change, exposing the chemokine receptor binding domains of gp120 and allowing them to interact with the target chemokine receptor.<ref name=Chan2 /><ref name=Wyatt /> This allows for a more stable two-pronged attachment, which allows the ] fusion peptide gp41 to penetrate the cell membrane.<ref name=Chan2 /><ref name=Wyatt /> ] in gp41, HR1, and HR2 then interact, causing the collapse of the extracellular portion of gp41 into a hairpin shape. This loop structure brings the virus and cell membranes close together, allowing fusion of the membranes and subsequent entry of the viral capsid.<ref name=Chan2 /><ref name=Wyatt /> | |||
| Sexual intercourse is the major mode of HIV transmission. Both X4 and R5 HIV are present in the ] which is passed from a male to his sexual partner. The virions can then infect numerous cellular targets and disseminate into the whole organism. However, a selection process leads to a predominant transmission of the R5 virus through this pathway.<ref name=Zhu1993> | |||
| After HIV has bound to the target cell, the HIV RNA and various enzymes, including reverse transcriptase, integrase, ribonuclease, and protease, are injected into the cell.<ref name=Chan2 />{{Failed verification|date=April 2014}} During the ]-based transport to the nucleus, the viral single-strand RNA genome is transcribed into double-strand DNA, which is then integrated into a host chromosome. | |||
| {{cite journal | |||
| | author=Zhu T, Mo H, Wang N, Nam DS, Cao Y, Koup RA, Ho DD. | title=Genotypic and phenotypic characterization of HIV-1 patients with primary infection | journal=Science | year=1993 | pages=1179–81 | volume=261 | issue=5125 | pmid=8356453 | doi=10.1126/science.8356453 | |||
| HIV can infect ]s (DCs) by this CD4-CCR5 route, but another route using ] such as ] can also be used.<ref name=Pope_2003>{{cite journal | vauthors = Pope M, Haase AT | title = Transmission, acute HIV-1 infection and the quest for strategies to prevent infection | journal = Nature Medicine | volume = 9 | issue = 7 | pages = 847–52 | year = 2003 | pmid = 12835704 | doi = 10.1038/nm0703-847 | s2cid = 26570505 | doi-access = free }}</ref> DCs are one of the first cells encountered by the virus during sexual transmission. They are currently thought to play an important role by transmitting HIV to T cells when the virus is captured in the ] by DCs.<ref name=Pope_2003 /> The presence of ], which occurs naturally in ]s, is believed to prevent the infection of cells by HIV.<ref>{{cite journal | vauthors = Haedicke J, Brown C, Naghavi MH | title = The brain-specific factor FEZ1 is a determinant of neuronal susceptibility to HIV-1 infection | journal = Proceedings of the National Academy of Sciences | volume = 106 | issue = 33 | pages = 14040–14045 | date = Aug 2009 | pmid = 19667186 | pmc = 2729016 | doi = 10.1073/pnas.0900502106 | bibcode = 2009PNAS..10614040H | doi-access = free }}</ref> | |||
| }}</ref><ref name=Wout> | |||
| ]]] | |||
| {{cite journal | |||
| HIV-1 entry, as well as entry of many other retroviruses, has long been believed to occur exclusively at the plasma membrane. More recently, however, productive infection by ]-independent, ] of HIV-1 has also been reported and was recently suggested to constitute the only route of productive entry.<ref>{{cite journal | vauthors = Daecke J, Fackler OT, Dittmar MT, Kräusslich HG | title = Involvement of clathrin-mediated endocytosis in human immunodeficiency virus type 1 entry | journal = Journal of Virology | volume = 79 | issue = 3 | pages = 1581–1594 | date = 2005 | pmid = 15650184 | pmc = 544101 | doi = 10.1128/jvi.79.3.1581-1594.2005 }}</ref><ref>{{cite journal | vauthors = Miyauchi K, Kim Y, Latinovic O, Morozov V, Melikyan GB | title = HIV Enters Cells via Endocytosis and Dynamin-Dependent Fusion with Endosomes | journal = Cell | volume = 137 | issue = 3 | pages = 433–444 | date = 2009 | pmid = 19410541 | pmc = 2696170 | doi = 10.1016/j.cell.2009.02.046 }}</ref><ref>{{cite journal | vauthors = Koch P, Lampe M, Godinez WJ, Müller B, Rohr K, Kräusslich HG, Lehmann MJ | title = Visualizing fusion of pseudotyped HIV-1 particles in real time by live cell microscopy | journal = Retrovirology | volume = 6 | pages = 84 | date = 2009 | pmid = 19765276 | pmc = 2762461 | doi = 10.1186/1742-4690-6-84 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Thorley JA, McKeating JA, Rappoport JZ | title = Mechanisms of viral entry: sneaking in the front door | journal = Protoplasma | volume = 244 | issue = 1–4 | pages = 15–24 | date = 2010 | pmid = 20446005 | pmc = 3038234 | doi = 10.1007/s00709-010-0152-6 }}</ref><ref>{{cite journal | vauthors = Permanyer M, Ballana E, Esté JA | title = Endocytosis of HIV: anything goes | journal = Trends in Microbiology | volume = 18 | issue = 12 | pages = 543–551 | date = 2010 | pmid = 20965729 | doi = 10.1016/j.tim.2010.09.003 }}</ref> | |||
| | author=van’t Wout AB, Kootstra NA, Mulder-Kampinga GA, Albrecht-van Lent N, Scherpbier HJ, Veenstra J, Boer K, Coutinho RA, Miedema F, Schuitemaker H. | title=Macrophage-tropic variants initiate human immunodeficiency virus type 1 infection after sexual, parenteral, and vertical transmission | journal=J Clin Invest | year=1994 | pages=2060–7 | volume=94 | issue=5 | pmid=7962552 | doi=10.1172/JCI117560 | |||
| ====Replication and transcription==== | |||
| }}</ref><ref name=Zhu1996> | |||
| ] of the HIV ] into ]]] | |||
| Shortly after the viral capsid enters the cell, an ] called ] liberates the positive-sense single-stranded ] genome from the attached viral proteins and copies it into a ] (cDNA) molecule.<ref name=Zheng>{{cite journal | vauthors = Zheng YH, Lovsin N, Peterlin BM | title = Newly identified host factors modulate HIV replication | journal = Immunology Letters | volume = 97 | issue = 2 | pages = 225–34 | year = 2005 | pmid = 15752562 | doi = 10.1016/j.imlet.2004.11.026 }}</ref> The process of reverse transcription is extremely error-prone, and the resulting mutations may cause ] or allow the virus to evade the body's immune system. The reverse transcriptase also has ribonuclease activity that degrades the viral RNA during the synthesis of cDNA, as well as DNA-dependent DNA polymerase activity that creates a ] DNA from the ''antisense'' cDNA.<ref>{{cite web |url=http://student.ccbcmd.edu/courses/bio141/lecguide/unit3/viruses/hivlc.html |website=Doc Kaiser's Microbiology Home Page |title=IV. Viruses> F. Animal Virus Life Cycles > 3. The Life Cycle of HIV |publisher=Community College of Baltimore County |date=January 2008 |url-status=dead |archive-url=https://web.archive.org/web/20100726222939/http://student.ccbcmd.edu/courses/bio141/lecguide/unit3/viruses/hivlc.html |archive-date=July 26, 2010 |df=mdy-all }}</ref> Together, the cDNA and its complement form a double-stranded viral DNA that is then transported into the ]. The integration of the viral DNA into the host cell's ] is carried out by another viral enzyme called ].<ref name=Zheng /> | |||
| {{cite journal | |||
| | author=Zhu T, Wang N, Carr A, Nam DS, Moor-Jankowski R, Cooper DA, Ho DD. | title=Genetic characterization of human immunodeficiency virus type 1 in blood and genital secretions: evidence for viral compartmentalization and selection during sexual transmission | journal=J Virol | year=1996 | pages=3098–107 | volume=70 | issue=5 | pmid=8627789 | |||
| The integrated viral DNA may then lie dormant, in the latent stage of HIV infection.<ref name=Zheng /> To actively produce the virus, certain cellular ]s need to be present, the most important of which is ] (nuclear factor kappa B), which is upregulated when T cells become activated.<ref name=Hiscott>{{cite journal | vauthors = Hiscott J, Kwon H, Génin P | title = Hostile takeovers: viral appropriation of the NF-kB pathway | journal = Journal of Clinical Investigation | volume = 107 | issue = 2 | pages = 143–151 | year = 2001 | pmid = 11160127 | pmc = 199181 | doi = 10.1172/JCI11918 }}</ref> This means that those cells most likely to be targeted, entered and subsequently killed by HIV are those actively fighting infection. | |||
| }}</ref> How this selective process works is still under investigation, but one model is that ] may selectively carry R5 HIV as they possess both CCR3 and CCR5 but not CXCR4 on their surface<ref name=Muciaccia> | |||
| During viral replication, the integrated DNA ] is ] into RNA. The full-length genomic RNAs (gRNA) can be packaged into new viral particles in a ] form. The selectivity in the packaging is explained by the structural properties of the dimeric conformer of the gRNA. The gRNA dimer is characterized by a tandem three-way junction within the gRNA monomer, in which the SD and AUG ], responsible for splicing and translation respectively, are sequestered and the DIS (dimerization initiation signal) hairpin is exposed. The formation of the gRNA dimer is mediated by a 'kissing' interaction between the DIS hairpin loops of the gRNA monomers. At the same time, certain guanosine residues in the gRNA are made available for binding of the nucleocapsid (NC) protein leading to the subsequent virion assembly.<ref>{{Cite journal|last1=Keane|first1=Sarah C.|last2=Heng|first2=Xiao|last3=Lu|first3=Kun|last4=Kharytonchyk|first4=Siarhei|last5=Ramakrishnan|first5=Venkateswaran|last6=Carter|first6=Gregory|last7=Barton|first7=Shawn|last8=Hosic|first8=Azra|last9=Florwick|first9=Alyssa|last10=Santos|first10=Justin|last11=Bolden|first11=Nicholas C.|date=2015-05-22|title=Structure of the HIV-1 RNA packaging signal|url=http://dx.doi.org/10.1126/science.aaa9266|journal=Science|volume=348|issue=6237|pages=917–921|doi=10.1126/science.aaa9266|pmid=25999508|pmc=4492308|bibcode=2015Sci...348..917K|issn=0036-8075}}</ref> The labile gRNA dimer has been also reported to achieve a more stable conformation following the NC binding, in which both the DIS and the U5:AUG regions of the gRNA participate in extensive base pairing.<ref>{{Cite journal|last1=Keane|first1=Sarah C.|last2=Van|first2=Verna|last3=Frank|first3=Heather M.|last4=Sciandra|first4=Carly A.|last5=McCowin|first5=Sayo|last6=Santos|first6=Justin|last7=Heng|first7=Xiao|last8=Summers|first8=Michael F.|date=2016-10-10|title=NMR detection of intermolecular interaction sites in the dimeric 5′-leader of the HIV-1 genome|journal=Proceedings of the National Academy of Sciences|volume=113|issue=46|pages=13033–13038|doi=10.1073/pnas.1614785113|pmid=27791166|pmc=5135362|bibcode=2016PNAS..11313033K |issn=0027-8424|doi-access=free}}</ref> | |||
| {{cite journal | |||
| | author=Muciaccia B, Padula F, Vicini E, Gandini L, Lenzi A, Stefanini M. | title=Beta-chemokine receptors 5 and 3 are expressed on the head region of human spermatozoon | journal=FASEB J | year=2005 | pages=2048–50 | volume=19 | issue=14 | pmid=16174786 | |||
| RNA can also be ] to produce mature ]s (mRNAs). In most cases, this processing involves ] to produce mRNAs that are shorter than the full-length genome. Which part of the RNA is removed during RNA splicing determines which of the HIV protein-coding sequences is translated.<ref name="Ocwieja">{{cite journal | vauthors = Ocwieja KE, Sherrill-Mix S, Mukherjee R, Custers-Allen R, David P, Brown M, Wang S, Link DR, Olson J, Travers K, Schadt E, Bushman FD | display-authors = 6 | title = Dynamic regulation of HIV-1 mRNA populations analyzed by single-molecule enrichment and long-read sequencing | journal = Nucleic Acids Research | volume = 40 | issue = 20 | pages = 10345–55 | date = November 2012 | pmid = 22923523 | pmc = 3488221 | doi = 10.1093/nar/gks753 | url = https://academic.oup.com/nar/article/40/20/10345/2414624 }}</ref> | |||
| }}</ref> and that genital ]s preferentially sequester X4 virus.<ref name=Berlier> | |||
| Mature HIV mRNAs are exported from the nucleus into the ], where they are ] to produce HIV proteins, including ]. As the newly produced Rev protein is produced it moves to the nucleus, where it binds to full-length, unspliced copies of virus RNAs and allows them to leave the nucleus.<ref name=Pollard>{{cite journal | vauthors = Pollard VW, Malim MH | title = The HIV-1 Rev protein | journal = Annual Review of Microbiology | volume = 52 | pages = 491–532 | year = 1998 | pmid = 9891806 | doi = 10.1146/annurev.micro.52.1.491 }}</ref> Some of these full-length RNAs function as mRNAs that are translated to produce the structural proteins Gag and Env. Gag proteins bind to copies of the virus RNA genome to package them into new virus particles.<ref>{{cite journal | vauthors = Butsch M, Boris-Lawrie K | title = Destiny of unspliced retroviral RNA: ribosome and/or virion? | journal = Journal of Virology | volume = 76 | issue = 7 | pages = 3089–94 | date = April 2002 | pmid = 11884533 | pmc = 136024 | doi = 10.1128/JVI.76.7.3089-3094.2002 }}</ref> | |||
| {{cite journal | |||
| HIV-1 and HIV-2 appear to package their RNA differently.<ref>{{cite journal | vauthors = Hellmund C, Lever AM | title = Coordination of Genomic RNA Packaging with Viral Assembly in HIV-1 | journal = Viruses | volume = 8 | issue = 7 | pages = 192 | date = July 2016 | pmid = 27428992 | pmc = 4974527 | doi = 10.3390/v8070192 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Soto-Rifo R, Limousin T, Rubilar PS, Ricci EP, Décimo D, Moncorgé O, Trabaud MA, André P, Cimarelli A, Ohlmann T | display-authors = 6 | title = Different effects of the TAR structure on HIV-1 and HIV-2 genomic RNA translation | journal = Nucleic Acids Research | volume = 40 | issue = 6 | pages = 2653–67 | date = March 2012 | pmid = 22121214 | pmc = 3315320 | doi = 10.1093/nar/gkr1093 }}</ref> HIV-1 will bind to any appropriate RNA.<ref>{{Cite book|url=https://books.google.com/books?id=P3vQCgAAQBAJ&q=HIV-1+will+bind+to+any+appropriate+RNA&pg=PA51|title=Role of Lipids in Virus Assembly| vauthors = Saad JS, Muriaux DM |date=2015-07-28|publisher=Frontiers Media SA|isbn=978-2-88919-582-4|language=en}}</ref> HIV-2 will preferentially bind to the mRNA that was used to create the Gag protein itself.<ref>{{cite journal | vauthors = Ricci EP, Herbreteau CH, Decimo D, Schaupp A, Datta SA, Rein A, Darlix JL, Ohlmann T | display-authors = 6 | title = In vitro expression of the HIV-2 genomic RNA is controlled by three distinct internal ribosome entry segments that are regulated by the HIV protease and the Gag polyprotein | journal = RNA | volume = 14 | issue = 7 | pages = 1443–55 | date = July 2008 | pmid = 18495939 | pmc = 2441975 | doi = 10.1261/rna.813608 }}</ref> | |||
| | author=Berlier W, Bourlet T, Lawrence P, Hamzeh H, Lambert C, Genin C, Verrier B, Dieu-Nosjean MC, Pozzetto B, Delezay O. | title=Selective sequestration of X4 isolates by human genital epithelial cells: Implication for virus tropism selection process during sexual transmission of HIV | journal=J Med Virol. | year=2005 | pages=465–74 | volume=77 | issue=4 | pmid=16254974 | doi=10.1002/jmv.20478 | |||
| ====Recombination==== | |||
| }}</ref> In patients infected with subtype B HIV-1, there is often a co-receptor switch in late-stage disease and T-tropic variants appear that can infect a variety of T cells through CXCR4.<ref name=Clevestig> | |||
| {{Further|Genetic recombination}} | |||
| Two RNA genomes are encapsidated in each HIV-1 particle (see ]). Upon infection and replication catalyzed by reverse transcriptase, recombination between the two genomes can occur.<ref name="Hu">{{cite journal | vauthors = Hu WS, Temin HM | title = Retroviral recombination and reverse transcription | journal = Science | volume = 250 | issue = 4985 | pages = 1227–33 | year = 1990 | pmid = 1700865 | doi = 10.1126/science.1700865 | bibcode = 1990Sci...250.1227H }}</ref><ref name="Charpentier">{{cite journal | vauthors = Charpentier C, Nora T, Tenaillon O, Clavel F, Hance AJ | title = Extensive recombination among human immunodeficiency virus type 1 quasispecies makes an important contribution to viral diversity in individual patients | journal = Journal of Virology | volume = 80 | issue = 5 | pages = 2472–82 | year = 2006 | pmid = 16474154 | pmc = 1395372 | doi = 10.1128/JVI.80.5.2472-2482.2006 }}</ref> Recombination occurs as the single-strand, positive-sense RNA genomes are reverse transcribed to form DNA. During reverse transcription, the nascent DNA can switch multiple times between the two copies of the viral RNA. This form of recombination is known as copy-choice. Recombination events may occur throughout the genome. Anywhere from two to 20 recombination events per genome may occur at each replication cycle, and these events can rapidly shuffle the genetic information that is transmitted from parental to progeny genomes.<ref name="Charpentier" /> | |||
| Viral recombination produces genetic variation that likely contributes to the ] of resistance to ].<ref>{{cite journal | vauthors = Nora T, Charpentier C, Tenaillon O, Hoede C, Clavel F, Hance AJ | title = Contribution of recombination to the evolution of human immunodeficiency viruses expressing resistance to antiretroviral treatment | journal = Journal of Virology | volume = 81 | issue = 14 | pages = 7620–8 | year = 2007 | pmid = 17494080 | pmc = 1933369 | doi = 10.1128/JVI.00083-07 }}</ref> Recombination may also contribute, in principle, to overcoming the immune defenses of the host. Yet, for the adaptive advantages of genetic variation to be realized, the two viral genomes packaged in individual infecting virus particles need to have arisen from separate progenitor parental viruses of differing genetic constitution. It is unknown how often such mixed packaging occurs under natural conditions.<ref>{{cite journal | vauthors = Chen J, Powell D, Hu WS | title = High frequency of genetic recombination is a common feature of primate lentivirus replication | journal = Journal of Virology | volume = 80 | issue = 19 | pages = 9651–8 | year = 2006 | pmid = 16973569 | pmc = 1617242 | doi = 10.1128/JVI.00936-06 }}</ref> | |||
| {{cite journal | |||
| | author=Clevestig P, Maljkovic I, Casper C, Carlenor E, Lindgren S, Naver L, Bohlin AB, Fenyo EM, Leitner T, Ehrnst A. | title=The X4 phenotype of HIV type 1 evolves from R5 in two children of mothers, carrying X4, and is not linked to transmission | journal=AIDS Res Hum Retroviruses | year=2005 | pages=371–8 | volume=5 | issue=21 | pmid=15929699 | doi=10.1089/aid.2005.21.371 | |||
| Bonhoeffer ''et al.''<ref name=Bonhoeffer>{{cite journal | vauthors = Bonhoeffer S, Chappey C, Parkin NT, Whitcomb JM, Petropoulos CJ | title = Evidence for positive epistasis in HIV-1 | journal = Science | volume = 306 | issue = 5701 | pages = 1547–50 | year = 2004 | pmid = 15567861 | doi = 10.1126/science.1101786 | bibcode = 2004Sci...306.1547B | s2cid = 45784964 }}</ref> suggested that template switching by reverse transcriptase acts as a repair process to deal with breaks in the single-stranded RNA genome. In addition, Hu and Temin<ref name=Hu /> suggested that recombination is an adaptation for repair of damage in the RNA genomes. Strand switching (copy-choice recombination) by reverse transcriptase could generate an undamaged copy of genomic DNA from two damaged single-stranded RNA genome copies. This view of the adaptive benefit of recombination in HIV could explain why each HIV particle contains two complete genomes, rather than one. Furthermore, the view that recombination is a repair process implies that the benefit of repair can occur at each replication cycle, and that this benefit can be realized whether or not the two genomes differ genetically. On the view that recombination in HIV is a repair process, the generation of recombinational variation would be a consequence, but not the cause of, the evolution of template switching.<ref name=Bonhoeffer /> | |||
| }}</ref> These variants then replicate more aggressively with heightened virulence that causes rapid T cell depletion, immune system collapse, and opportunistic infections that mark the advent of AIDS.<ref name=Moore> | |||
| HIV-1 infection causes ] and production of ].<ref>{{cite journal | vauthors = Israël N, Gougerot-Pocidalo MA | title = Oxidative stress in human immunodeficiency virus infection | journal = Cellular and Molecular Life Sciences | volume = 53 | issue = 11–12 | pages = 864–70 | year = 1997 | pmid = 9447238 | doi = 10.1007/s000180050106 | s2cid = 22663454 | pmc = 11147326 }}</ref> Thus, the HIV genome may be vulnerable to ], including breaks in the single-stranded RNA. For HIV, as well as for viruses in general, successful infection depends on overcoming host defense strategies that often include production of genome-damaging reactive oxygen species. Thus, Michod ''et al.''<ref name="pmid18295550">{{cite journal | vauthors = Michod RE, Bernstein H, Nedelcu AM | title = Adaptive value of sex in microbial pathogens | journal = Infection, Genetics and Evolution | volume = 8 | issue = 3 | pages = 267–85 | date = May 2008 | pmid = 18295550 | doi = 10.1016/j.meegid.2008.01.002 | bibcode = 2008InfGE...8..267M | url = http://www.hummingbirds.arizona.edu/Faculty/Michod/Downloads/IGE%20review%20sex.pdf | access-date = May 10, 2013 | archive-date = May 16, 2017 | archive-url = https://web.archive.org/web/20170516235741/http://www.hummingbirds.arizona.edu/Faculty/Michod/Downloads/IGE%20review%20sex.pdf | url-status = dead }}</ref> suggested that recombination by viruses is an adaptation for repair of genome damage, and that recombinational variation is a byproduct that may provide a separate benefit. | |||
| {{cite journal | |||
| | author=Moore JP.| title=Coreceptors: implications for HIV pathogenesis and therapy | journal=Science | year=1997 | pages=51–2 | volume=276 | issue=5309 | pmid=9122710 | doi=10.1126/science.276.5309.51 | |||
| ====Assembly and release==== | |||
| }}</ref> Thus, during the course of infection, viral adaptation to the use of CXCR4 instead of CCR5 may be a key step in the progression to AIDS. A number of studies with subtype B-infected individuals have determined that between 40 and 50% of AIDS patients can harbour viruses of the SI, and presumably the X4, phenotype.<ref name=Karlsson> | |||
| ] of an infected ]. The HIV virions have been marked with a green ] and then viewed under a fluorescent microscope.]] | |||
| The final step of the viral cycle, assembly of new HIV-1 virions, begins at the ] of the host cell. The Env polyprotein (gp160) goes through the ] and is transported to the ] where it is ] by ] resulting in the two HIV envelope glycoproteins, ] and ].<ref>{{cite journal | vauthors = Hallenberger S, Bosch V, Angliker H, Shaw E, Klenk HD, Garten W | title = Inhibition of furin-mediated cleavage activation of HIV-1 glycoprotein gp160 | journal = Nature | volume = 360 | issue = 6402 | pages = 358–61 | date = November 26, 1992 | pmid = 1360148 | doi = 10.1038/360358a0 | bibcode = 1992Natur.360..358H | s2cid = 4306605 }}</ref> These are transported to the plasma membrane of the host cell where gp41 anchors gp120 to the membrane of the infected cell. The Gag (p55) and Gag-Pol (p160) polyproteins also associate with the inner surface of the plasma membrane along with the HIV genomic RNA as the forming virion begins to bud from the host cell. The budded virion is still immature as the ] polyproteins still need to be cleaved into the actual matrix, capsid and nucleocapsid proteins. This cleavage is mediated by the packaged viral protease and can be inhibited by antiretroviral drugs of the ] class. The various structural components then assemble to produce a mature HIV virion.<ref name=Gelderblom>{{cite book | author= Gelderblom HR | year = 1997 | title = HIV sequence compendium | chapter = Fine structure of HIV and SIV |chapter-url=http://www.hiv.lanl.gov/content/sequence/HIV/COMPENDIUM/1997/partIII/Gelderblom.pdf | editor = Los Alamos National Laboratory | pages = 31–44 | publisher = ] }}</ref> Only mature virions are then able to infect another cell. | |||
| ===Spread within the body=== | |||
| {{cite journal | |||
| ] | |||
| | author=Karlsson A, Parsmyr K, Aperia K, Sandstrom E, Fenyo EM, Albert J.| title=MT-2 cell tropism of human immunodeficiency virus type 1 isolates as a marker for response to treatment and development of drug resistance | journal=J Infect Dis. | year=1994 | pages=1367–75 | volume=170 | issue=6 | pmid=7995974 | |||
| The classical process of infection of a cell by a virion can be called "cell-free spread" to distinguish it from a more recently recognized process called "cell-to-cell spread".<ref name=Zhang>{{cite journal | vauthors = Zhang C, Zhou S, Groppelli E, Pellegrino P, Williams I, Borrow P, Chain BM, Jolly C | title = Hybrid Spreading Mechanisms and T Cell Activation Shape the Dynamics of HIV-1 Infection | journal = PLOS Computational Biology | volume = 11 | issue = 4 | pages = e1004179 | year = 2015 | pmid = 25837979 | pmc = 4383537 | doi = 10.1371/journal.pcbi.1004179 | arxiv = 1503.08992 | bibcode = 2015PLSCB..11E4179Z | doi-access = free }}</ref> In cell-free spread (see figure), virus particles bud from an infected T cell, enter the blood or ] and then infect another T cell following a chance encounter.<ref name="Zhang" /> HIV can also disseminate by direct transmission from one cell to another by a process of cell-to-cell spread, for which two pathways have been described. Firstly, an infected T cell can transmit virus directly to a target T cell via a ].<ref name="Arthos" /><ref name=Jolly>{{cite journal | vauthors = Jolly C, Kashefi K, Hollinshead M, Sattentau QJ | title = HIV-1 cell to cell transfer across an Env-induced, actin-dependent synapse | journal = Journal of Experimental Medicine | volume = 199 | issue = 2 | pages = 283–293 | year = 2004| pmid = 14734528 | pmc = 2211771 | doi = 10.1084/jem.20030648 }}</ref> Secondly, an ] (APC), such as a macrophage or dendritic cell, can transmit HIV to T cells by a process that either involves productive infection (in the case of macrophages) or capture and transfer of virions ''in trans'' (in the case of dendritic cells).<ref name=Sattentau>{{cite journal | vauthors = Sattentau Q | title = Avoiding the void: cell-to-cell spread of human viruses | journal = Nature Reviews Microbiology | volume = 6 | issue = 11 | pages = 815–826 | year = 2008| pmid = 18923409 | doi = 10.1038/nrmicro1972 | s2cid = 20991705 | doi-access = free }}</ref> Whichever pathway is used, infection by cell-to-cell transfer is reported to be much more efficient than cell-free virus spread.<ref name=Duncan>{{cite journal | vauthors = Duncan CJ, Russell RA, Sattentau QJ | title = High multiplicity HIV-1 cell-to-cell transmission from macrophages to CD4+ T cells limits antiretroviral efficacy | journal = AIDS | volume = 27 | issue = 14 | pages = 2201–2206 | year = 2013 | pmid = 24005480 | pmc = 4714465 | doi = 10.1097/QAD.0b013e3283632ec4 }}</ref> A number of factors contribute to this increased efficiency, including polarised virus budding towards the site of cell-to-cell contact, close apposition of cells, which minimizes fluid-phase ] of virions, and clustering of HIV entry receptors on the target cell towards the contact zone.<ref name="Jolly" /> Cell-to-cell spread is thought to be particularly important in ]s, where CD4<sup>+</sup> T cells are densely packed and likely to interact frequently.<ref name="Zhang" /> ] studies have supported the concept of the HIV virological synapse ''in vivo''.<ref name=Sewald>{{cite journal | vauthors = Sewald X, Gonzalez DG, Haberman AM, Mothes W | title = In vivo imaging of virological synapses | journal = Nature Communications | volume = 3 | pages = 1320 | year = 2012 | pmid = 23271654 | pmc = 3784984 | doi = 10.1038/ncomms2338 | bibcode = 2012NatCo...3.1320S }}</ref> The many dissemination mechanisms available to HIV contribute to the virus' ongoing replication in spite of anti-retroviral therapies.<ref name="Zhang" /><ref name=Sigal>{{cite journal | vauthors = Sigal A, Kim JT, Balazs AB, Dekel E, Mayo A, Milo R, Baltimore D | title = Cell-to-cell spread of HIV permits ongoing replication despite antiretroviral therapy | journal = Nature | volume = 477 | issue = 7362 | pages = 95–98 | year = 2011 | pmid = 21849975 | doi = 10.1038/nature10347 | bibcode = 2011Natur.477...95S | s2cid = 4409389 | url = https://resolver.caltech.edu/CaltechAUTHORS:20110922-140553274 }}</ref> | |||
| ===Genetic variability=== | |||
| }}</ref><ref name=Koot> | |||
| {{Further|Subtypes of HIV}} | |||
| ] of the SIV and HIV]] | |||
| HIV differs from many viruses in that it has very high ]. This diversity is a result of its fast ], with the generation of about 10<sup>10</sup> virions every day, coupled with a high ] of approximately 3 x 10<sup>−5</sup> per ] per cycle of replication and ] properties of reverse transcriptase.<ref name=RobertsonDL>{{cite journal | vauthors = Robertson DL, Hahn BH, Sharp PM | title = Recombination in AIDS viruses | journal = Journal of Molecular Evolution | volume = 40 | issue = 3 | pages = 249–59 | year = 1995 | pmid = 7723052 | doi = 10.1007/BF00163230 | bibcode = 1995JMolE..40..249R | s2cid = 19728830 | doi-access = free }}</ref><ref name="Rambaut_2004">{{cite journal | vauthors = Rambaut A, Posada D, Crandall KA, Holmes EC | title = The causes and consequences of HIV evolution | journal = Nature Reviews Genetics | volume = 5 | issue = 52–61 | pages = 52–61 | date = January 2004 | pmid = 14708016 | doi = 10.1038/nrg1246 | s2cid = 5790569 | doi-access = free }}</ref><ref name="pmid17960579">{{cite journal | vauthors = Perelson AS, Ribeiro RM | title = Estimating drug efficacy and viral dynamic parameters: HIV and HCV | journal = Statistics in Medicine | volume = 27 | issue = 23 | pages = 4647–57 | date = October 2008 | pmid = 17960579 | doi = 10.1002/sim.3116 | s2cid = 33662579 | url = https://zenodo.org/record/1229363 }}</ref> | |||
| This complex scenario leads to the generation of many variants of HIV in a single infected patient in the course of one day.<ref name=RobertsonDL /> This variability is compounded when a single cell is simultaneously infected by two or more different strains of HIV. When ] occurs, the genome of progeny virions may be composed of RNA strands from two different strains. This hybrid virion then infects a new cell where it undergoes replication. As this happens, the reverse transcriptase, by jumping back and forth between the two different RNA templates, will generate a newly synthesized retroviral ] that is a recombinant between the two parental genomes.<ref name=RobertsonDL /> This recombination is most obvious when it occurs between subtypes.<ref name=RobertsonDL /> | |||
| {{cite journal | |||
| | author=Koot M, van 't Wout AB, Kootstra NA, de Goede RE, Tersmette M, Schuitemaker H.| title=Relation between changes in cellular load, evolution of viral phenotype, and the clonal composition of virus populations in the course of human immunodeficiency virus type 1 infection | journal=J Infect Dis. | year=1996 | pages=349–54 | volume=173 | issue=2 | pmid=8568295 | |||
| The closely related ] (SIV) has evolved into many strains, classified by the natural host species. SIV strains of the ] (SIVagm) and ] (SIVsmm) are thought to have a long evolutionary history with their hosts. These hosts have adapted to the presence of the virus,<ref name=pmid19661993>{{cite journal | vauthors = Sodora DL, Allan JS, Apetrei C, Brenchley JM, Douek DC, Else JG, Estes JD, Hahn BH, Hirsch VM, Kaur A, Kirchhoff F, Muller-Trutwin M, Pandrea I, Schmitz JE, Silvestri G | title = Toward an AIDS vaccine: lessons from natural simian immunodeficiency virus infections of African nonhuman primate hosts | journal = Nature Medicine | volume = 15 | issue = 8 | pages = 861–865 | year = 2009 | pmid = 19661993 | pmc = 2782707 | doi = 10.1038/nm.2013 }}</ref> which is present at high levels in the host's blood, but evokes only a mild immune response,<ref>{{cite journal | vauthors = Holzammer S, Holznagel E, Kaul A, Kurth R, Norley S | title = High virus loads in naturally and experimentally SIVagm-infected African green monkeys | journal = Virology | volume = 283 | issue = 2 | pages = 324–31 | year = 2001 | pmid = 11336557 | doi = 10.1006/viro.2001.0870 | doi-access = free }}</ref> does not cause the development of simian AIDS,<ref>{{Cite journal |last1=Kurth |first1= R. |last2=Norley |first2= S. | year = 1996 | title = Why don't the natural hosts of SIV develop simian AIDS? | journal = The Journal of NIH Research | volume = 8 | pages = 33–37 }}</ref> and does not undergo the extensive mutation and recombination typical of HIV infection in humans.<ref>{{cite journal | vauthors = Baier M, Dittmar MT, Cichutek K, Kurth R | title = Development of vivo of genetic variability of simian immunodeficiency virus | journal = Proceedings of the National Academy of Sciences of the United States of America | volume = 88 | issue = 18 | pages = 8126–30 | year = 1991 | pmid = 1896460 | pmc = 52459 | doi = 10.1073/pnas.88.18.8126 | bibcode = 1991PNAS...88.8126B | doi-access = free }}</ref> | |||
| }}</ref> | |||
| In contrast, when these strains infect species that have not adapted to SIV ("heterologous" or similar hosts such as ] or ]), the animals develop AIDS and the virus generates ] similar to what is seen in human HIV infection.<ref>{{cite journal | vauthors = Daniel MD, King NW, Letvin NL, Hunt RD, Sehgal PK, Desrosiers RC | title = A new type D retrovirus isolated from macaques with an immunodeficiency syndrome | journal = Science | volume = 223 | issue = 4636 | pages = 602–5 | year = 1984 | pmid = 6695172 | doi = 10.1126/science.6695172 | bibcode = 1984Sci...223..602D }}</ref> ] SIV (SIVcpz), the closest genetic relative of HIV-1, is associated with increased mortality and AIDS-like symptoms in its natural host.<ref name=pmid19626114>{{cite journal | vauthors = Keele BF, Jones JH, Terio KA, Estes JD, Rudicell RS, Wilson ML, Li Y, Learn GH, Beasley TM, Schumacher-Stankey J, Wroblewski E, Mosser A, Raphael J, Kamenya S, Lonsdorf EV, Travis DA, Mlengeya T, Kinsel MJ, Else JG, Silvestri G, Goodall J, Sharp PM, Shaw GM, Pusey AE, Hahn BH | title = Increased mortality and AIDS-like immunopathology in wild chimpanzees infected with SIVcpz | journal = Nature | volume = 460 | issue = 7254 | pages = 515–519 | year = 2009 | pmid = 19626114 | pmc = 2872475 | doi = 10.1038/nature08200 | bibcode = 2009Natur.460..515K }}</ref> SIVcpz appears to have been transmitted relatively recently to chimpanzee and human populations, so their hosts have not yet adapted to the virus.<ref name=pmid19661993 /> This virus has also lost a function of the '']'' gene that is present in most SIVs. For non-pathogenic SIV variants, ''nef'' suppresses T cell activation through the ] marker. ''Nef''{{'s}} function in non-pathogenic forms of SIV is to ] expression of ], ], and signals that affect T cell trafficking. In HIV-1 and SIVcpz, ''nef'' does not inhibit T-cell activation and it has lost this function. Without this function, T cell depletion is more likely, leading to immunodeficiency.<ref name=pmid19626114 /><ref>{{cite journal | vauthors = Schindler M, Münch J, Kutsch O, Li H, Santiago ML, Bibollet-Ruche F, Müller-Trutwin MC, Novembre FJ, Peeters M, Courgnaud V, Bailes E, Roques P, Sodora DL, Silvestri G, Sharp PM, Hahn BH, Kirchhoff F | title = Nef-mediated suppression of T cell activation was lost in a lentiviral lineage that gave rise to HIV-1 | journal = Cell | volume = 125 | issue = 6 | pages = 1055–67 | date = 2006 | pmid = 16777597 | doi = 10.1016/j.cell.2006.04.033 | s2cid = 15132918 | doi-access = free }}</ref> | |||
| ==Replication cycle== | |||
| ] | |||
| ===Entry to the cell=== | |||
| HIV enters macrophages and CD4<SUP>+</SUP> T cells by the ] of ]s on its surface to receptors on the target cell followed by fusion of the viral envelope with the cell membrane and the release of the HIV capsid into the cell.<ref name=Chan2>{{cite journal |author=Chan D, Kim P |title=HIV entry and its inhibition |journal=Cell |volume=93 |issue=5 |pages=681–4 |year=1998 |pmid=9630213 |doi=10.1016/S0092-8674(00)81430-0}}</ref><ref name=Wyatt>{{cite journal |author=Wyatt R, Sodroski J |title=The HIV-1 envelope glycoproteins: fusogens, antigens, and immunogens |journal=Science |volume=280 |issue=5371 |pages=1884–8 |year=1998 | doi=10.1126/science.280.5371.1884 |pmid=9632381}}</ref> | |||
| Three groups of HIV-1 have been identified on the basis of differences in the envelope (''env'') region: M, N, and O.<ref name=Thomson>{{cite journal | vauthors = Thomson MM, Pérez-Alvarez L, Nájera R | title = Molecular epidemiology of HIV-1 genetic forms and its significance for vaccine development and therapy | journal = The Lancet Infectious Diseases | volume = 2 | issue = 8 | pages = 461–471 | year = 2002 | pmid = 12150845 | doi = 10.1016/S1473-3099(02)00343-2 }}</ref> Group M is the most prevalent and is subdivided into eight subtypes (or ]s), based on the whole genome, which are geographically distinct.<ref name=Carr>{{cite book |vauthors = Carr JK, Foley BT, Leitner T, Salminen M, Korber B, McCutchan F | year = 1998 | title = HIV sequence compendium | chapter = Reference sequences representing the principal genetic diversity of HIV-1 in the pandemic | chapter-url = http://www.hiv.lanl.gov/content/sequence/HIV/COMPENDIUM/1998/III/Carr.pdf | editor = Los Alamos National Laboratory | pages = 10–19 | publisher = ] | location = ] }}</ref> The most prevalent are subtypes B (found mainly in North America and Europe), A and D (found mainly in Africa), and C (found mainly in Africa and Asia); these subtypes form branches in the ] representing the lineage of the M group of HIV-1. ] with distinct subtypes gives rise to circulating recombinant forms (CRFs). In 2000, the last year in which an analysis of global subtype prevalence was made, 47.2% of infections worldwide were of subtype C, 26.7% were of subtype A/CRF02_AG, 12.3% were of subtype B, 5.3% were of subtype D, 3.2% were of CRF_AE, and the remaining 5.3% were composed of other subtypes and CRFs.<ref name=Osmanov>{{cite journal | vauthors = Osmanov S, Pattou C, Walker N, Schwardländer B, Esparza J | title = Estimated global distribution and regional spread of HIV-1 genetic subtypes in the year 2000 | journal = Journal of Acquired Immune Deficiency Syndromes| volume = 29 | issue = 2 | pages = 184–190 | year = 2002 | pmid = 11832690 | doi = 10.1097/00042560-200202010-00013 | author6 = WHO-UNAIDS Network for HIV Isolation Characterization | s2cid = 12536801 }}</ref> Most HIV-1 research is focused on subtype B; few laboratories focus on the other subtypes.<ref name=Perrin>{{cite journal | vauthors = Perrin L, Kaiser L, Yerly S | title = Travel and the spread of HIV-1 genetic variants | journal = The Lancet Infectious Diseases | volume = 3 | issue = 1 | pages = 22–27 | year = 2003 | pmid = 12505029 | doi = 10.1016/S1473-3099(03)00484-5 }}</ref> The existence of a fourth group, "P", has been hypothesised based on a virus isolated in 2009.<ref name="Plantier_2009">{{cite journal | vauthors = Plantier JC, Leoz M, Dickerson JE, De Oliveira F, Cordonnier F, Lemée V, Damond F, Robertson DL, Simon F | title = A new human immunodeficiency virus derived from gorillas | journal = Nature Medicine | volume = 15 | issue = 8 | pages = 871–2 | date = August 2009 | pmid = 19648927 | doi = 10.1038/nm.2016 | s2cid = 76837833 }}</ref><ref name="Smith 2009">{{cite web | last=Smith | first=Lewis | title=Woman found carrying new strain of HIV from gorillas | website=The Independent | date=August 3, 2009 | url=https://www.independent.co.uk/life-style/health-and-families/health-news/woman-found-carrying-new-strain-of-hiv-from-gorillas-1766627.html | access-date=November 27, 2015}}</ref> The strain is apparently derived from ] SIV (SIVgor), first isolated from ]s in 2006.<ref name="Plantier_2009" /> | |||
| Entry to the cell begins through interaction of the trimeric envelope complex (] spike) and both ] and a chemokine receptor (generally either ] or ], but others are known to interact) on the cell surface.<ref name=Chan2/><ref name=Wyatt/> gp120 binds to ] α<sub>4</sub>β<sub>7</sub> activating ] the central integrin involved in the establishment of virological synapses, which facilitate efficient cell-to-cell spreading of HIV-1.<ref name=Arthos>{{cite journal |author=Arthos J, Cicala C, Martinelli E, Macleod K, Van Ryk D, Wei D, Xiao Z, Veenstra TD, Conrad TP, Lempicki RA, McLaughlin S, Pascuccio M, Gopaul R, McNally J, Cruz CC, Censoplano N, Chung E, Reitano KN, Kottilil S, Goode DJ, Fauci AS. |title=HIV-1 envelope protein binds to and signals through integrin alpha(4)beta(7), the gut mucosal homing receptor for peripheral T cells |journal=Nature Immunol. |volume=In Press |issue= |pages= 301|year=2008|pmid=18264102 |doi=10.1038/ni1566}}</ref> The gp160 spike contains binding domains for both CD4 and chemokine receptors.<ref name=Chan2/><ref name=Wyatt/> The first step in fusion involves the high-affinity attachment of the CD4 binding domains of ] to CD4. Once gp120 is bound with the CD4 protein, the envelope complex undergoes a structural change, exposing the chemokine binding domains of gp120 and allowing them to interact with the target chemokine receptor.<ref name=Chan2/><ref name=Wyatt/> This allows for a more stable two-pronged attachment, which allows the N-terminal fusion peptide gp41 to penetrate the cell membrane.<ref name=Chan2/><ref name=Wyatt/> Repeat sequences in gp41, HR1 and HR2 then interact, causing the collapse of the extracellular portion of gp41 into a hairpin. This loop structure brings the virus and cell membranes close together, allowing fusion of the membranes and subsequent entry of the viral capsid.<ref name=Chan2/><ref name=Wyatt/> | |||
| HIV-2's closest relative is SIVsm, a strain of SIV found in sooty mangabees. Since HIV-1 is derived from SIVcpz, and HIV-2 from SIVsm, the genetic sequence of HIV-2 is only partially homologous to HIV-1 and more closely resembles that of SIVsm.<ref>{{cite journal | vauthors = Sharp PM, Hahn BH | title = The evolution of HIV-1 and the origin of AIDS | journal = Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences | volume = 365 | issue = 1552 | pages = 2487–94 | date = August 2010 | pmid = 20643738 | pmc = 2935100 | doi = 10.1098/rstb.2010.0031 }}</ref><ref>{{cite journal | vauthors = Keele BF, Van Heuverswyn F, Li Y, Bailes E, Takehisa J, Santiago ML, Bibollet-Ruche F, Chen Y, Wain LV, Liegeois F, Loul S, Ngole EM, Bienvenue Y, Delaporte E, Brookfield JF, Sharp PM, Shaw GM, Peeters M, Hahn BH | display-authors = 6 | title = Chimpanzee reservoirs of pandemic and nonpandemic HIV-1 | journal = Science | volume = 313 | issue = 5786 | pages = 523–6 | date = July 2006 | pmid = 16728595 | pmc = 2442710 | doi = 10.1126/science.1126531 | bibcode = 2006Sci...313..523K }}</ref> | |||
| Once HIV has bound to the target cell, the HIV ] and various ]s, including reverse transcriptase, integrase, ribonuclease and protease, are injected into the cell.<ref name=Chan2/> | |||
| During the microtubule based transport to the nucleus, the viral single strand RNA genome is transcribed into double strand DNA, which is then integrated into a host chromosome. | |||
| == Diagnosis == | |||
| HIV can infect ]s (DCs) by this CD4-CCR5 route, but another route using mannose-specific C-type lectin receptors such as ] can also be used.<ref name=Pope_2003>{{cite journal |author=Pope M, Haase A |title=Transmission, acute HIV-1 infection and the quest for strategies to prevent infection |journal=Nat Med |volume=9 |issue=7 |pages=847–52 |year=2003 |pmid=12835704 |doi=10.1038/nm0703-847}}</ref> DCs are one of the first cells encountered by the virus during sexual transmission. They are currently thought to play an important role by transmitting HIV to T cells once the virus has been captured in the ] by DCs.<ref name=Pope_2003 /> | |||
| {{Main|Diagnosis of HIV/AIDS}} | |||
| ] | |||
| Many HIV-positive people are unaware that they are infected with the virus.<ref name="Kumaranayake"> | |||
| ===Replication and transcription=== | |||
| Once the viral capsid enters the cell, an ] called '']'' liberates the single-stranded (+)] from the attached viral proteins and copies it into a complementary ].<ref name=Zheng>{{cite journal | |||
| | author=Zheng, Y. H., Lovsin, N. and Peterlin, B. M. | title=Newly identified host factors modulate HIV replication | journal=Immunol. Lett. | year=2005 | pages=225–34 | volume=97 | issue=2 | pmid=15752562 | doi=10.1016/j.imlet.2004.11.026}}</ref> This process of reverse transcription is extremely error-prone and it is during this step that mutations may occur. Such mutations may cause ]. The reverse transcriptase then makes a complementary DNA strand to form a double-stranded viral DNA intermediate (vDNA). This vDNA is then transported into the ]. The integration of the viral DNA into the host cell's ] is carried out by another viral enzyme called '']''.<ref name=Zheng/> | |||
| ] | |||
| This integrated viral DNA may then lie dormant, in the latent stage of HIV infection.<ref name=Zheng/> To actively produce the virus, certain cellular ]s need to be present, the most important of which is ] (NF kappa B), which is upregulated when T cells become activated.<ref name=Hiscott>{{cite journal | |||
| | author=Hiscott J, Kwon H, Genin P. | title=Hostile takeovers: viral appropriation of the NF-kappaB pathway | journal=J Clin Invest. | year=2001 | pages=143–151 | volume=107 | issue=2 | pmid=11160127 | doi=10.1172/JCI11918 | |||
| }}</ref> This means that those cells most likely to be killed by HIV are those currently fighting infection. | |||
| {{cite journal | vauthors = Kumaranayake L, Watts C | title = Resource allocation and priority setting of HIV/AIDS interventions: addressing the generalized epidemic in sub-Saharan Africa | journal = Journal of International Development | year = 2001 | pages = 451–466 | volume = 13 | issue = 4 | doi = 10.1002/jid.797}}</ref> For example, in 2001 less than 1% of the sexually active urban population in Africa had been tested, and this proportion is even lower in rural populations.<ref name="Kumaranayake" /> Furthermore, in 2001 only 0.5% of ] attending urban health facilities were counselled, tested or received their test results.<ref name="Kumaranayake" /> Again, this proportion is even lower in rural health facilities.<ref name="Kumaranayake" /> Since donors may therefore be unaware of their infection, ] and blood products used in medicine and ] are routinely screened for HIV.<ref name="Kleinman">{{cite web | author=Kleinman S | publisher=Uptodate | date=September 2004 | url=http://www.uptodate.com/patients/content/topic.do?topicKey=blod_dis/2419 | title=Patient information: Blood donation and transfusion | archive-url=https://web.archive.org/web/20080412115832/http://www.uptodate.com/patients/content/topic.do?topicKey=blod_dis%2F2419 | archive-date=April 12, 2008 | url-status=dead | df=mdy-all }}</ref> | |||
| In this replication process, the integrated ] is copied to ] which is then ] into smaller pieces. These small pieces produce the regulatory proteins ] (which encourages new virus production) and ]. As Rev accumulates it gradually starts to inhibit ] splicing.<ref name=Pollard> | |||
| HIV-1 testing is initially done using an ] (ELISA) to detect antibodies to HIV-1. Specimens with a non-reactive result from the initial ELISA are considered HIV-negative, unless new exposure to an infected partner or partner of unknown HIV status has occurred. Specimens with a reactive ELISA result are retested in duplicate.<ref name="CDC2001">{{cite journal |author=Centers for Disease Control and Prevention | title = Revised guidelines for HIV counseling, testing, and referral | journal = MMWR Recommendations and Reports | volume = 50 | issue = RR–19 | pages = 1–57 | year = 2001 | pmid = 11718472 }}</ref> If the result of either duplicate test is reactive, the specimen is reported as repeatedly reactive and undergoes confirmatory testing with a more specific supplemental test (e.g., a ] (PCR), ] or, less commonly, an ] (IFA)). Only specimens that are repeatedly reactive by ELISA and positive by IFA or PCR or reactive by western blot are considered HIV-positive and indicative of HIV infection. Specimens that are repeatedly ELISA-reactive occasionally provide an indeterminate western blot result, which may be either an incomplete antibody response to HIV in an infected person or nonspecific reactions in an uninfected person.<ref name="celum">{{cite journal | vauthors = Celum CL, Coombs RW, Lafferty W, Inui TS, Louie PH, Gates CA, McCreedy BJ, Egan R, Grove T, Alexander S | title = Indeterminate human immunodeficiency virus type 1 western blots: seroconversion risk, specificity of supplemental tests, and an algorithm for evaluation | journal = The Journal of Infectious Diseases | volume = 164 | issue = 4 | pages = 656–664 | year = 1991 | pmid = 1894929 | doi = 10.1093/infdis/164.4.656 }}</ref> | |||
| {{cite journal | |||
| | author=Pollard, V. W. and Malim, M. H. | title=The HIV-1 Rev protein | journal=Annu. Rev. Microbiol. | year=1998 | pages=491–532 | volume=52 | issue= | pmid=9891806 | doi=10.1146/annurev.micro.52.1.491 | |||
| {{Pie chart | |||
| }}</ref> At this stage, the structural proteins Gag and Env are produced from the full-length mRNA. The full-length RNA is actually the virus genome; it binds to the Gag protein and is packaged into new virus particles. | |||
| | caption= HIV deaths in 2014 excluding the U.S.:<ref>{{cite web |title=Country Comparison :: HIV/AIDS - Deaths |url=https://www.cia.gov/library/publications/the-world-factbook/rankorder/2157rank.html |publisher=The World Factbook, Central Intelligence Agency |access-date=November 22, 2015 |archive-date=April 30, 2017 |archive-url=https://web.archive.org/web/20170430003645/https://www.cia.gov/library/publications/the-world-factbook/rankorder/2157rank.html |url-status=dead }}</ref> | |||
| | other = yes | color = cyan | |||
| | label1 = ] | value1 = 15.76 | |||
| | color1 = silver | |||
| | label2 = ] | value2 = 12.51 | |||
| | color2 = #FF0000 | |||
| | label3 = ] | value3 = 11.50 | |||
| | color3 = #800080 | |||
| | label4 = ] | value4 = 4.169 | |||
| | color4 = #008000 | |||
| | label5 = ] | value5 = 4.061 | |||
| | color5 = #00058f | |||
| | label6 = ] | value6 = 3.49 | |||
| | color6 = #808000 | |||
| | label7 = ] | value7 = 3.09 | |||
| | color7 = #7953c1 | |||
| | label8= ] | value8 = 3.04 | |||
| | color8 = #FFA500 | |||
| | label9= ] | value9 = 2.98 | |||
| | color9 = #704045 | |||
| | label10= ] | value10 = 2.97 | |||
| | color10 = #536cb6 | |||
| | label11 = ] | value11 = 2.94 | |||
| | color11 = #5d2e68 | |||
| | label12 = ] | value12 = 2.17 | |||
| | color12 = #add2d5 | |||
| | label13 = ] | value13 = 2.11 | |||
| | color13 = #033e88 | |||
| }} | |||
| Although IFA can be used to confirm infection in these ambiguous cases, this assay is not widely used. In general, a second specimen should be collected more than a month later and retested for persons with indeterminate western blot results. Although much less commonly available, ]ing (e.g., viral RNA or proviral DNA amplification method) can also help diagnosis in certain situations.<ref name="CDC2001" /> In addition, a few tested specimens might provide inconclusive results because of a low quantity specimen. In these situations, a second specimen is collected and tested for HIV infection. | |||
| HIV-1 and HIV-2 appear to package their RNA differently; HIV-1 will bind to any appropriate RNA whereas HIV-2 will preferentially bind to the mRNA which was used to create the Gag protein itself. This may mean that HIV-1 is better able to mutate (HIV-1 infection progresses to AIDS faster than HIV-2 infection and is responsible for the majority of global infections). | |||
| Modern HIV testing is extremely accurate, when the ] is taken into consideration. A single screening test is correct more than 99% of the time.<ref>{{cite journal | vauthors = Chou R, Selph S, Dana T, Bougatsos C, Zakher B, Blazina I, Korthuis PT | title = Screening for HIV: systematic review to update the 2005 U.S. Preventive Services Task Force recommendation |s2cid-access=free |doi-access=free | journal = Annals of Internal Medicine | volume = 157 | issue = 10 | pages = 706–18 | date = November 2012 | pmid = 23165662 | doi = 10.7326/0003-4819-157-10-201211200-00007 | s2cid = 27494096 }}</ref> The chance of a false-positive result in a standard two-step testing protocol is estimated to be about 1 in 250,000 in a low risk population.<ref name="ScreenReview2005">{{cite journal | vauthors = Chou R, Huffman LH, Fu R, Smits AK, Korthuis PT | title = Screening for HIV: a review of the evidence for the U.S. Preventive Services Task Force |s2cid-access=free |doi-access=free | journal = Annals of Internal Medicine | volume = 143 | issue = 1 | pages = 55–73 | date = July 2005 | pmid = 15998755 | doi = 10.7326/0003-4819-143-1-200507050-00010 | author6 = US Preventive Services Task Force | s2cid = 24086322 }}</ref> Testing post-exposure is recommended immediately and then at six weeks, three months, and six months.<ref name="PEP10">{{cite journal | vauthors = Tolle MA, Schwarzwald HL | title = Postexposure prophylaxis against human immunodeficiency virus |url=https://www.aafp.org/pubs/afp/issues/2010/0715/p161.html | journal = American Family Physician | volume = 82 | issue = 2 | pages = 161–6 | date = July 2010 | pmid = 20642270 |url-status=live |archive-url=https://web.archive.org/web/20231128140702/https://www.aafp.org/pubs/afp/issues/2010/0715/p161.html |archive-date= Nov 28, 2023 }}</ref> | |||
| ===Assembly and release=== | |||
| The final step of the viral cycle, assembly of new HIV-1 virons, begins at the plasma membrane of the host cell. The Env polyprotein (gp160) goes through the ] and is transported to the ] complex where it is cleaved by ] and processed into the two HIV envelope glycoproteins gp41 and gp120. These are transported to the ] of the host cell where gp41 anchors the gp120 to the membrane of the infected cell. The Gag (p55) and Gag-Pol (p160) polyproteins also associate with the inner surface of the plasma membrane along with the HIV genomic RNA as the forming virion begins to bud from the host cell. Maturation either occurs in the forming bud or in the immature virion after it buds from the host cell. During maturation, HIV proteases cleave the polyproteins into individual functional HIV proteins and enzymes. The various structural components then assemble to produce a mature HIV virion.<ref name=Gelderblom>{{cite book | |||
| | last = Gelderblom | first = H. R | year = 1997 | title = '''HIV Sequence Compendium''' | chapter = Fine structure of HIV and SIV | chapterurl = http://www.hiv.lanl.gov/content/sequence/HIV/COMPENDIUM/1997/partIII/Gelderblom.pdf | editor = Los Alamos National Laboratory (ed.) | edition = | pages = 31-44 | publisher = ] | location = ] | format = ]}}</ref> This cleavage step can be inhibited by protease inhibitors. The mature virus is then able to infect another cell. | |||
| The latest recommendations of the US ] (CDC) show that HIV testing must start with an ] combination test for HIV-1 and HIV-2 ] and p24 ]. A negative result rules out HIV exposure, while a positive one must be followed by an HIV-1/2 antibody differentiation immunoassay to detect which antibodies are present. This gives rise to four possible scenarios: | |||
| ==Genetic variability== | |||
| * 1. HIV-1 (+) & HIV-2 (−): HIV-1 antibodies detected | |||
| {{See|Subtypes of HIV}} | |||
| * 2. HIV-1 (−) & HIV-2 (+): HIV-2 antibodies detected | |||
| ] of the SIV and HIV.]] | |||
| * 3. HIV-1 (+) & HIV-2 (+): both HIV-1 and HIV-2 antibodies detected | |||
| HIV differs from many viruses in that it has very high genetic variability. This diversity is a result of its fast ], with the generation of 10<sup>9</sup> to 10<sup>10</sup> virions every day, coupled with a high mutation rate of approximately 3 x 10<sup>-5</sup> per nucleotide base per cycle of replication and ] properties of reverse transcriptase.<ref name=RobertsonDL> | |||
| * 4. HIV-1 (−) or indeterminate & HIV-2 (−): ] must be carried out to detect the acute infection of HIV-1 or its absence.<ref name="cdc.gov">{{cite web|title=Quick Reference Guide—Laboratory Testing for the Diagnosis of HIV Infection: Updated Recommendations|url=https://www.cdc.gov/hiv/pdf/testingHIValgorithmQuickRef.pdf|website=Centers for Disease Control and Prevention |publisher=New York State Department of Health|access-date=April 13, 2017|pages=1–2|date=June 27, 2014|archive-url=https://web.archive.org/web/20170302175531/https://www.cdc.gov/hiv/pdf/testingHIValgorithmQuickRef.pdf|archive-date=March 2, 2017|url-status=dead}}</ref> | |||
| ==Research== | |||
| {{cite journal | |||
| | author=Robertson DL, Hahn BH, Sharp PM. | title=Recombination in AIDS viruses | journal=J Mol Evol. | year=1995 | pages=249–59 | volume=40 | issue=3 | pmid=7723052 | doi=10.1007/BF00163230 | |||
| {{Main|HIV/AIDS research}}HIV/AIDS research includes all ] that attempts to prevent, treat, or cure ], as well as fundamental research about the nature of HIV as an infectious agent and AIDS as the disease caused by HIV. | |||
| }}</ref> This complex scenario leads to the generation of many variants of HIV in a single infected patient in the course of one day.<ref name=RobertsonDL/> This variability is compounded when a single cell is simultaneously infected by two or more different strains of HIV. When simultaneous infection occurs, the genome of progeny virions may be composed of RNA strands from two different strains. This hybrid virion then infects a new cell where it undergoes replication. As this happens, the reverse transcriptase, by jumping back and forth between the two different RNA templates, will generate a newly synthesized retroviral DNA sequence that is a recombinant between the two parental genomes.<ref name=RobertsonDL/> This recombination is most obvious when it occurs between subtypes.<ref name=RobertsonDL/> | |||
| Many governments and research institutions participate in HIV/AIDS research. This research includes behavioral ], such as research into ], and ], such as research into ], ]s, and ]s.<ref>{{cite web |url=https://aidsinfo.nih.gov/education-materials/fact-sheets/21/58/fda-approved-hiv-medicines |title=HIV Treatment: FDA-Approved HIV Medicines |publisher=AIDSinfo |access-date=October 7, 2016 |archive-date=February 23, 2017 |archive-url=https://web.archive.org/web/20170223195011/https://aidsinfo.nih.gov/education-materials/fact-sheets/21/58/fda-approved-HIV-medicines |url-status=dead }}</ref> Other medical research areas include the topics of ], ], ], and ]. | |||
| The closely related ] (SIV) exhibits a somewhat different behavior: in its natural hosts, ]s and ]s, the retrovirus is present in high levels in the blood, but evokes only a mild immune response,<ref>{{cite journal |author=Holzammer S, Holznagel E, Kaul A, Kurth R, Norley S |title=High virus loads in naturally and experimentally SIVagm-infected African green monkeys |journal=Virology |volume=283 |issue=2 |pages=324–31 |year=2001 |pmid=11336557 |doi=10.1006/viro.2001.0870}}</ref> does not cause the development of simian AIDS,<ref>Kurth, R. and Norley, S. (1996) Why don't the natural hosts of SIV develop simian AIDS?, ''J. NIH Res.'' '''8''', 33-37.</ref> and does not undergo the extensive mutation and recombination typical of HIV.<ref>{{cite journal |author=Baier M, Dittmar MT, Cichutek K, Kurth R |title=Development of vivo of genetic variability of simian immunodeficiency virus |journal=Proc. Natl. Acad. Sci. U.S.A. |volume=88 |issue=18 |pages=8126–30 |year=1991 |pmid=1896460 |doi=}}</ref> By contrast, infection of heterologous hosts (rhesus or cynomologus macaques) with SIV results in the generation of genetic diversity that is on the same order as HIV in infected humans; these heterologous hosts also develop simian AIDS.<ref>{{cite journal |author=Daniel MD, King NW, Letvin NL, Hunt RD, Sehgal PK, Desrosiers RC |title=A new type D retrovirus isolated from macaques with an immunodeficiency syndrome |journal=Science |volume=223 |issue=4636 |pages=602–5 |year=1984 |pmid=6695172 |doi=10.1126/science.6695172}}</ref> The relationship, if any, between genetic diversification, immune response, and disease progression is unknown. | |||
| == Treatment and transmission== | |||
| Three groups of HIV-1 have been identified on the basis of differences in ''env'': M, N, and O.<ref name=Thomson> | |||
| {{Main|Management of HIV/AIDS}}{{See also|1=HIV/AIDS#Transmission|2=Undetectable = Untransmittable}} | |||
| The management of HIV/AIDS typically involves the use of multiple ]. In many parts of the world, HIV has become a chronic condition, with progression to ] increasingly rare. | |||
| ] and the resulting ] in CD4<sup>+</sup> T cells, dendritic cells, and macrophages is the main barrier to eradication of the virus.<ref name="HIV Latency" /><ref name="Rodari">{{cite journal |last1=Rodari |first1=Anthony |last2=Darcis |first2=Gilles |last3=Van Lint |first3=Carine M. |date=29 September 2021 |title=The Current Status of Latency Reversing Agents for HIV-1 Remission |journal=Annual Review of Virology |language=en |volume=8 |issue=1 |pages=491–514 |doi=10.1146/annurev-virology-091919-103029 |issn=2327-056X |pmid=34586875 |doi-access=free}}</ref> | |||
| {{cite journal | |||
| | author=Thomson, M. M., Perez-Alvarez, L. and Najera, R. | title=Molecular epidemiology of HIV-1 genetic forms and its significance for vaccine development and therapy | journal=Lancet Infect. Dis. | year=2002 | pages=461–471 | volume=2 | issue=8 | pmid=12150845 | doi=10.1016/S1473-3099(02)00343-2 | |||
| While HIV is highly virulent, transmission through sexual contact does not occur when an HIV-positive individual maintains a consistently undetectable ] (<50 copies/ml) due to antiretroviral treatment. This concept was first proposed by the Swiss Federal Commission for AIDS/HIV in 2008 in what is known as the ].<ref>{{cite web |author=Swiss National AIDS Commission |date=15 October 2016 |title=The Swiss statement |url=http://i-base.info/qa/factsheets/the-swiss-statement |access-date=2 April 2019 |publisher=]}}</ref><ref name="Vernazza&Bernard">{{cite journal |vauthors=Vernazza P, Bernard EJ |date=29 January 2016 |title=HIV is not transmitted under fully suppressive therapy: The Swiss Statement—eight years later |journal=] |volume=146 |pages=w14246 |doi=10.4414/smw.2016.14246 |pmid=26824882 |doi-access=free}}</ref> Although initially controversial, subsequent studies have confirmed that the risk of transmitting HIV through sex is effectively zero when the HIV-positive person has a consistently undetectable viral load, a concept now widely known as U=U, or "Undetectable = Untransmittable."<ref>{{cite journal |author=The Lancet HIV |date=November 2017 |title=U=U taking off in 2017 |department=Editorial |journal=The Lancet. HIV |volume=4 |issue=11 |pages=e475 |doi=10.1016/S2352-3018(17)30183-2 |pmid=29096785 |doi-access=free}}</ref><ref>{{cite web |year=2019 |title=Can't Pass It On |url=https://www.tht.org.uk/our-work/our-campaigns/cant-pass-it-on |url-status=live |archive-url=https://web.archive.org/web/20190407233322/https://www.tht.org.uk/our-work/our-campaigns/cant-pass-it-on |archive-date=7 April 2019 |access-date=2 April 2019 |publisher=]}}</ref> | |||
| }}</ref> Group M is the most prevalent and is subdivided into eight subtypes (or ]s), based on the whole genome, which are geographically distinct.<ref name=Carr>{{cite book | |||
| | last = Carr | first = J. K. | coauthors = Foley, B. T., Leitner, T., Salminen, M., Korber, B. and McCutchan, F. | year = 1998 | title = '''HIV Sequence Compendium''' | chapter = Reference Sequences Representing the Principal Genetic Diversity of HIV-1 in the Pandemic | chapterurl = http://www.hiv.lanl.gov/content/sequence/HIV/COMPENDIUM/1998/III/Carr.pdf | editor = Los Alamos National Laboratory (ed.) | edition = | pages = 10-19 | publisher = ] | location = ] | format=]}}</ref> The most prevalent are subtypes B (found mainly in North America and Europe), A and D (found mainly in Africa), and C (found mainly in Africa and Asia); these subtypes form branches in the phylogenetic tree representing the lineage of the M group of HIV-1. Coinfection with distinct subtypes gives rise to circulating recombinant forms (CRFs). In 2000, the last year in which an analysis of global subtype prevalence was made, 47.2 percent of infections worldwide were of subtype C, 26.7 percent were of subtype A/CRF02_AG, 12.3 percent were of subtype B, 5.3 percent were of subtype D, 3.2 percent were of CRF_AE, and the remaining 5.3 percent were composed of other subtypes and CRFs.<ref name=Osmanov> | |||
| Studies that established the U=U principle include Opposites Attract,<ref name="Opposites Attract">{{cite journal | vauthors = Bavinton BR, Pinto AN, Phanuphak N, Grinsztejn B, Prestage GP, Zablotska-Manos IB, Jin F, Fairley CK, Moore R, Roth N, Bloch M, Pell C, McNulty AM, Baker D, Hoy J, Tee BK, Templeton DJ, Cooper DA, Emery S, Kelleher A, Grulich AE | display-authors = 6 | title = Viral suppression and HIV transmission in serodiscordant male couples: an international, prospective, observational, cohort study | journal = The Lancet. HIV | volume = 5 | issue = 8 | pages = e438–e447 | date = August 2018 | pmid = 30025681 | doi = 10.1016/S2352-3018(18)30132-2 | s2cid = 51702998 }}</ref> PARTNER 1,<ref name="PARTNER1">{{cite journal | vauthors = Rodger AJ, Cambiano V, Bruun T, Vernazza P, Collins S, van Lunzen J, Corbelli GM, Estrada V, Geretti AM, Beloukas A, Asboe D, Viciana P, Gutiérrez F, Clotet B, Pradier C, Gerstoft J, Weber R, Westling K, Wandeler G, Prins JM, Rieger A, Stoeckle M, Kümmerle T, Bini T, Ammassari A, Gilson R, Krznaric I, Ristola M, Zangerle R, Handberg P, Antela A, Allan S, Phillips AN, Lundgren J | display-authors = 6 | title = Sexual Activity Without Condoms and Risk of HIV Transmission in Serodifferent Couples When the HIV-Positive Partner Is Using Suppressive Antiretroviral Therapy | journal = JAMA | volume = 316 | issue = 2 | pages = 171–81 | date = July 2016 | pmid = 27404185 | doi = 10.1001/jama.2016.5148 | doi-access = free }}</ref> PARTNER 2<ref name="PARTNER2-2019" /><ref name="PARTNER2">{{cite conference|last=Rodger |first= A. (for the PARTNER study group) |title=Risk of HIV transmission through condomless sex in MSM couples with suppressive ART: The PARTNER2 Study extended results in gay men |conference=AIDS2018: 22nd International AIDS Conference |location=Amsterdam, the Netherlands |date=July 2018 |url=https://programme.aids2018.org/Abstract/Abstract/13470 |access-date=2 April 2019}}</ref> (which focused on male-male couples),<ref name="Hoffman">{{cite press release |title=The science is clear: with HIV, undetectable equals untransmittable |date=10 January 2019 |publisher=] |url=https://www.nih.gov/news-events/news-releases/science-clear-hiv-undetectable-equals-untransmittable |quote=NIAID Director Anthony S. Fauci, M.D., and colleagues summarize results from large clinical trials and cohort studies validating U=U. The landmark NIH-funded HPTN 052 clinical trial showed that no linked HIV transmissions occurred among HIV serodifferent heterosexual couples when the partner living with HIV had a durably suppressed viral load. Subsequently, the PARTNER and Opposites Attract studies confirmed these findings and extended them to male-male couples. ... The success of U=U as an HIV prevention method depends on achieving and maintaining an undetectable viral load by taking ART daily as prescribed. |access-date=3 May 2019 |vauthors=Hoffman H |agency=]}}</ref> and ]<ref name="HPTN052">{{cite journal | vauthors = Cohen MS, Chen YQ, McCauley M, Gamble T, Hosseinipour MC, Kumarasamy N, Hakim JG, Kumwenda J, Grinsztejn B, Pilotto JH, Godbole SV, Chariyalertsak S, Santos BR, Mayer KH, Hoffman IF, Eshleman SH, Piwowar-Manning E, Cottle L, Zhang XC, Makhema J, Mills LA, Panchia R, Faesen S, Eron J, Gallant J, Havlir D, Swindells S, Elharrar V, Burns D, Taha TE, Nielsen-Saines K, Celentano DD, Essex M, Hudelson SE, Redd AD, Fleming TR | display-authors = 6 | title = Antiretroviral Therapy for the Prevention of HIV-1 Transmission | journal = The New England Journal of Medicine | volume = 375 | issue = 9 | pages = 830–9 | date = September 2016 | pmid = 27424812 | pmc = 5049503 | doi = 10.1056/NEJMoa1600693 | doi-access = free | author-link1 = Myron S. Cohen }}</ref> (which focused on heterosexual couples).<ref name="Hoffman" /> These studies involved couples where one partner was HIV-positive and one was HIV-negative, and included regular HIV testing. Across these four studies, a total of 4,097 couples participated from four continents, reporting 151,880 acts of condomless sex with zero phylogenetically-linked HIV transmissions when the positive partner had an undetectable viral load.<ref>{{cite conference | vauthors = Hodson M |title=U=U: Talking to patients about transmission risk |conference=British HIV Association Autumn Conference 2017 |date=17 November 2017 |url=https://www.bhiva.org/file/iGHaSOpwVeAQY/MatthewHodson.pdf |access-date=3 May 2019}} ( for presentation on behalf of ])</ref> Following these findings, the U=U consensus statement advocating the use of the term 'zero risk' was endorsed by numerous individuals and organizations, including the ], the ], and '']'' medical journal.<ref>{{cite web |publisher=] |title=Consensus statement: Risk of Sexual Transmission of HIV from a Person Living with HIV who has an Undetectable Viral Load |url=https://www.preventionaccess.org/consensus |date=21 July 2016 |access-date=2 April 2019}} '''Note''': When the statement and list of endorsements was retrieved, it had last been updated on 23 August 2018 and included "over 850 organizations from nearly 100 countries."</ref> | |||
| {{cite journal | |||
| | author=Osmanov S, Pattou C, Walker N, Schwardlander B, Esparza J; WHO-UNAIDS Network for HIV Isolation and Characterization. | title=Estimated global distribution and regional spread of HIV-1 genetic subtypes in the year 2000 | journal=Acquir. Immune. Defic. Syndr. | year=2002 | pages=184–190 | volume=29 | issue=2 | pmid=11832690 | |||
| Additionally, reactivation of ] (HSV-2) in individuals with ] is associated with an increase in ] enriched CD4<sup>+</sup> T cells and inflammatory dendritic cells in the dermis of ulcerated genital skin, persisting even after ulcer healing. HIV's tropism for CCR-5 positive cells contributes to the two- to threefold increased risk of HIV acquisition in persons with genital herpes. Notably, daily antiviral medication, such as ], does not reduce the subclinical post-reactivation inflammation and therefore does not decrease the risk of HIV acquisition.<ref>{{cite journal | vauthors = Zhu J, Hladik F, Woodward A, Klock A, Peng T, Johnston C, Remington M, Magaret A, Koelle DM, Wald A, Corey L | display-authors = 6 | title = Persistence of HIV-1 receptor-positive cells after HSV-2 reactivation is a potential mechanism for increased HIV-1 acquisition | journal = Nature Medicine | volume = 15 | issue = 8 | pages = 886–92 | date = August 2009 | pmid = 19648930 | pmc = 2723183 | doi = 10.1038/nm.2006 }}</ref><ref>{{cite journal | vauthors = Looker KJ, Elmes JA, Gottlieb SL, Schiffer JT, Vickerman P, Turner KM, Boily MC | title = Effect of HSV-2 infection on subsequent HIV acquisition: an updated systematic review and meta-analysis | journal = The Lancet. Infectious Diseases | volume = 17 | issue = 12 | pages = 1303–1316 | date = December 2017 | pmid = 28843576 | pmc = 5700807 | doi = 10.1016/S1473-3099(17)30405-X }}</ref> | |||
| }}</ref> Most HIV-1 research is focused on subtype B; few laboratories focus on the other subtypes.<ref name=Perrin> | |||
| ==History== | |||
| {{cite journal | |||
| <!--This section is the same as the one at HIV/AIDS. If you change one please change the other. --> | |||
| | author=Perrin L, Kaiser L, Yerly S. | title=Travel and the spread of HIV-1 genetic variants | journal=Lancet Infect Dis. | year=2003 | pages=22–27 | volume=3 | issue=1 | pmid=12505029 | doi=10.1016/S1473-3099(03)00484-5 | |||
| {{Main|History of HIV/AIDS}} | |||
| {{Further|Category:HIV/AIDS by country}} | |||
| ===Discovery=== | |||
| }}</ref> | |||
| {{multiple image | |||
| | total_width = 480 | |||
| | image1 = Françoise Barré-Sinoussi-press conference Dec 06th, 2008-1.jpg | |||
| | image2 = Gallo, Robert C. (3) (cropped).jpg | |||
| | image3 = Luc Montagnier-press conference Dec 06th, 2008-6.jpg | |||
| | footer = ], ], and ], co-discoverers of HIV | |||
| }} | |||
| The first news story on "an exotic new disease" appeared May 18, 1981, in the gay newspaper '']''.<ref>{{cite news|title=On this day|work=]|date=May 18, 2020|pages = 2A}}</ref> | |||
| AIDS was first clinically observed in 1981 in the United States.<ref name=M2010>{{cite book | veditors = Mandell GL, Bennett JE, Dolin R |title=Mandell, Douglas, and Bennett's principles and practice of infectious diseases |year=2010 |publisher=Churchill Livingstone/Elsevier |location=Philadelphia |isbn=978-0-443-06839-3 |chapter=Chapter 169 |edition=7th}}{{page needed|date=December 2017}}</ref> The initial cases were a cluster of injection drug users and gay men with no known cause of impaired immunity who showed symptoms of '']'' pneumonia (PCP or PJP, the latter term recognizing that the causative agent is now called ''Pneumocystis jirovecii''), a rare opportunistic infection that was known to occur in people with very compromised immune systems.<ref name=MMWR2>{{cite journal |vauthors=Gottlieb MS |title=Pneumocystis pneumonia—Los Angeles. 1981 |journal=American Journal of Public Health |volume=96 |issue=6 |pages=980–1; discussion 982–3 |year=2006 |pmid=16714472 |pmc=1470612 |doi=10.2105/AJPH.96.6.980 |url=https://www.cdc.gov/mmwr/preview/mmwrhtml/june_5.htm |archive-url=https://web.archive.org/web/20090422042240/http://www.cdc.gov/mmwr/preview/mmwrhtml/june_5.htm |url-status=live |archive-date=April 22, 2009 }}</ref> Soon thereafter, researchers at the ] studied gay men developing a previously rare skin cancer called ] (KS).<ref name="pmid7287964">{{cite journal |vauthors=Friedman-Kien AE |title=Disseminated Kaposi's sarcoma syndrome in young homosexual men |journal=Journal of the American Academy of Dermatology |volume=5 |issue=4 |pages=468–71 |date=October 1981 |pmid=7287964 |doi=10.1016/S0190-9622(81)80010-2 }}</ref><ref name="pmid6116083">{{cite journal |vauthors=Hymes KB, Cheung T, Greene JB, Prose NS, Marcus A, Ballard H, William DC, Laubenstein LJ |title=Kaposi's sarcoma in homosexual men — a report of eight cases |journal=The Lancet |volume=2 |issue=8247 |pages=598–600 |date=September 1981 |pmid=6116083 |doi=10.1016/S0140-6736(81)92740-9 |s2cid=43529542 }}</ref> Many more cases of PJP and KS emerged, alerting U.S. ] (CDC) and a CDC task force was formed to monitor the outbreak.<ref name="Basavapathruni_2007">{{cite journal |vauthors=Basavapathruni A, Anderson KS |title=Reverse transcription of the HIV-1 pandemic |journal=The FASEB Journal |volume=21 |issue=14 |pages=3795–3808 |date=December 2007 |pmid=17639073 |doi=10.1096/fj.07-8697rev |doi-access=free |s2cid=24960391 }}</ref> The earliest retrospectively described case of AIDS is believed to have been in Norway beginning in 1966.<ref>{{cite book | veditors = Lederberg J |title=Encyclopedia of Microbiology |date=2000 |publisher=Elsevier |location=Burlington |isbn=978-0-08-054848-7 |pages = 106 |edition=2nd |url=https://books.google.com/books?id=fhC_nz8eHh0C&pg=PA106 |access-date=9 June 2016}}</ref> | |||
| The genetic sequence of HIV-2 is only partially homologous to HIV-1 and more closely resembles that of SIV than HIV-1. | |||
| In the beginning, the CDC did not have an official name for the disease, often referring to it by way of the diseases that were associated with it, for example, ], the disease after which the discoverers of HIV originally named the virus.<ref name=MMWR1982a>{{cite journal |author=Centers for Disease Control |title=Persistent, generalized lymphadenopathy among homosexual males |journal=] |volume=31 |issue=19 |pages=249–251 |year=1982 |pmid=6808340 |url=https://www.cdc.gov/mmwr/preview/mmwrhtml/00001096.htm }}</ref><ref name="Montagnier">{{cite journal |vauthors=Barré-Sinoussi F, Chermann JC, Rey F, Nugeyre MT, Chamaret S, Gruest J, Dauguet C, Axler-Blin C, Vézinet-Brun F, Rouzioux C, Rozenbaum W, Montagnier L |title=Isolation of a T-lymphotropic retrovirus from a patient at risk for acquired immune deficiency syndrome (AIDS) |journal=] |volume=220 |issue=4599 |pages=868–871 |year=1983 |pmid=6189183 |doi=10.1126/science.6189183 |bibcode=1983Sci...220..868B |s2cid=390173 }}</ref> They also used ''Kaposi's Sarcoma and Opportunistic Infections'', the name by which a task force had been set up in 1981.<ref name=MMWR1982b>{{cite journal |author=Centers for Disease Control |title=Opportunistic infections and Kaposi's sarcoma among Haitians in the United States |journal=Morbidity and Mortality Weekly Report |volume=31 |issue=26 |pages=353–354; 360–361 |year=1982 |pmid=6811853 |url=https://www.cdc.gov/mmwr/preview/mmwrhtml/00001123.htm }}</ref> In the general press, the term ''GRID'', which stood for ], had been coined.<ref name=Altman>{{Cite news |author=Altman LK |url=https://www.nytimes.com/1982/05/11/science/new-homosexual-disorder-worries-health-officials.html |title=New homosexual disorder worries health officials |work=] |date=May 11, 1982 |access-date=August 31, 2011}}</ref> The CDC, in search of a name and looking at the infected communities, coined "the 4H disease", as it seemed to single out homosexuals, heroin users, ], and ]ans.<ref>{{cite journal |title=AIDS and Syphilis: The Iconography of Disease |journal=October |volume=43 |pages=87–107 | veditors = GilmanSL |year=1987 |jstor=3397566 | vauthors = Gilman SL |doi=10.2307/3397566 }}</ref><ref name=SciRep470b>{{cite web |publisher=] |date=July 28, 2006 |url=http://www.scienceonline.org/cgi/reprint/313/5786/470b.pdf |title=Making Headway Under Hellacious Circumstances |access-date=June 23, 2008 |archive-date=June 24, 2008 |archive-url=https://web.archive.org/web/20080624235131/http://www.scienceonline.org/cgi/reprint/313/5786/470b.pdf |url-status=dead }}</ref> However, after determining that AIDS was not isolated to the ],<ref name=MMWR1982b /> it was realized that the term GRID was misleading and ''AIDS'' was introduced at a meeting in July 1982.<ref name=Kher>{{Cite magazine |author=Kher U | title=A Name for the Plague| magazine=Time | date=July 27, 1982 |url=http://www.time.com/time/80days/820727.html |access-date=March 10, 2008| archive-url=https://web.archive.org/web/20080307015307/http://www.time.com/time/80days/820727.html| archive-date=March 7, 2008 | url-status= dead}}</ref> By September 1982 the CDC started using the name AIDS.<ref name=MMWR1982c>{{cite journal |author=Centers for Disease Control |title=Update on acquired immune deficiency syndrome (AIDS)—United States |journal=Morbidity and Mortality Weekly Report |volume=31 |issue=37 |pages=507–508; 513–514 |year=1982 |pmid=6815471 }}</ref> | |||
| ==The clinical course of infection== | |||
| [[Image:Hiv-timecourse.png|300px|thumb|right|A generalized graph of the relationship between HIV copies (viral load) and CD4 counts over the average course of untreated HIV infection; any particular individual's disease course may vary considerably. | |||
| {{legend-line|blue solid 2px|CD4<sup>+</sup> T cell count (cells per µL)}} | |||
| {{legend-line|red solid 2px|HIV RNA copies per mL of plasma}} | |||
| ]] | |||
| Infection with HIV-1 is associated with a progressive decrease of the CD4<SUP>+</SUP> T cell count and an increase in ]. The stage of infection can be determined by measuring the patient's CD4<SUP>+</SUP> T cell count, and the level of HIV in the blood. | |||
| In 1983, two separate research groups led by American ] and French investigators {{lang|fr|]|italic=no}} and ] independently declared that a novel retrovirus may have been infecting AIDS patients, and published their findings in the same issue of the journal '']''.<ref name="Gallo">{{cite journal |vauthors=Gallo RC, Sarin PS, Gelmann EP, Robert-Guroff M, Richardson E, Kalyanaraman VS, Mann D, Sidhu GD, Stahl RE, Zolla-Pazner S, Leibowitch J, Popovic M |title=Isolation of human T-cell leukemia virus in acquired immune deficiency syndrome (AIDS) |journal=] |volume=220 |issue=4599 |pages=865–867 |year=1983 |pmid=6601823 |doi=10.1126/science.6601823 |bibcode=1983Sci...220..865G }}</ref><ref name="Montagnier"/><ref>{{cite web |url=https://www.nobelprize.org/nobel_prizes/medicine/laureates/2008/press.html |title=The 2008 Nobel Prize in Physiology or Medicine - Press Release|website=www.nobelprize.org|access-date=2018-01-28}}</ref> Gallo claimed that a virus his group had isolated from a person with AIDS was strikingly similar in ] to other ]es (HTLVs) his group had been the first to isolate. Gallo admitted in 1987 that the virus he claimed to have discovered in 1984 was in reality a virus sent to him from France the year before.<ref>{{cite news | vauthors = Crewdson J |title=GALLO ADMITS FRENCH DISCOVERED AIDS VIRUS |url=https://www.chicagotribune.com/news/ct-xpm-1991-05-30-9102180196-story.html |access-date=25 April 2020 |publisher=Chicago Tribune |date=30 May 1991}}</ref> Gallo's group called their newly isolated virus HTLV-III. Montagnier's group isolated a virus from a patient presenting with swelling of the ]s of the neck and ], two classic symptoms of primary HIV infection. Contradicting the report from Gallo's group, Montagnier and his colleagues showed that core proteins of this virus were immunologically different from those of HTLV-I. Montagnier's group named their isolated virus lymphadenopathy-associated virus (LAV).<ref name="Basavapathruni_2007" /> As these two viruses turned out to be the same, in 1986 LAV and HTLV-III were renamed HIV.<ref>{{cite book | veditors = Aldrich R, Wotherspoon G |title=Who's who in gay and lesbian history |year=2001 |publisher=Routledge |location=London |isbn=978-0-415-22974-6 |pages = 154 |url=https://books.google.com/books?id=9KA7_1s6w-QC&pg=PA154 }}</ref> | |||
| HIV infection has basically four stages: incubation period, acute infection, latency stage and AIDS. The initial ] upon infection is ] and usually lasts between two and four weeks. The second stage, acute infection, which lasts an average of 28 days and can include symptoms such as ], ] (swollen lymph nodes), ] (sore throat), ], ] (muscle pain), ], and mouth and esophageal sores. The latency stage, which occurs third, shows few or no symptoms and can last anywhere from two weeks to twenty years and beyond. AIDS, the fourth and final stage of HIV infection shows as symptoms of various ]s. | |||
| Another group working contemporaneously with the Montagnier and Gallo groups was that of ] at the ]. He independently discovered the AIDS virus in 1983 and named it the AIDS associated retrovirus (ARV).<ref>{{cite journal |author=Levy JA |display-authors=etal |year=1984 |title=Isolation of lymphocytopathic retroviruses from San Francisco patients with AIDS |journal=Science |volume=225 |issue=4664 |pages=840–842 |doi=10.1126/science.6206563 |pmid=6206563 |bibcode=1984Sci...225..840L}}</ref> This virus was very different from the virus reported by the Montagnier and Gallo groups. The ARV strains indicated, for the first time, the heterogeneity of HIV isolates and several of these remain classic examples of the AIDS virus found in the United States.<ref>{{cite journal |vauthors=Levy JA, Kaminsky LS, Morrow WJ, Steimer K, Luciw P, Dina D, Hoxie J, Oshiro L |year=1985 |title=Infection by the retrovirus associated with the acquired immunodeficiency syndrome |journal=Annals of Internal Medicine |volume=103 |issue=5 |pages=694–699 |doi=10.7326/0003-4819-103-5-694 |pmid=2996401 }}</ref> | |||
| ===Acute HIV infection=== | |||
| {{Main|Acute HIV infection}} | |||
| The initial infection with HIV generally occurs after transfer of body fluids from an infected person to an uninfected one. The first stage of infection, the primary, or acute infection, is a period of rapid viral replication that immediately follows the individual's exposure to HIV leading to an abundance of virus in the peripheral blood with levels of HIV commonly approaching several million viruses per mL.<ref name=Piatak> | |||
| ===Origins=== | |||
| {{cite journal | author=Piatak, M., Jr, Saag, M. S., Yang, L. C., Clark, S. J., Kappes, J. C., Luk, K. C., Hahn, B. H., Shaw, G. M. and Lifson, J.D. | title=High levels of HIV-1 in plasma during all stages of infection determined by competitive PCR | journal=Science | year=1993 | pages=1749–1754 | volume=259 | issue=5102 | pmid=8096089 | doi=10.1126/science.8096089}} | |||
| Both HIV-1 and HIV-2 are believed to have originated in non-human ]s in West-central Africa, and are believed to have transferred to humans (a process known as ]) in the early 20th century.<ref name=Orgin2011>{{cite journal | vauthors = Sharp PM, Hahn BH | title = Origins of HIV and the AIDS Pandemic | journal = Cold Spring Harbor Perspectives in Medicine | volume = 1 | issue = 1 | pages = a006841 | year = 2011 | pmid = 22229120 | pmc = 3234451 | doi = 10.1101/cshperspect.a006841 }}</ref><ref name=Faria2014>{{cite journal | vauthors = Faria NR, Rambaut A, Suchard MA, Baele G, Bedford T, Ward MJ, Tatem AJ, Sousa JD, Arinaminpathy N, Pépin J, Posada D, Peeters M, Pybus OG, Lemey P | title = The early spread and epidemic ignition of HIV-1 in human populations | journal = Science | volume = 346 | issue = 6205 | pages = 56–61 | year = 2014 | pmid = 25278604| pmc = 4254776| doi = 10.1126/science.1256739 | bibcode = 2014Sci...346...56F }}</ref> | |||
| HIV-1 appears to have originated in southern ] through the evolution of SIVcpz, a ] (SIV) that infects wild ]s (HIV-1 descends from the SIVcpz endemic in the chimpanzee subspecies '']'').<ref name="pmid9989410">{{cite journal | vauthors = Gao F, Bailes E, Robertson DL, Chen Y, Rodenburg CM, Michael SF, Cummins LB, Arthur LO, Peeters M, Shaw GM, Sharp PM, Hahn BH | title = Origin of HIV-1 in the chimpanzee Pan troglodytes troglodytes | journal = Nature | volume = 397 | issue = 6718 | pages = 436–41 | year = 1999 | pmid = 9989410 | doi = 10.1038/17130 | bibcode = 1999Natur.397..436G | s2cid = 4432185 | doi-access = free }}</ref><ref name=Keele>{{cite journal | vauthors = Keele BF, Van Heuverswyn F, Li Y, Bailes E, Takehisa J, Santiago ML, Bibollet-Ruche F, Chen Y, Wain LV, Liegeois F, Loul S, Ngole EM, Bienvenue Y, Delaporte E, Brookfield JF, Sharp PM, Shaw GM, Peeters M, Hahn BH | title = Chimpanzee reservoirs of pandemic and nonpandemic HIV-1 | journal = Science | volume = 313 | issue = 5786 | pages = 523–6 | year = 2006 | pmid = 16728595 | pmc = 2442710 | doi = 10.1126/science.1126531 | bibcode = 2006Sci...313..523K }}</ref> The closest relative of HIV-2 is SIVsmm, a virus of the ] (''Cercocebus atys atys''), an ] living in littoral West Africa (from southern ] to western ]).<ref name=Reeves /> ]s such as the ] are resistant to HIV-1 infection, possibly because of a ] of two viral resistance genes.<ref name=Goodier>{{cite journal | vauthors = Goodier JL, Kazazian HH | title = Retrotransposons revisited: the restraint and rehabilitation of parasites | journal = Cell | volume = 135 | issue = 1 | pages = 23–35 | year = 2008 | pmid = 18854152 | doi = 10.1016/j.cell.2008.09.022 | s2cid = 3093360 | doi-access = free }}</ref> | |||
| </ref> This response is accompanied by a marked drop in the numbers of circulating CD4<sup>+</sup> T cells. This acute viremia is associated in virtually all patients with the activation of ], which kill HIV-infected cells, and subsequently with antibody production, or ]. The CD8<sup>+</sup> T cell response is thought to be important in controlling virus levels, which peak and then decline, as the CD4<sup>+</sup> T cell counts rebound to around 800 cells per µL (the normal ] is 1200 cells per µL ). A good CD8<sup>+</sup> T cell response has been linked to slower disease progression and a better prognosis, though it does not eliminate the virus.<ref name=Pantaleo1998> | |||
| HIV-1 is thought to have jumped the species barrier on at least three separate occasions, giving rise to the three groups of the virus, M, N, and O.<ref name="Sharp2001">{{cite journal | vauthors = Sharp PM, Bailes E, Chaudhuri RR, Rodenburg CM, Santiago MO, Hahn BH | title = The origins of acquired immune deficiency syndrome viruses: where and when? | journal = Philosophical Transactions of the Royal Society B | volume = 356 | issue = 1410 | pages = 867–76 | year = 2001 | pmid = 11405934 | pmc = 1088480 | doi = 10.1098/rstb.2001.0863 }}</ref> | |||
| {{cite journal | |||
| | author=Pantaleo G, Demarest JF, Schacker T, Vaccarezza M, Cohen OJ, Daucher M, Graziosi C, Schnittman SS, Quinn TC, Shaw GM, Perrin L, Tambussi G, Lazzarin A, Sekaly RP, Soudeyns H, Corey L, Fauci AS. | title=The qualitative nature of the primary immune response to HIV infection is a prognosticator of disease progression independent of the initial level of plasma viremia | journal=Proc Natl Acad Sci U S A. | year=1997 | pages=254–258 | volume=94 | issue=1 | pmid=8990195 | doi=10.1073/pnas.94.1.254 | |||
| ] source of ], the ] source of ], and the chimpanzee source of ]]] | |||
| }}</ref> During this period (usually 2-4 weeks post-exposure) most individuals (80 to 90%) develop an influenza or mononucleosis-like illness called ], the most common symptoms of which may include ], ], ], ], ], ], mouth and esophagal sores, and may also include, but less commonly, ], ] and ], enlarged liver/spleen, ], ], and neurological symptoms. Infected individuals may experience all, some, or none of these symptoms. The duration of symptoms varies, averaging 28 days and usually lasting at least a week.<ref name=Kahn> | |||
| There is evidence that humans who participate in ] activities, either as hunters or as bushmeat vendors, commonly acquire SIV.<ref name=Kalish2005>{{cite journal | vauthors = Kalish ML, Wolfe ND, Ndongmo CB, McNicholl J, Robbins KE, Aidoo M, Fonjungo PN, Alemnji G, Zeh C, Djoko CF, Mpoudi-Ngole E, Burke DS, Folks TM | title = Central African hunters exposed to simian immunodeficiency virus | journal = Emerging Infectious Diseases | volume = 11 | issue = 12 | pages = 1928–30 | year = 2005 | pmid = 16485481 | pmc = 3367631 | doi = 10.3201/eid1112.050394 }}</ref> However, SIV is a weak virus, and it is typically suppressed by the human immune system within weeks of infection. It is thought that several transmissions of the virus from individual to individual in quick succession are necessary to allow it enough time to mutate into HIV.<ref name=Marx2001>{{cite journal | vauthors = Marx PA, Alcabes PG, Drucker E | title = Serial human passage of simian immunodeficiency virus by unsterile injections and the emergence of epidemic human immunodeficiency virus in Africa | journal = Philosophical Transactions of the Royal Society B | volume = 356 | issue = 1410 | pages = 911–20 | year = 2001 | pmid = 11405938 | pmc = 1088484 | doi = 10.1098/rstb.2001.0867 }}</ref> Furthermore, due to its relatively low person-to-person transmission rate, it can only spread throughout the population in the presence of one or more high-risk transmission channels, which are thought to have been absent in Africa prior to the 20th century. | |||
| Specific proposed high-risk transmission channels, allowing the virus to adapt to humans and spread throughout the society, depend on the proposed timing of the animal-to-human crossing. Genetic studies of the virus suggest that the most recent common ancestor of the HIV-1 M group dates back to {{Circa|1910}}.<ref name=Worobey2008>{{cite journal | vauthors = Worobey M, Gemmel M, Teuwen DE, Haselkorn T, Kunstman K, Bunce M, Muyembe JJ, Kabongo JM, Kalengayi RM, Van Marck E, Gilbert MT, Wolinsky SM | title = Direct evidence of extensive diversity of HIV-1 in Kinshasa by 1960 | journal = Nature | volume = 455 | issue = 7213 | pages = 661–4 | year = 2008 | pmid = 18833279 | pmc = 3682493 | doi = 10.1038/nature07390 | bibcode = 2008Natur.455..661W }}</ref> Proponents of this dating link the HIV epidemic with the emergence of ] and growth of large colonial African cities, leading to social changes, including different patterns of sexual contact (especially multiple, concurrent partnerships), the spread of ], and the concomitant high frequency of ] diseases (such as ]) in nascent colonial cities.<ref name=Sousa2010>{{cite journal | vauthors = de Sousa JD, Müller V, Lemey P, Vandamme AM | title = High GUD incidence in the early 20th century created a particularly permissive time window for the origin and initial spread of epidemic HIV strains | journal = PLOS ONE | volume = 5 | issue = 4 | pages = e9936 | year = 2010 | pmid = 20376191 | pmc = 2848574 | doi = 10.1371/journal.pone.0009936 | veditors = Martin DP | bibcode = 2010PLoSO...5.9936S | doi-access = free }}</ref> While transmission rates of HIV during vaginal intercourse are typically low, they are increased manyfold if one of the partners has a ] resulting in genital ulcers. Early 1900s colonial cities were notable for their high prevalence of prostitution and genital ulcers to the degree that as of 1928 as many as 45% of female residents of eastern ] were thought to have been prostitutes and as of 1933 around 15% of all residents of the same city were infected by one of the forms of ].<ref name=Sousa2010 /> | |||
| {{cite journal | |||
| | author=Kahn, J. O. and Walker, B. D. | title=Acute Human Immunodeficiency Virus type 1 infection | journal=N. Engl. J. Med. | year=1998 | pages=33–39 | volume=331 | issue=1 | pmid=9647878 | doi=10.1056/NEJM199807023390107 | |||
| The earliest, well-documented case of HIV in a human dates back to 1959 in the ].<ref name=Zhu>{{cite journal | vauthors = Zhu T, Korber BT, Nahmias AJ, Hooper E, Sharp PM, Ho DD | title = An African HIV-1 Sequence from 1959 and Implications for the Origin of the epidemic | journal = Nature | volume = 391 | issue = 6667 | pages = 594–7 | year = 1998 | pmid = 9468138 | doi = 10.1038/35400 | bibcode = 1998Natur.391..594Z | s2cid = 4416837 | doi-access = free }}</ref> The virus may have been present in the United States as early as the mid- to late 1960s, as a sixteen-year-old male named ] presented with symptoms in 1966 and died in 1969.<ref>{{cite news| vauthors = Kolata G |title=Boy's 1969 death suggests AIDS invaded U.S. several times|work=] |date=October 28, 1987 |url=https://query.nytimes.com/gst/fullpage.html?res=9B0DEFD6173AF93BA15753C1A961948260 |access-date=February 11, 2009}}</ref> | |||
| }}</ref> Because of the nonspecific nature of these symptoms, they are often not recognized as signs of HIV infection. Even if patients go to their doctors or a hospital, they will often be misdiagnosed as having one of the more common infectious diseases with the same symptoms. Consequently, these primary symptoms are not used to diagnose HIV infection as they do not develop in all cases and because many are caused by other more common diseases. However, recognizing the syndrome can be important because the patient is much more infectious during this period.<ref name="pmid11187417">{{cite journal |author=Daar ES, Little S, Pitt J, ''et al'' |title=Diagnosis of primary HIV-1 infection. Los Angeles County Primary HIV Infection Recruitment Network |journal=Ann. Intern. Med. |volume=134 |issue=1 |pages=25–9 |year=2001 |pmid=11187417 |doi=}}</ref> | |||
| An alternative and likely complementary hypothesis points to the widespread use of unsafe medical practices in Africa during years following World War II, such as unsterile reuse of single-use syringes during mass vaccination, antibiotic, and anti-malaria treatment campaigns.<ref name=Marx2001 /><ref name="Chitnis2000">{{cite journal | vauthors = Chitnis A, Rawls D, Moore J | title = Origin of HIV type 1 in colonial French Equatorial Africa? | journal = AIDS Research and Human Retroviruses | volume = 16 | issue = 1 | pages = 5–8 | date = January 2000 | pmid = 10628811 | doi = 10.1089/088922200309548 | s2cid = 17783758 }}</ref><ref name="McNeil">{{cite news|first=Donald Jr. |last=McNeil|author-link=Donald McNeil, Jr|date=September 16, 2010|title=Precursor to H.I.V. was in monkeys for millennia|work=]|url=https://www.nytimes.com/2010/09/17/health/17aids.html |archive-url=https://ghostarchive.org/archive/20220103/https://www.nytimes.com/2010/09/17/health/17aids.html |archive-date=2022-01-03 |url-access=subscription |url-status=live|access-date=September 17, 2010|quote=Dr. Marx believes that the crucial event was the introduction into Africa of millions of inexpensive, mass-produced syringes in the 1950s. ... suspect that the growth of colonial cities is to blame. Before 1910, no Central African town had more than 10,000 people. But urban migration rose, increasing sexual contacts and leading to red-light districts.}}{{cbignore}}</ref> Research on the timing of most recent common ancestor for HIV-1 groups M and O, as well as on HIV-2 groups A and B, indicates that SIV has given rise to transmissible HIV lineages throughout the twentieth century.<ref name=":0">{{cite journal | vauthors = Wertheim JO, Worobey M | title = Dating the age of the SIV lineages that gave rise to HIV-1 and HIV-2 | journal = PLOS Computational Biology | volume = 5 | issue = 5 | pages = e1000377 | date = May 2009 | pmid = 19412344 | pmc = 2669881 | doi = 10.1371/journal.pcbi.1000377 | bibcode = 2009PLSCB...5E0377W | doi-access = free }}</ref> The dispersed timing of these transmissions to humans implies that no single external factor is needed to explain the cross-species transmission of HIV. This observation is consistent with both of the two prevailing views of the origin of the HIV epidemics, namely SIV transmission to humans during the slaughter or butchering of infected primates, and the colonial expansion of sub-Saharan African cities.<ref name=":0" /> | |||
| ===Latency stage=== | |||
| A strong immune defense reduces the number of viral particles in the blood stream, marking the start of the infection's ''clinical latency'' stage. Clinical latency can vary between two weeks and 20 years. During this early phase of infection, HIV is active within ], where large amounts of virus become trapped in the follicular ]s (FDC) network.<ref name=burton> | |||
| == See also == | |||
| {{cite journal | |||
| {{Portal|Medicine|Viruses}} | |||
| | author=Burton GF, Keele BF, Estes JD, Thacker TC, Gartner S. | title=Follicular dendritic cell contributions to HIV pathogenesis | journal=Semin Immunol. | year=2002 | pages=275–284 | volume=14 | issue=4 | pmid=12163303 | doi=10.1016/S1044-5323(02)00060-X | |||
| * ] | |||
| * ] | |||
| * ] | |||
| * ] | |||
| * ] | |||
| == References == | |||
| }}</ref> The surrounding tissues that are rich in CD4<SUP>+</SUP> T cells may also become infected, and viral particles accumulate both in infected cells and as free virus. Individuals who are in this phase are still infectious. During this time, ] carry most of the proviral load.<ref name=clapham> | |||
| {{Reflist|32em}} | |||
| == Further reading == | |||
| {{cite journal | |||
| {{Refbegin}} | |||
| | author=Clapham PR, McKnight A. | title=HIV-1 receptors and cell tropism | journal=Br Med Bull. | year=2001 | pages=43–59 | volume=58 | issue=4 | pmid=11714623 | doi=10.1093/bmb/58.1.43 | |||
| * {{cite journal | vauthors = Berlier W, Bourlet T, Lawrence P, Hamzeh H, Lambert C, Genin C, Verrier B, Dieu-Nosjean MC, Pozzetto B, Delézay O | title = Selective sequestration of X4 isolates by human genital epithelial cells: Implication for virus tropism selection process during sexual transmission of HIV | journal = Journal of Medical Virology | volume = 77 | issue = 4 | pages = 465–74 | year = 2005 | pmid = 16254974 | doi = 10.1002/jmv.20478 | s2cid = 25762969 }} | |||
| * {{cite book|author=] (UNAIDS) |title=Global HIV/AIDS Response, Epidemic update and health sector progress towards universal access|year=2011|publisher=Joint United Nations Programme on HIV/AIDS|url=http://www.unaids.org/en/media/unaids/contentassets/documents/unaidspublication/2011/20111130_UA_Report_en.pdf}} | |||
| * {{cite journal | vauthors = Muciaccia B, Padula F, Vicini E, Gandini L, Lenzi A, Stefanini M | title = Beta-chemokine receptors 5 and 3 are expressed on the head region of human spermatozoon | journal = The FASEB Journal | volume = 19 | issue = 14 | pages = 2048–50 | year = 2005 | pmid = 16174786 | doi = 10.1096/fj.05-3962fje | doi-access = free | hdl = 11573/361629 | s2cid = 7928126 }} | |||
| {{Refend}} | |||
| == External links == | |||
| }}</ref> | |||
| {{Sister project links|b=Sexual Health/Sexually Transmitted Diseases#HIV|commons=Category:HIV|n=Category:AID|s=no|q=no|v=no}} | |||
| <!--======================== {{No more links}} ============================ | |||
| | PLEASE BE CAUTIOUS IN ADDING MORE LINKS TO THIS ARTICLE. Misplaced Pages | | |||
| | is not a collection of links nor should it be used for advertising. | | |||
| | | | |||
| | Excessive or inappropriate links WILL BE DELETED. | | |||
| | See ] & ] for details. | | |||
| | | | |||
| | If there are already plentiful links, please propose additions or | | |||
| | replacements on this article's discussion page, or submit your link | | |||
| | to the relevant category at the "long dead (2017)" Open Directory Project (dmoz.org) | | |||
| | and link back to that category using the {{dmoz}} template. | | |||
| ======================== {{No more links}} ============================ --> | |||
| {{HIV and AIDS}} | |||
| {{ |
{{STD and STI}} | ||
| {{Retroviruses}} | |||
| :''For more details on this topic, see ], ] and ]'' | |||
| {{Breakthrough of the Year}} | |||
| When CD4<sup>+</sup> T cell numbers decline below a critical level, cell-mediated immunity is lost, and infections with a variety of opportunistic ]s appear. The first symptoms often include moderate and unexplained weight loss, recurring ] infections (such as ], ], ], ]), ], skin rashes, and oral ulcerations. Common opportunistic infections and tumors, most of which are normally controlled by robust CD4<sup>+</sup> T cell-mediated immunity then start to affect the patient. Typically, resistance is lost early on to oral Candida species and to ''Mycobacterium tuberculosis'', which leads to an increased susceptibility to ] (thrush) and ]. Later, reactivation of latent ] may cause worsening recurrences of ] eruptions, ], ]-induced B-cell lymphomas, or ], a ] of ]s that occurs when HIV proteins such as Tat interact with ]. Pneumonia caused by the fungus '']'' is common and often fatal. In the final stages of AIDS, infection with ] (another herpes virus) or ] is more prominent. Not all patients with AIDS get all these infections or tumors, and there are other tumors and infections that are less prominent but still significant. | |||
| {{Taxonbar|from=Q15787}} | |||
| {{Authority control}} | |||
| {{DEFAULTSORT:Hiv}} | |||
| ==HIV test== | |||
| ] | |||
| {{main|HIV test}} | |||
| ] | |||
| Many HIV-positive people are unaware that they are infected with the virus.<ref name=Kumaranayake> | |||
| ] | |||
| ] | |||
| {{cite journal | |||
| ] | |||
| | author=Kumaranayake, L. and Watts, C. | title=Resource allocation and priority setting of HIV/AIDS interventions: addressing the generalized epidemic in sub-Saharan Africa | journal=J. Int. Dev. | year=2001 | pages=451–466 | volume=13 | issue=4 | doi = 10.1002/jid.797 | |||
| }}</ref> For example, less than 1% of the sexually active urban population in Africa have been tested and this proportion is even lower in rural populations.<ref name=Kumaranayake /> Furthermore, only 0.5% of pregnant women attending urban health facilities are counselled, tested or receive their test results.<ref name=Kumaranayake/> Again, this proportion is even lower in rural health facilities.<ref name=Kumaranayake/> Since donors may therefore be unaware of their infection, donor blood and blood products used in medicine and medical research are routinely screened for HIV.<ref name=Kleinman>{{ | |||
| cite web | |||
| | author=Kleinman, S. | publisher=Uptodate | |||
| | year=2004 |month=September | year=2004 | |||
| | url=http://www.uptodate.com/patients/content/topic.do?topicKey=blod_dis/2419 | |||
| | title=Patient information: Blood donation and transfusion | |||
| | accessdate=2008-04-03 | |||
| }}</ref> | |||
| HIV-1 testing consists of initial screening with an ] (ELISA) to detect antibodies to HIV-1. Specimens with a nonreactive result from the initial ELISA are considered HIV-negative unless new exposure to an infected partner or partner of unknown HIV status has occurred. Specimens with a reactive ELISA result are retested in duplicate.<ref name=CDC2001> | |||
| {{cite journal | |||
| | author=Centers for Disease Control and Prevention. | title=Revised guidelines for HIV counseling, testing, and referral | journal=MMWR Recomm Rep. | year=2001 | pages=1–57 | volume=50 | issue=RR-19 | pmid=11718472 | |||
| }}</ref> If the result of either duplicate test is reactive, the specimen is reported as repeatedly reactive and undergoes confirmatory testing with a more specific supplemental test (e.g., ] or, less commonly, an ] (IFA)). Only specimens that are repeatedly reactive by ELISA and positive by IFA or reactive by Western blot are considered HIV-positive and indicative of HIV infection. Specimens that are repeatedly ELISA-reactive occasionally provide an indeterminate Western blot result, which may be either an incomplete antibody response to HIV in an infected person, or nonspecific reactions in an uninfected person.<ref name=celum> | |||
| {{cite journal | |||
| | author=Celum CL, Coombs RW, Lafferty W, Inui TS, Louie PH, Gates CA, McCreedy BJ, Egan R, Grove T, Alexander S, et al. | title=Indeterminate human immunodeficiency virus type 1 western blots: seroconversion risk, specificity of supplemental tests, and an algorithm for evaluation | journal=J Infect Dis. | year=1991 | pages=656–664 | volume=164 | issue=4 | pmid=1894929 | |||
| }}</ref> Although IFA can be used to confirm infection in these ambiguous cases, this assay is not widely used. Generally, a second specimen should be collected more than a month later and retested for persons with indeterminate Western blot results. Although much less commonly available, nucleic acid testing (e.g., viral RNA or proviral DNA amplification method) can also help diagnosis in certain situations.<ref name=CDC2001 /> In addition, a few tested specimens might provide inconclusive results because of a low quantity specimen. In these situations, a second specimen is collected and tested for HIV infection. | |||
| ==Treatment== | |||
| :''See also ]'' | |||
| ]'' - a nucleoside analog reverse transcriptase inhibitors (NARTIs or NRTIs)]] | |||
| There is currently no ] or cure for HIV or AIDS. The only known method of prevention is avoiding exposure to the virus. However, a course of antiretroviral treatment administered immediately after exposure, referred to as ], is believed to reduce the risk of infection if begun as quickly as possible.<ref name=Fan>{{cite book | |||
| | author = | year = 2005 | title = '''AIDS : science and society''' | chapter = | chapterurl = | editor = Fan, H., Conner, R. F. and Villarreal, L. P. eds | edition = 4th edition | pages = | publisher = Jones and Bartlett Publishers | location = ] | id = ISBN 0-7637-0086-X}}</ref> Current treatment for HIV infection consists of ], or HAART.<ref name=DhhsHivTreatment>{{ cite web | author=] | publisher= | month=January | year=2005 | url=http://www.hab.hrsa.gov/tools/HIVpocketguide05/PktGARTtables.htm | title=A Pocket Guide to Adult HIV/AIDS Treatment January 2005 edition | accessdate=2006-01-17}}</ref> This has been highly beneficial to many HIV-infected individuals since its introduction in 1996, when the protease inhibitor-based HAART initially became available.<ref name=Pallelal>{{ cite journal | author=Palella, F. J., Delaney, K. M., Moorman, A. C., Loveless, M. O., Fuhrer, J., Satten, G. A., Aschman, D. J. and Holmberg, S. D. | title=Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection | journal=N. Engl. J. Med. | year=1998 | pages=853–860 | volume=338 | issue=13 | pmid=9516219 | doi=10.1056/NEJM199803263381301}}</ref> | |||
| Current HAART options are combinations (or "cocktails") consisting of at least three drugs belonging to at least two types, or "classes," of ] agents. Typically, these classes are two ]s (NARTIs or NRTIs) plus either a ] or a ] (NNRTI). New classes of drugs such as ] provide treatment options for patients who are infected with viruses already resistant to common therapies, although they are not widely available and not typically accessible in resource-limited settings. | |||
| Because AIDS progression in children is more rapid and less predictable than in adults, particularly in young infants, more aggressive treatment is recommended for children than adults.<ref name=2005dhhsHivChildren>{{ cite web | author=] Working Group on Antiretroviral Therapy and Medical Management of HIV-Infected Children | publisher= | date=November 3, 2005 | url=http://www.aidsinfo.nih.gov/ContentFiles/PediatricGuidelines_PDA.pdf | title=Guidelines for the Use of Antiretroviral Agents in Pediatric HIV Infection | format= PDF | accessdate=2006-01-17}}</ref> In developed countries where HAART is available, doctors assess their patients thoroughly: measuring the ], how fast CD4 declines, and patient readiness. They then decide when to recommend starting treatment.<ref name=2005DhhsHivTreatment>{{ cite web | author=] Panel on Clinical Practices for Treatment of HIV Infection | publisher= | date=October 6, 2005 | url=http://aidsinfo.nih.gov/ContentFiles/AdultandAdolescentGL.pdf | title=Guidelines for the Use of Antiretroviral Agents in HIV-1-Infected Adults and Adolescents | format= PDF | accessdate=2006-01-17}}</ref> | |||
| HAART neither cures the patient nor does it uniformly remove all symptoms; high levels of HIV-1, often HAART resistant, return if treatment is stopped.<ref name=martinez>{{ cite journal | author=Martinez-Picado, J., DePasquale, M. P., Kartsonis, N., Hanna, G. J., Wong, J., Finzi, D., Rosenberg, E., Gunthard, H.F., Sutton, L., Savara, A., Petropoulos, C. J., Hellmann, N., Walker, B. D., Richman, D. D., Siliciano, R. and D'Aquila, R. T. | title=Antiretroviral resistance during successful therapy of human immunodeficiency virus type 1 infection | journal=Proc. Natl. Acad. Sci. U. S. A. | year=2000 | pages=10948–10953 | volume=97 | issue=20 | pmid=11005867 | doi=10.1073/pnas.97.20.10948}}</ref><ref name=Dybul>{{ cite journal | author=Dybul, M., Fauci, A. S., Bartlett, J. G., Kaplan, J. E., Pau, A. K.; Panel on Clinical Practices for Treatment of HIV. | title=Guidelines for using antiretroviral agents among HIV-infected adults and adolescents | journal=Ann. Intern. Med. | year=2002 | pages=381–433 | volume=137 | issue=5 Pt 2 | pmid=12617573}}</ref> Moreover, it would take more than a lifetime for HIV infection to be cleared using HAART.<ref name=blankson>{{ cite journal | author=Blankson, J. N., Persaud, D., Siliciano, R. F. | title=The challenge of viral reservoirs in HIV-1 infection |journal=Annu. Rev. Med. | year=2002 | pages=557–593 | volume=53 | issue= | pmid=11818490 | doi=10.1146/annurev.med.53.082901.104024}}</ref> Despite this, many HIV-infected individuals have experienced remarkable improvements in their general health and quality of life, which has led to a large reduction in HIV-associated ] and mortality in the developed world.<ref name=Pallelal>{{ | |||
| cite journal | |||
| | author=Palella, F. J., Delaney, K. M., Moorman, A. C., Loveless, M. O., Fuhrer, J., Satten, G. A., Aschman, D. J. and Holmberg, S. D. | title=Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection | journal=N. Engl. J. Med. | year=1998 | pages=853-860 | volume=338 | issue=13 | pmid=9516219 | |||
| }}</ref><ref name=Wood>{{ | |||
| cite journal | |||
| | author=Wood, E., Hogg, R. S., Yip, B., Harrigan, P. R., O'Shaughnessy, M. V. and Montaner, J. S. | |||
| | title=Is there a baseline CD4 cell count that precludes a survival response to modern antiretroviral therapy? | |||
| | journal=AIDS | year=2003 | pages=711-720 | volume=17 | issue=5 | |||
| | pmid=12646794 | |||
| }}</ref><ref name=Chene>{{ | |||
| cite journal | |||
| | author=Chene, G., Sterne, J. A., May, M., Costagliola, D., Ledergerber, B., Phillips, A. N., Dabis, F., Lundgren, J., D'Arminio Monforte, A., de Wolf, F., Hogg, R., Reiss, P., Justice, A., Leport, C., Staszewski, S., Gill, J., Fatkenheuer, G., Egger, M. E. and the Antiretroviral Therapy Cohort Collaboration. | |||
| | title=Prognostic importance of initial response in HIV-1 infected patients starting potent antiretroviral therapy: analysis of prospective studies | |||
| | journal=Lancet | year=2003 | pages=679-686 | volume=362 | issue=9385 | |||
| | pmid=12957089 | |||
| }}</ref> One study suggests the average life expectancy of an HIV infected individual is 32 years from the time of infection if treatment is started when the CD4 count is 350/µL.<ref name=schack> A computer based study in 2006, following the 2004 United States treatment guidelines: {{ | |||
| cite journal | |||
| | author=Schackman BR, Gebo KA, Walensky RP, Losina E, Muccio T, Sax PE, Weinstein MC, Seage GR 3rd, Moore RD, Freedberg KA. | |||
| | title=The lifetime cost of current HIV care in the United States | |||
| | journal=Med Care | year=2006 | pages=990-997 | volume=44 | issue=11 | |||
| | pmid=17063130 | |||
| }}</ref> In the absence of HAART, progression from HIV infection to AIDS has been observed to occur at a ] of between nine to ten years and the median survival time after developing AIDS is only 9.2 months.<ref name=Morgan2 /> However, HAART sometimes achieves far less than optimal results, in some circumstances being effective in less than fifty percent of patients. This is due to a variety of reasons such as medication intolerance/side effects, prior ineffective antiretroviral therapy and infection with a drug-resistant strain of HIV. However, non-adherence and non-persistence with antiretroviral therapy is the major reason most individuals fail to benefit from HAART.<ref name=becker>{{ | |||
| cite journal | |||
| | author=Becker SL, Dezii CM, Burtcel B, Kawabata H, Hodder S. | title=Young HIV-infected adults are at greater risk for medication nonadherence | journal=MedGenMed. | year=2002 | pages=21 | volume=4| issue=3 | pmid=12466764 | |||
| }}</ref> The reasons for non-adherence and non-persistence with HAART are varied and overlapping. Major psychosocial issues, such as poor access to medical care, inadequate social supports, psychiatric disease and drug abuse contribute to non-adherence. The complexity of these HAART regimens, whether due to pill number, dosing frequency, meal restrictions or other issues along with side effects that create intentional non-adherence also contribute to this problem.<ref name=Nieuwkerk>{{ | |||
| cite journal | |||
| | author=Nieuwkerk, P., Sprangers, M., Burger, D., Hoetelmans, R. M., Hugen, P. W., Danner, S. A., van Der Ende, M. E., Schneider, M. M., Schrey, G., Meenhorst, P. L., Sprenger, H. G., Kauffmann, R. H., Jambroes, M., Chesney, M. A., de Wolf, F., Lange, J. M. and the ATHENA Project. | title=Limited Patient Adherence to Highly Active Antiretroviral Therapy for HIV-1 Infection in an Observational Cohort Study | journal=Arch. Intern. Med. | year=2001 | pages=1962-1968 | volume=161 | issue=16 | pmid=11525698 | |||
| }}</ref><ref name=Kleeberger>{{ | |||
| cite journal | |||
| | author=Kleeberger, C., Phair, J., Strathdee, S., Detels, R., Kingsley, L. and Jacobson, L. P. | title=Determinants of Heterogeneous Adherence to HIV-Antiretroviral Therapies in the Multicenter AIDS Cohort Study| journal=J. Acquir. Immune Defic. Syndr. | year=2001 | pages=82-92 | volume=26 | issue=1 | pmid=11176272 | |||
| }}</ref><ref name=heath>{{ | |||
| cite journal | |||
| | author=Heath, K. V., Singer, J., O'Shaughnessy, M. V., Montaner, J. S. and Hogg, R. S. | title=Intentional Nonadherence Due to Adverse Symptoms Associated With Antiretroviral Therapy | journal=J. Acquir. Immune Defic. Syndr. | year=2002 | pages=211-217 | volume=31 | issue=2 | pmid=12394800 | |||
| }}</ref> The side effects include ], ], ], an increase in ] risks and ]s.<ref name=Montessori>{{ | |||
| cite journal | | |||
| author=Montessori, V., Press, N., Harris, M., Akagi, L., Montaner, J. S. | | |||
| title=Adverse effects of antiretroviral therapy for HIV infection. | | |||
| journal=CMAJ | year=2004 | pages=229-238 | volume=170 | issue=2 | pmid=14734438 | |||
| }}</ref><ref name=Saitoh>{{ | |||
| cite journal | |||
| | author=Saitoh, A., Hull, A. D., Franklin, P. and Spector, S. A. | |||
| | title=Myelomeningocele in an infant with intrauterine exposure to efavirenz | |||
| | journal=J. Perinatol. | year=2005 | pages=555-556 | volume=25 | issue=8 | |||
| | pmid=16047034 | |||
| }}</ref> | |||
| The timing for starting HIV treatment is still debated. There is no question that treatment should be started before the patient's CD4 count falls below 200, and most national guidelines say to start treatment once the CD4 count falls below 350; but there is some evidence from cohort studies that treatment should be started before the CD4 count falls below 350.<ref name="Wang2004">{{ | |||
| cite journal | |||
| | author=Wang C, Vlahov D, Galai N, ''et al.'' | |||
| | title=Mortality in HIV-seropositive versus seronegative persons in the era of highly active antiretroviral therapy. | |||
| | journal=J. Infect. Dis. | year=2004 | volume=190 | pages=1046–54 | |||
| | pmid=15319852 | |||
| }}</ref><ref name="Wood">{{ | |||
| cite journal | |||
| | author=Wood E, HoggRS, Harrigan PR, Montaner JS. | |||
| | title=When to initial antiretroviral therapy in HIV-1-infected adults: a review for clinicians and patients | |||
| | journal=Lancet Infect. Dis. | |||
| | year=2005 | |||
| | volume=5 | |||
| | pages=407–14 | |||
| }}</ref> In those countries where CD4 counts are not available, patients with WHO stage III or IV disease<ref name="WHO">{{ | |||
| cite web | |||
| | author=World Health Organisation | |||
| | title=WHO case definitions of HIV for surveillance and revised clinical staging and immunological classification | |||
| | year=2006 | |||
| | url=http://www.who.int/hiv/pub/guidelines/WHO%20HIV%20Staging.pdf | |||
| | accessdate=2006-12-27 | |||
| |format=PDF}}</ref> should be offered treatment. | |||
| Anti-retroviral drugs are expensive, and the majority of the world's infected individuals do not have access to medications and treatments for HIV and AIDS.<ref name=Ferrantelli>{{ | |||
| cite journal | |||
| | author=Ferrantelli F, Cafaro A, Ensoli B. | title=Nonstructural HIV proteins as targets for prophylactic or therapeutic vaccines | journal=Curr Opin Biotechnol. | year=2004 | pages=543-556 | volume=15 | issue=6 | |||
| | pmid=15560981 | |||
| }}</ref> Research to improve current treatments includes decreasing side effects of current drugs, further simplifying drug regimens to improve adherence, and determining the best sequence of regimens to manage drug resistance. Unfortunately, only a vaccine is thought to be able to halt the pandemic. This is because a vaccine would cost less, thus being affordable for developing countries, and would not require daily treatment.<ref name=Ferrantelli/> However, after over 20 years of research, HIV-1 remains a difficult target for a vaccine.<ref name=Ferrantelli/> | |||
| Promising new treatments include ]<ref name="Cre recombinase">Researchers at the Heinrich Pette Institute of Experimental Virology and Immunology at Hamburg:{{cite web | |||
| | author=Paternity Testing Labs | |||
| | title=German scientists “cure” HIV-infected human lymphocytes | |||
| | year=2007 | |||
| | url=http://www.theblogofscience.com/german-scientists-cure-hiv-infected-human-lymphocytes/ | |||
| | accessdate=2008-04-03 | |||
| }}</ref> and the enzyme ],<ref name="Tre recombinase"> scientists at the Max Planck Institute for Molecular Cell Biology and Genetics in Dresden: {{ | |||
| cite web | |||
| | author=Terra Daily | |||
| | title=Another Potential Cure For HIV Discovered | |||
| | year=2007 | |||
| | url=http://www.terradaily.com/reports/Another_Potential_Cure_For_HIV_Discovered_999.html | |||
| | accessdate=2007-06-29 | |||
| }}</ref> both of which are able to remove HIV from an infected cell. These enzymes promise a treatment in which a patient's ] are extracted, cured, and reinjected to promulgate the enzyme into the body. The carried enzyme then finds and removes the virus. | |||
| ==Epidemiology== | |||
| {{main|AIDS pandemic}} | |||
| ] | |||
| UNAIDS and the WHO estimate that AIDS has killed more than 25 million people since it was first recognized in 1981, making it one of the most destructive pandemics in recorded history. Despite recent improved access to antiretroviral treatment and care in many regions of the world, the AIDS pandemic claimed an estimated 2.8 million (between 2.4 and 3.3 million) lives in 2005 of which more than half a million (570,000) were children.<ref name=UNAIDS2006 /> | |||
| In 2007, between 30.6 and 36.1 million people were believed to live with HIV, and it killed an estimated 2.1 million people that year, including 330,000 children; there were 2.5 million new infections.<ref name=UNAIDS2007>{{cite web | |||
| | author =], ] | |||
| | month = December | year = 2007 | |||
| | title = 2007 AIDS epidemic update | |||
| | url= http://data.unaids.org/pub/EPISlides/2007/2007_epiupdate_en.pdf | |||
| | accessdate = 2008-03-12 | |||
| | format= PDF | |||
| }}</ref> | |||
| ] remains by far the worst-affected region, with an estimated 21.6 to 27.4 million people currently living with HIV. Two million [1.5–3.0 million] of them are children younger than 15 years of age. More than 64% of all people living with HIV are in sub-Saharan Africa, as are more than three quarters of all women living with HIV. In 2005, there were 12.0 million [10.6–13.6 million] AIDS orphans living in sub-Saharan Africa 2005.<ref name=UNAIDS2006 /> ] are second-worst affected with 15% of the total. AIDS accounts for the deaths of 500,000 children in this region. ] has the largest number of HIV patients in the world followed by ].<ref>{{cite news |first=Donald |last=McNeil, Jr. |authorlink= |coauthors= |title= U.N. Agency to Say It Overstated Extent of H.I.V. Cases by Millions |url=http://query.nytimes.com/gst/fullpage.html?res=9C01EEDF103BF933A15752C1A9619C8B63&n |work= |publisher=''The New York Times'' |date=November 20, 2007 |accessdate=2008-01-16 }}</ref> India has an estimated 2.5 million infections (0.23% of population), making India the country with the third largest population of HIV patients. In the 35 African nations with the highest prevalence, average ] is 48.3 years—6.5 years less than it would be without the disease.<ref name=UNAIDS2001>{{ | |||
| cite web | |||
| | author=UNAIDS | publisher= | year=2001 | |||
| | url=http://data.unaids.org/Publications/External-Documents/GAS26-rt3_en.pdf | |||
| | title=Special Session of the General Assembly on HIV/AIDS Round table 3 Socio-economic impact of the epidemic and the strengthening of national capacities to combat HIV/AIDS | |||
| | accessdate=2006-06-15 | |||
| | format= ] | |||
| }}</ref> | |||
| The latest evaluation report of the ] Operations Evaluation Department assesses the development effectiveness of the World Bank's country-level HIV/AIDS assistance defined as policy dialogue, analytic work, and lending with the explicit objective of reducing the scope or impact of the AIDS epidemic.<ref name=Worldbank>{{ | |||
| cite web | |||
| | author=] | publisher= | year=2005 | |||
| | url=http://www.worldbank.org/oed/aids/main_report.html | |||
| | title=Evaluating the World Bank's Assistance for Fighting the HIV/AIDS Epidemic | |||
| | accessdate=2006-01-17 | |||
| }}</ref> This is the first comprehensive evaluation of the World Bank's HIV/AIDS support to countries, from the beginning of the epidemic through mid-2004. Because the Bank aims to assist in implementation of national government programmes, their experience provides important insights on how national AIDS programmes can be made more effective. | |||
| The development of ] as effective therapy for HIV infection and AIDS has substantially reduced the death rate from this disease in those areas where these drugs are widely available. This has created the misperception that the disease has vanished. In fact, as the life expectancy of persons with AIDS has increased in countries where HAART is widely used, the number of persons living with AIDS has increased substantially. In the United States, the number of persons with AIDS increased from about 35,000 in 1988 to over 220,000 in 1996 and 312,000 in 2002<ref name=CDC2002>{{ | |||
| cite journal | | |||
| author=] | | |||
| title=Cases of HIV Infection and AIDS in the United States, 2002 | | |||
| journal=HIV/AIDS Surveillance Report |year = 2002| url=http://www.cdc.gov/hiv/topics/surveillance/resources/reports/2002report/table1.htm | |||
| }}</ref> | |||
| In Africa, the number of MTCT and the prevalence of AIDS is beginning to reverse decades of steady progress in child survival. Countries such as Uganda are attempting to curb the MTCT epidemic by offering VCT (voluntary counselling and testing), PMTCT (prevention of mother-to-child transmission) and ANC (ante-natal care) services, which include the distribution of antiretroviral therapy. | |||
| ==AIDS denialism== | |||
| {{main|AIDS denialism}} | |||
| Individuals, including several scientists who are not recognized experts on HIV, question the connection between HIV and AIDS,<ref name=Duesberg>{{cite journal | |||
| | author=Duesberg, P. H. | |||
| | title=HIV is not the cause of AIDS | |||
| | journal=Science | year=1988 | pages=514, 517 | volume=241 | issue=4865 | |||
| | pmid=3399880 | doi=10.1126/science.3399880 | |||
| }}</ref> the ''specific details'' qualifying (but not denying) the existence of HIV itself(This is a critique of the Montagnier group's 1983 claims),<ref name=Papadopulos>{{ | |||
| cite journal | |||
| | author=Papadopulos-Eleopulos, E., Turner, V. F., Papadimitriou, J., Page, B., Causer, D., Alfonso, H., Mhlongo, S., Miller, T., Maniotis, A. and Fiala, C. | |||
| | title=A critique of the Montagnier evidence for the HIV/AIDS hypothesis | |||
| | journal=Med Hypotheses | year=2004 | pages=597–601 | volume=63 | issue=4 | |||
| | pmid=15325002 | |||
| }}</ref> or the validity of current testing and treatment methods. These claims have been examined and rejected as having no validity,<ref name=consensus> For evidence that HIV is the cause of AIDS, see (for example): | |||
| *{{cite journal |author= ,|title=The Durban Declaration |journal=Nature |volume=406 |issue=6791 |pages=15–6 |year=2000 |pmid=10894520 |doi=10.1038/35017662}} - full text . | |||
| *{{cite journal | |||
| | author=Cohen, J. | |||
| | title=The Controversy over HIV and AIDS | |||
| | journal=Science | year=1994 | pages=1642–1649 | volume=266 | issue=5191 | |||
| | url=http://www.sciencemag.org/feature/data/cohen/266-5191-1642a.pdf | |||
| | format = PDF | |||
| | doi=10.1126/science.7992043 | |||
| | pmid=7992043}} | |||
| *{{cite web | |||
| | author=Various | |||
| | publisher=] | year= | |||
| | url=http://www3.niaid.nih.gov/news/focuson/hiv/resources/ | |||
| | title=Focus on the HIV-AIDS Connection: Resource links | |||
| | accessdate = 2006-09-07 | |||
| }} | |||
| *{{cite journal |author=O'Brien SJ, Goedert JJ |title=HIV causes AIDS: Koch's postulates fulfilled |journal=Curr. Opin. Immunol. |volume=8 |issue=5 |pages=613–8 |year=1996 |pmid=8902385 |doi=}} | |||
| *{{cite journal |author=Galéa P, Chermann JC |title=HIV as the cause of AIDS and associated diseases |journal=Genetica |volume=104 |issue=2 |pages=133–42 |year=1998 |pmid=10220906 |doi=}}</ref> although they have had a political impact, particularly in ], where governmental acceptance of AIDS denialism has been blamed for an ineffective response to that country's AIDS epidemic.<ref>{{cite journal |author=Watson J |title=Scientists, activists sue South Africa's AIDS 'denialists' |journal=Nat. Med. |volume=12 |issue=1 |pages=6 |year=2006 |pmid=16397537 |doi=10.1038/nm0106-6a}}</ref><ref>{{cite journal |author=Baleta A |title=S Africa's AIDS activists accuse government of murder |journal=Lancet |volume=361 |issue=9363 |pages=1105 |year=2003 |pmid=12672319 |doi=10.1016/S0140-6736(03)12909-1}}</ref><ref>{{cite journal |author=Cohen J |title=South Africa's new enemy |journal=Science |volume=288 |issue=5474 |pages=2168–70 |year=2000 |pmid=10896606 |doi=10.1126/science.288.5474.2168}}</ref> | |||
| ==References== | |||
| {{reflist|colwidth=30em}} | |||
| ==External links== | |||
| {{Sisterlinks|b=Sexual Health/Sexually Transmitted Diseases#HIV|commons=Category:HIV|n=Category:AIDS}} | |||
| <!--===========================({{NoMoreLinks}})=============================== | |||
| | PLEASE BE CAUTIOUS IN ADDING MORE LINKS TO THIS ARTICLE. WIKIPEDIA IS | | |||
| | NOT A COLLECTION OF LINKS. | | |||
| | | | |||
| | Excessive or inappropriate links WILL BE DELETED. | | |||
| | See ] and ] for details. | | |||
| | | | |||
| | If there are already plentiful links, please propose additions or | | |||
| | replacements on this article's discussion page. Or submit your link | | |||
| | to the appropriate category at the Open Directory Project (www.dmoz.org)| | |||
| | and link back to that category using the {{dmoz}} template. | | |||
| ===========================({{NoMoreLinks}})===============================--> | |||
| * {{Dmoz|Health/Conditions_and_Diseases/Immune_Disorders/Immune_Deficiency/AIDS/|HIV/AIDS}} | |||
| * {{cite web | |||
| |url=http://aidsinfo.nih.gov/ | |||
| |title=AIDSinfo - HIV/AIDS Treatment Information | |||
| |accessdate=2008-03-21 | |||
| |publisher=US Department of Health and Human Services | |||
| |format= | |||
| |work= | |||
| }} | |||
| * {{cite web | |||
| |url=http://www.unaids.org/en/ | |||
| |title=UNAIDS: The Joint United Nations Programme on HIV/AIDS | |||
| |accessdate=2008-03-21 | |||
| |publisher=UNAIDS | |||
| |format= | |||
| |work= | |||
| }} | |||
| * {{cite web | |||
| |url=http://www.AIDS.gov | |||
| |title=AIDS.gov: Portal to all Federal HIV/AIDS information | |||
| |accessdate=2008-05-20 | |||
| |publisher=AIDS.gov | |||
| |format= | |||
| |work= | |||
| }} | |||
| * {{cite web | |||
| |url=http://www.thebody.com/ | |||
| |title=HIV News and Resources | |||
| |accessdate=2008-07-18 | |||
| |publisher=The Body | |||
| |format= | |||
| |work= | |||
| }} | |||
| {{AIDS}} | |||
| {{STD/STI}} | |||
| ] | |||
| ] | |||
| ] | ] | ||
| ] | ] | ||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
Latest revision as of 20:56, 31 December 2024
Human retrovirus, cause of AIDSThis article is about the virus. For the infection caused by the virus, see HIV/AIDS. For other uses, see HIV (disambiguation). "AIDS virus" redirects here. For the computer virus, see AIDS (computer virus).
| Human immunodeficiency viruses | |
|---|---|

| |
| Scanning electron micrograph of HIV-1 (in green) budding from cultured lymphocyte. Multiple round bumps on cell surface represent sites of assembly and budding of virions. | |
| Scientific classification | |
| (unranked): | Virus |
| Realm: | Riboviria |
| Kingdom: | Pararnavirae |
| Phylum: | Artverviricota |
| Class: | Revtraviricetes |
| Order: | Ortervirales |
| Family: | Retroviridae |
| Subfamily: | Orthoretrovirinae |
| Genus: | Lentivirus |
| Groups included | |
| Other lentiviruses | |
The human immunodeficiency viruses (HIV) are two species of Lentivirus (a subgroup of retrovirus) that infect humans. Over time, they cause acquired immunodeficiency syndrome (AIDS), a condition in which progressive failure of the immune system allows life-threatening opportunistic infections and cancers to thrive. Without treatment, the average survival time after infection with HIV is estimated to be 9 to 11 years, depending on the HIV subtype.
In most cases, HIV is a sexually transmitted infection and occurs by contact with or transfer of blood, pre-ejaculate, semen, and vaginal fluids. Non-sexual transmission can occur from an infected mother to her infant during pregnancy, during childbirth by exposure to her blood or vaginal fluid, and through breast milk. Within these bodily fluids, HIV is present as both free virus particles and virus within infected immune cells. Research has shown (for both same-sex and opposite-sex couples) that HIV is not contagious during sexual intercourse without a condom if the HIV-positive partner has a consistently undetectable viral load.
HIV infects vital cells in the human immune system, such as helper T cells (specifically CD4 T cells), macrophages, and dendritic cells. HIV infection leads to low levels of CD4 T cells through a number of mechanisms, including pyroptosis of abortively infected T cells, apoptosis of uninfected bystander cells, direct viral killing of infected cells, and killing of infected CD4 T cells by CD8 cytotoxic lymphocytes that recognize infected cells. When CD4 T cell numbers decline below a critical level, cell-mediated immunity is lost, and the body becomes progressively more susceptible to opportunistic infections, leading to the development of AIDS.
Virology
| Species | Virulence | Infectivity | Prevalence | Inferred origin |
|---|---|---|---|---|
| HIV-1 | High | High | Global | Common chimpanzee |
| HIV-2 | Lower | Low | West Africa | Sooty mangabey |
Classification
See also: Subtypes of HIVHIV is a member of the genus Lentivirus, part of the family Retroviridae. Lentiviruses have many morphologies and biological properties in common. Many species are infected by lentiviruses, which are characteristically responsible for long-duration illnesses with a long incubation period. Lentiviruses are transmitted as single-stranded, positive-sense, enveloped RNA viruses. Upon entry into the target cell, the viral RNA genome is converted (reverse transcribed) into double-stranded DNA by a virally encoded enzyme, reverse transcriptase, that is transported along with the viral genome in the virus particle. The resulting viral DNA is then imported into the cell nucleus and integrated into the cellular DNA by a virally encoded enzyme, integrase, and host co-factors. Once integrated, the virus may become latent, allowing the virus and its host cell to avoid detection by the immune system, for an indeterminate amount of time. The virus can remain dormant in the human body for up to ten years after primary infection; during this period the virus does not cause symptoms. Alternatively, the integrated viral DNA may be transcribed, producing new RNA genomes and viral proteins, using host cell resources, that are packaged and released from the cell as new virus particles that will begin the replication cycle anew.
Two types of HIV have been characterized: HIV-1 and HIV-2. HIV-1 is the virus that was initially discovered and termed both lymphadenopathy associated virus (LAV) and human T-lymphotropic virus 3 (HTLV-III). HIV-1 is more virulent and more infective than HIV-2, and is the cause of the majority of HIV infections globally. The lower infectivity of HIV-2, compared to HIV-1, implies that fewer of those exposed to HIV-2 will be infected per exposure. Due to its relatively poor capacity for transmission, HIV-2 is largely confined to West Africa.
Structure and genome
Main article: Structure and genome of HIV
HIV is similar in structure to other retroviruses. It is roughly spherical with a diameter of about 120 nm, around 100,000 times smaller in volume than a red blood cell. It is composed of two copies of positive-sense single-stranded RNA that codes for the virus' nine genes enclosed by a conical capsid composed of 2,000 copies of the viral protein p24. The single-stranded RNA is tightly bound to nucleocapsid proteins, p7, and enzymes needed for the development of the virion such as reverse transcriptase, proteases, ribonuclease and integrase. A matrix composed of the viral protein p17 surrounds the capsid ensuring the integrity of the virion particle.
This is, in turn, surrounded by the viral envelope, that is composed of the lipid bilayer taken from the membrane of a human host cell when the newly formed virus particle buds from the cell. The viral envelope contains proteins from the host cell and relatively few copies of the HIV envelope protein, which consists of a cap made of three molecules known as glycoprotein (gp) 120, and a stem consisting of three gp41 molecules that anchor the structure into the viral envelope. The envelope protein, encoded by the HIV env gene, allows the virus to attach to target cells and fuse the viral envelope with the target cell's membrane releasing the viral contents into the cell and initiating the infectious cycle.

As the sole viral protein on the surface of the virus, the envelope protein is a major target for HIV vaccine efforts. Over half of the mass of the trimeric envelope spike is N-linked glycans. The density is high as the glycans shield the underlying viral protein from neutralisation by antibodies. This is one of the most densely glycosylated molecules known and the density is sufficiently high to prevent the normal maturation process of glycans during biogenesis in the endoplasmic and Golgi apparatus. The majority of the glycans are therefore stalled as immature 'high-mannose' glycans not normally present on human glycoproteins that are secreted or present on a cell surface. The unusual processing and high density means that almost all broadly neutralising antibodies that have so far been identified (from a subset of patients that have been infected for many months to years) bind to, or are adapted to cope with, these envelope glycans.
The molecular structure of the viral spike has now been determined by X-ray crystallography and cryogenic electron microscopy. These advances in structural biology were made possible due to the development of stable recombinant forms of the viral spike by the introduction of an intersubunit disulphide bond and an isoleucine to proline mutation (radical replacement of an amino acid) in gp41. The so-called SOSIP trimers not only reproduce the antigenic properties of the native viral spike, but also display the same degree of immature glycans as presented on the native virus. Recombinant trimeric viral spikes are promising vaccine candidates as they display less non-neutralising epitopes than recombinant monomeric gp120, which act to suppress the immune response to target epitopes.

The RNA genome consists of at least seven structural landmarks (LTR, TAR, RRE, PE, SLIP, CRS, and INS), and nine genes (gag, pol, and env, tat, rev, nef, vif, vpr, vpu, and sometimes a tenth tev, which is a fusion of tat, env and rev), encoding 19 proteins. Three of these genes, gag, pol, and env, contain information needed to make the structural proteins for new virus particles. For example, env codes for a protein called gp160 that is cut in two by a cellular protease to form gp120 and gp41. The six remaining genes, tat, rev, nef, vif, vpr, and vpu (or vpx in the case of HIV-2), are regulatory genes for proteins that control the ability of HIV to infect cells, produce new copies of virus (replicate), or cause disease.
The two tat proteins (p16 and p14) are transcriptional transactivators for the LTR promoter acting by binding the TAR RNA element. The TAR may also be processed into microRNAs that regulate the apoptosis genes ERCC1 and IER3. The rev protein (p19) is involved in shuttling RNAs from the nucleus and the cytoplasm by binding to the RRE RNA element. The vif protein (p23) prevents the action of APOBEC3G (a cellular protein that deaminates cytidine to uridine in the single-stranded viral DNA and/or interferes with reverse transcription). The vpr protein (p14) arrests cell division at G2/M. The nef protein (p27) down-regulates CD4 (the major viral receptor), as well as the MHC class I and class II molecules.
Nef also interacts with SH3 domains. The vpu protein (p16) influences the release of new virus particles from infected cells. The ends of each strand of HIV RNA contain an RNA sequence called a long terminal repeat (LTR). Regions in the LTR act as switches to control production of new viruses and can be triggered by proteins from either HIV or the host cell. The Psi element is involved in viral genome packaging and recognized by gag and rev proteins. The SLIP element (TTTTTT) is involved in the frameshift in the gag-pol reading frame required to make functional pol.
Tropism
Main article: HIV tropism
The term viral tropism refers to the cell types a virus infects. HIV can infect a variety of immune cells such as CD4 T cells, macrophages, and microglial cells. HIV-1 entry to macrophages and CD4 T cells is mediated through interaction of the virion envelope glycoproteins (gp120) with the CD4 molecule on the target cells' membrane and also with chemokine co-receptors.
Macrophage-tropic (M-tropic) strains of HIV-1, or non-syncytia-inducing strains (NSI; now called R5 viruses) use the β-chemokine receptor, CCR5, for entry and are thus able to replicate in both macrophages and CD4 T cells. This CCR5 co-receptor is used by almost all primary HIV-1 isolates regardless of viral genetic subtype. Indeed, macrophages play a key role in several critical aspects of HIV infection. They appear to be the first cells infected by HIV and perhaps the source of HIV production when CD4 cells become depleted in the patient. Macrophages and microglial cells are the cells infected by HIV in the central nervous system. In the tonsils and adenoids of HIV-infected patients, macrophages fuse into multinucleated giant cells that produce huge amounts of virus.
T-tropic strains of HIV-1, or syncytia-inducing strains (SI; now called X4 viruses) replicate in primary CD4 T cells as well as in macrophages and use the α-chemokine receptor, CXCR4, for entry.
Dual-tropic HIV-1 strains are thought to be transitional strains of HIV-1 and thus are able to use both CCR5 and CXCR4 as co-receptors for viral entry.
The α-chemokine SDF-1, a ligand for CXCR4, suppresses replication of T-tropic HIV-1 isolates. It does this by down-regulating the expression of CXCR4 on the surface of HIV target cells. M-tropic HIV-1 isolates that use only the CCR5 receptor are termed R5; those that use only CXCR4 are termed X4, and those that use both, X4R5. However, the use of co-receptors alone does not explain viral tropism, as not all R5 viruses are able to use CCR5 on macrophages for a productive infection and HIV can also infect a subtype of myeloid dendritic cells, which probably constitute a reservoir that maintains infection when CD4 T cell numbers have declined to extremely low levels.
Some people are resistant to certain strains of HIV. For example, people with the CCR5-Δ32 mutation are resistant to infection by the R5 virus, as the mutation leaves HIV unable to bind to this co-receptor, reducing its ability to infect target cells.
Sexual intercourse is the major mode of HIV transmission. Both X4 and R5 HIV are present in the seminal fluid, which enables the virus to be transmitted from a male to his sexual partner. The virions can then infect numerous cellular targets and disseminate into the whole organism. However, a selection process leads to a predominant transmission of the R5 virus through this pathway. In patients infected with subtype B HIV-1, there is often a co-receptor switch in late-stage disease and T-tropic variants that can infect a variety of T cells through CXCR4. These variants then replicate more aggressively with heightened virulence that causes rapid T cell depletion, immune system collapse, and opportunistic infections that mark the advent of AIDS. HIV-positive patients acquire an enormously broad spectrum of opportunistic infections, which was particularly problematic prior to the onset of HAART therapies; however, the same infections are reported among HIV-infected patients examined post-mortem following the onset of antiretroviral therapies. Thus, during the course of infection, viral adaptation to the use of CXCR4 instead of CCR5 may be a key step in the progression to AIDS. A number of studies with subtype B-infected individuals have determined that between 40 and 50 percent of AIDS patients can harbour viruses of the SI and, it is presumed, the X4 phenotypes.
HIV-2 is much less pathogenic than HIV-1 and is restricted in its worldwide distribution to West Africa. The adoption of "accessory genes" by HIV-2 and its more promiscuous pattern of co-receptor usage (including CD4-independence) may assist the virus in its adaptation to avoid innate restriction factors present in host cells. Adaptation to use normal cellular machinery to enable transmission and productive infection has also aided the establishment of HIV-2 replication in humans. A survival strategy for any infectious agent is not to kill its host, but ultimately become a commensal organism. Having achieved a low pathogenicity, over time, variants that are more successful at transmission will be selected.
Replication cycle
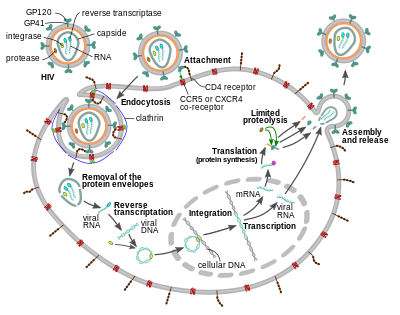
Entry to the cell

The HIV virion enters macrophages and CD4 T cells by the adsorption of glycoproteins on its surface to receptors on the target cell followed by fusion of the viral envelope with the target cell membrane and the release of the HIV capsid into the cell.
Entry to the cell begins through interaction of the trimeric envelope complex (gp160 spike) on the HIV viral envelope and both CD4 and a chemokine co-receptor (generally either CCR5 or CXCR4, but others are known to interact) on the target cell surface. Gp120 binds to integrin α4β7 activating LFA-1, the central integrin involved in the establishment of virological synapses, which facilitate efficient cell-to-cell spreading of HIV-1. The gp160 spike contains binding domains for both CD4 and chemokine receptors.
The first step in fusion involves the high-affinity attachment of the CD4 binding domains of gp120 to CD4. Once gp120 is bound with the CD4 protein, the envelope complex undergoes a structural change, exposing the chemokine receptor binding domains of gp120 and allowing them to interact with the target chemokine receptor. This allows for a more stable two-pronged attachment, which allows the N-terminal fusion peptide gp41 to penetrate the cell membrane. Repeat sequences in gp41, HR1, and HR2 then interact, causing the collapse of the extracellular portion of gp41 into a hairpin shape. This loop structure brings the virus and cell membranes close together, allowing fusion of the membranes and subsequent entry of the viral capsid.
After HIV has bound to the target cell, the HIV RNA and various enzymes, including reverse transcriptase, integrase, ribonuclease, and protease, are injected into the cell. During the microtubule-based transport to the nucleus, the viral single-strand RNA genome is transcribed into double-strand DNA, which is then integrated into a host chromosome.
HIV can infect dendritic cells (DCs) by this CD4-CCR5 route, but another route using mannose-specific C-type lectin receptors such as DC-SIGN can also be used. DCs are one of the first cells encountered by the virus during sexual transmission. They are currently thought to play an important role by transmitting HIV to T cells when the virus is captured in the mucosa by DCs. The presence of FEZ-1, which occurs naturally in neurons, is believed to prevent the infection of cells by HIV.

HIV-1 entry, as well as entry of many other retroviruses, has long been believed to occur exclusively at the plasma membrane. More recently, however, productive infection by pH-independent, clathrin-mediated endocytosis of HIV-1 has also been reported and was recently suggested to constitute the only route of productive entry.
Replication and transcription

Shortly after the viral capsid enters the cell, an enzyme called reverse transcriptase liberates the positive-sense single-stranded RNA genome from the attached viral proteins and copies it into a complementary DNA (cDNA) molecule. The process of reverse transcription is extremely error-prone, and the resulting mutations may cause drug resistance or allow the virus to evade the body's immune system. The reverse transcriptase also has ribonuclease activity that degrades the viral RNA during the synthesis of cDNA, as well as DNA-dependent DNA polymerase activity that creates a sense DNA from the antisense cDNA. Together, the cDNA and its complement form a double-stranded viral DNA that is then transported into the cell nucleus. The integration of the viral DNA into the host cell's genome is carried out by another viral enzyme called integrase.
The integrated viral DNA may then lie dormant, in the latent stage of HIV infection. To actively produce the virus, certain cellular transcription factors need to be present, the most important of which is NF-κB (nuclear factor kappa B), which is upregulated when T cells become activated. This means that those cells most likely to be targeted, entered and subsequently killed by HIV are those actively fighting infection.
During viral replication, the integrated DNA provirus is transcribed into RNA. The full-length genomic RNAs (gRNA) can be packaged into new viral particles in a pseudodiploid form. The selectivity in the packaging is explained by the structural properties of the dimeric conformer of the gRNA. The gRNA dimer is characterized by a tandem three-way junction within the gRNA monomer, in which the SD and AUG hairpins, responsible for splicing and translation respectively, are sequestered and the DIS (dimerization initiation signal) hairpin is exposed. The formation of the gRNA dimer is mediated by a 'kissing' interaction between the DIS hairpin loops of the gRNA monomers. At the same time, certain guanosine residues in the gRNA are made available for binding of the nucleocapsid (NC) protein leading to the subsequent virion assembly. The labile gRNA dimer has been also reported to achieve a more stable conformation following the NC binding, in which both the DIS and the U5:AUG regions of the gRNA participate in extensive base pairing.
RNA can also be processed to produce mature messenger RNAs (mRNAs). In most cases, this processing involves RNA splicing to produce mRNAs that are shorter than the full-length genome. Which part of the RNA is removed during RNA splicing determines which of the HIV protein-coding sequences is translated.
Mature HIV mRNAs are exported from the nucleus into the cytoplasm, where they are translated to produce HIV proteins, including Rev. As the newly produced Rev protein is produced it moves to the nucleus, where it binds to full-length, unspliced copies of virus RNAs and allows them to leave the nucleus. Some of these full-length RNAs function as mRNAs that are translated to produce the structural proteins Gag and Env. Gag proteins bind to copies of the virus RNA genome to package them into new virus particles. HIV-1 and HIV-2 appear to package their RNA differently. HIV-1 will bind to any appropriate RNA. HIV-2 will preferentially bind to the mRNA that was used to create the Gag protein itself.
Recombination
Further information: Genetic recombinationTwo RNA genomes are encapsidated in each HIV-1 particle (see Structure and genome of HIV). Upon infection and replication catalyzed by reverse transcriptase, recombination between the two genomes can occur. Recombination occurs as the single-strand, positive-sense RNA genomes are reverse transcribed to form DNA. During reverse transcription, the nascent DNA can switch multiple times between the two copies of the viral RNA. This form of recombination is known as copy-choice. Recombination events may occur throughout the genome. Anywhere from two to 20 recombination events per genome may occur at each replication cycle, and these events can rapidly shuffle the genetic information that is transmitted from parental to progeny genomes.
Viral recombination produces genetic variation that likely contributes to the evolution of resistance to anti-retroviral therapy. Recombination may also contribute, in principle, to overcoming the immune defenses of the host. Yet, for the adaptive advantages of genetic variation to be realized, the two viral genomes packaged in individual infecting virus particles need to have arisen from separate progenitor parental viruses of differing genetic constitution. It is unknown how often such mixed packaging occurs under natural conditions.
Bonhoeffer et al. suggested that template switching by reverse transcriptase acts as a repair process to deal with breaks in the single-stranded RNA genome. In addition, Hu and Temin suggested that recombination is an adaptation for repair of damage in the RNA genomes. Strand switching (copy-choice recombination) by reverse transcriptase could generate an undamaged copy of genomic DNA from two damaged single-stranded RNA genome copies. This view of the adaptive benefit of recombination in HIV could explain why each HIV particle contains two complete genomes, rather than one. Furthermore, the view that recombination is a repair process implies that the benefit of repair can occur at each replication cycle, and that this benefit can be realized whether or not the two genomes differ genetically. On the view that recombination in HIV is a repair process, the generation of recombinational variation would be a consequence, but not the cause of, the evolution of template switching.
HIV-1 infection causes chronic inflammation and production of reactive oxygen species. Thus, the HIV genome may be vulnerable to oxidative damage, including breaks in the single-stranded RNA. For HIV, as well as for viruses in general, successful infection depends on overcoming host defense strategies that often include production of genome-damaging reactive oxygen species. Thus, Michod et al. suggested that recombination by viruses is an adaptation for repair of genome damage, and that recombinational variation is a byproduct that may provide a separate benefit.
Assembly and release
The final step of the viral cycle, assembly of new HIV-1 virions, begins at the plasma membrane of the host cell. The Env polyprotein (gp160) goes through the endoplasmic reticulum and is transported to the Golgi apparatus where it is cleaved by furin resulting in the two HIV envelope glycoproteins, gp41 and gp120. These are transported to the plasma membrane of the host cell where gp41 anchors gp120 to the membrane of the infected cell. The Gag (p55) and Gag-Pol (p160) polyproteins also associate with the inner surface of the plasma membrane along with the HIV genomic RNA as the forming virion begins to bud from the host cell. The budded virion is still immature as the gag polyproteins still need to be cleaved into the actual matrix, capsid and nucleocapsid proteins. This cleavage is mediated by the packaged viral protease and can be inhibited by antiretroviral drugs of the protease inhibitor class. The various structural components then assemble to produce a mature HIV virion. Only mature virions are then able to infect another cell.
Spread within the body

The classical process of infection of a cell by a virion can be called "cell-free spread" to distinguish it from a more recently recognized process called "cell-to-cell spread". In cell-free spread (see figure), virus particles bud from an infected T cell, enter the blood or extracellular fluid and then infect another T cell following a chance encounter. HIV can also disseminate by direct transmission from one cell to another by a process of cell-to-cell spread, for which two pathways have been described. Firstly, an infected T cell can transmit virus directly to a target T cell via a virological synapse. Secondly, an antigen-presenting cell (APC), such as a macrophage or dendritic cell, can transmit HIV to T cells by a process that either involves productive infection (in the case of macrophages) or capture and transfer of virions in trans (in the case of dendritic cells). Whichever pathway is used, infection by cell-to-cell transfer is reported to be much more efficient than cell-free virus spread. A number of factors contribute to this increased efficiency, including polarised virus budding towards the site of cell-to-cell contact, close apposition of cells, which minimizes fluid-phase diffusion of virions, and clustering of HIV entry receptors on the target cell towards the contact zone. Cell-to-cell spread is thought to be particularly important in lymphoid tissues, where CD4 T cells are densely packed and likely to interact frequently. Intravital imaging studies have supported the concept of the HIV virological synapse in vivo. The many dissemination mechanisms available to HIV contribute to the virus' ongoing replication in spite of anti-retroviral therapies.
Genetic variability
Further information: Subtypes of HIV
HIV differs from many viruses in that it has very high genetic variability. This diversity is a result of its fast replication cycle, with the generation of about 10 virions every day, coupled with a high mutation rate of approximately 3 x 10 per nucleotide base per cycle of replication and recombinogenic properties of reverse transcriptase.
This complex scenario leads to the generation of many variants of HIV in a single infected patient in the course of one day. This variability is compounded when a single cell is simultaneously infected by two or more different strains of HIV. When simultaneous infection occurs, the genome of progeny virions may be composed of RNA strands from two different strains. This hybrid virion then infects a new cell where it undergoes replication. As this happens, the reverse transcriptase, by jumping back and forth between the two different RNA templates, will generate a newly synthesized retroviral DNA sequence that is a recombinant between the two parental genomes. This recombination is most obvious when it occurs between subtypes.
The closely related simian immunodeficiency virus (SIV) has evolved into many strains, classified by the natural host species. SIV strains of the African green monkey (SIVagm) and sooty mangabey (SIVsmm) are thought to have a long evolutionary history with their hosts. These hosts have adapted to the presence of the virus, which is present at high levels in the host's blood, but evokes only a mild immune response, does not cause the development of simian AIDS, and does not undergo the extensive mutation and recombination typical of HIV infection in humans.
In contrast, when these strains infect species that have not adapted to SIV ("heterologous" or similar hosts such as rhesus or cynomologus macaques), the animals develop AIDS and the virus generates genetic diversity similar to what is seen in human HIV infection. Chimpanzee SIV (SIVcpz), the closest genetic relative of HIV-1, is associated with increased mortality and AIDS-like symptoms in its natural host. SIVcpz appears to have been transmitted relatively recently to chimpanzee and human populations, so their hosts have not yet adapted to the virus. This virus has also lost a function of the nef gene that is present in most SIVs. For non-pathogenic SIV variants, nef suppresses T cell activation through the CD3 marker. Nef's function in non-pathogenic forms of SIV is to downregulate expression of inflammatory cytokines, MHC-1, and signals that affect T cell trafficking. In HIV-1 and SIVcpz, nef does not inhibit T-cell activation and it has lost this function. Without this function, T cell depletion is more likely, leading to immunodeficiency.
Three groups of HIV-1 have been identified on the basis of differences in the envelope (env) region: M, N, and O. Group M is the most prevalent and is subdivided into eight subtypes (or clades), based on the whole genome, which are geographically distinct. The most prevalent are subtypes B (found mainly in North America and Europe), A and D (found mainly in Africa), and C (found mainly in Africa and Asia); these subtypes form branches in the phylogenetic tree representing the lineage of the M group of HIV-1. Co-infection with distinct subtypes gives rise to circulating recombinant forms (CRFs). In 2000, the last year in which an analysis of global subtype prevalence was made, 47.2% of infections worldwide were of subtype C, 26.7% were of subtype A/CRF02_AG, 12.3% were of subtype B, 5.3% were of subtype D, 3.2% were of CRF_AE, and the remaining 5.3% were composed of other subtypes and CRFs. Most HIV-1 research is focused on subtype B; few laboratories focus on the other subtypes. The existence of a fourth group, "P", has been hypothesised based on a virus isolated in 2009. The strain is apparently derived from gorilla SIV (SIVgor), first isolated from western lowland gorillas in 2006.
HIV-2's closest relative is SIVsm, a strain of SIV found in sooty mangabees. Since HIV-1 is derived from SIVcpz, and HIV-2 from SIVsm, the genetic sequence of HIV-2 is only partially homologous to HIV-1 and more closely resembles that of SIVsm.
Diagnosis
Main article: Diagnosis of HIV/AIDS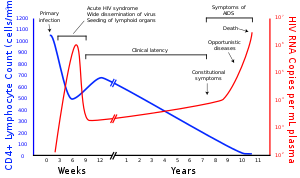
Many HIV-positive people are unaware that they are infected with the virus. For example, in 2001 less than 1% of the sexually active urban population in Africa had been tested, and this proportion is even lower in rural populations. Furthermore, in 2001 only 0.5% of pregnant women attending urban health facilities were counselled, tested or received their test results. Again, this proportion is even lower in rural health facilities. Since donors may therefore be unaware of their infection, donor blood and blood products used in medicine and medical research are routinely screened for HIV.
HIV-1 testing is initially done using an enzyme-linked immunosorbent assay (ELISA) to detect antibodies to HIV-1. Specimens with a non-reactive result from the initial ELISA are considered HIV-negative, unless new exposure to an infected partner or partner of unknown HIV status has occurred. Specimens with a reactive ELISA result are retested in duplicate. If the result of either duplicate test is reactive, the specimen is reported as repeatedly reactive and undergoes confirmatory testing with a more specific supplemental test (e.g., a polymerase chain reaction (PCR), western blot or, less commonly, an immunofluorescence assay (IFA)). Only specimens that are repeatedly reactive by ELISA and positive by IFA or PCR or reactive by western blot are considered HIV-positive and indicative of HIV infection. Specimens that are repeatedly ELISA-reactive occasionally provide an indeterminate western blot result, which may be either an incomplete antibody response to HIV in an infected person or nonspecific reactions in an uninfected person.
HIV deaths in 2014 excluding the U.S.:
Nigeria (15.76%) South Africa (12.51%) India (11.50%) Tanzania (4.169%) Mozambique (4.061%) Zimbabwe (3.49%) Cameroon (3.09%) Indonesia (3.04%) Kenya (2.98%) Uganda (2.97%) Malawi (2.94%) DR Congo (2.17%) Ethiopia (2.11%) Other (29.21%)Although IFA can be used to confirm infection in these ambiguous cases, this assay is not widely used. In general, a second specimen should be collected more than a month later and retested for persons with indeterminate western blot results. Although much less commonly available, nucleic acid testing (e.g., viral RNA or proviral DNA amplification method) can also help diagnosis in certain situations. In addition, a few tested specimens might provide inconclusive results because of a low quantity specimen. In these situations, a second specimen is collected and tested for HIV infection.
Modern HIV testing is extremely accurate, when the window period is taken into consideration. A single screening test is correct more than 99% of the time. The chance of a false-positive result in a standard two-step testing protocol is estimated to be about 1 in 250,000 in a low risk population. Testing post-exposure is recommended immediately and then at six weeks, three months, and six months.
The latest recommendations of the US Centers for Disease Control and Prevention (CDC) show that HIV testing must start with an immunoassay combination test for HIV-1 and HIV-2 antibodies and p24 antigen. A negative result rules out HIV exposure, while a positive one must be followed by an HIV-1/2 antibody differentiation immunoassay to detect which antibodies are present. This gives rise to four possible scenarios:
- 1. HIV-1 (+) & HIV-2 (−): HIV-1 antibodies detected
- 2. HIV-1 (−) & HIV-2 (+): HIV-2 antibodies detected
- 3. HIV-1 (+) & HIV-2 (+): both HIV-1 and HIV-2 antibodies detected
- 4. HIV-1 (−) or indeterminate & HIV-2 (−): Nucleic acid test must be carried out to detect the acute infection of HIV-1 or its absence.
Research
Main article: HIV/AIDS researchHIV/AIDS research includes all medical research that attempts to prevent, treat, or cure HIV/AIDS, as well as fundamental research about the nature of HIV as an infectious agent and AIDS as the disease caused by HIV.
Many governments and research institutions participate in HIV/AIDS research. This research includes behavioral health interventions, such as research into sex education, and drug development, such as research into microbicides for sexually transmitted diseases, HIV vaccines, and anti-retroviral drugs. Other medical research areas include the topics of pre-exposure prophylaxis, post-exposure prophylaxis, circumcision, and accelerated aging effects.
Treatment and transmission
Main article: Management of HIV/AIDSSee also: HIV/AIDS § Transmission, and Undetectable = UntransmittableThe management of HIV/AIDS typically involves the use of multiple antiretroviral drugs. In many parts of the world, HIV has become a chronic condition, with progression to AIDS increasingly rare.
HIV latency and the resulting viral reservoir in CD4 T cells, dendritic cells, and macrophages is the main barrier to eradication of the virus.
While HIV is highly virulent, transmission through sexual contact does not occur when an HIV-positive individual maintains a consistently undetectable viral load (<50 copies/ml) due to antiretroviral treatment. This concept was first proposed by the Swiss Federal Commission for AIDS/HIV in 2008 in what is known as the Swiss Statement. Although initially controversial, subsequent studies have confirmed that the risk of transmitting HIV through sex is effectively zero when the HIV-positive person has a consistently undetectable viral load, a concept now widely known as U=U, or "Undetectable = Untransmittable."
Studies that established the U=U principle include Opposites Attract, PARTNER 1, PARTNER 2 (which focused on male-male couples), and HPTN052 (which focused on heterosexual couples). These studies involved couples where one partner was HIV-positive and one was HIV-negative, and included regular HIV testing. Across these four studies, a total of 4,097 couples participated from four continents, reporting 151,880 acts of condomless sex with zero phylogenetically-linked HIV transmissions when the positive partner had an undetectable viral load. Following these findings, the U=U consensus statement advocating the use of the term 'zero risk' was endorsed by numerous individuals and organizations, including the CDC, the British HIV Association, and The Lancet medical journal.
Additionally, reactivation of herpes simplex virus-2 (HSV-2) in individuals with genital herpes is associated with an increase in CCR-5 enriched CD4 T cells and inflammatory dendritic cells in the dermis of ulcerated genital skin, persisting even after ulcer healing. HIV's tropism for CCR-5 positive cells contributes to the two- to threefold increased risk of HIV acquisition in persons with genital herpes. Notably, daily antiviral medication, such as acyclovir, does not reduce the subclinical post-reactivation inflammation and therefore does not decrease the risk of HIV acquisition.
History
Main article: History of HIV/AIDS Further information: Category:HIV/AIDS by countryDiscovery


 Françoise Barré-Sinoussi, Robert Gallo, and Luc Montagnier, co-discoverers of HIV
Françoise Barré-Sinoussi, Robert Gallo, and Luc Montagnier, co-discoverers of HIV
The first news story on "an exotic new disease" appeared May 18, 1981, in the gay newspaper New York Native.
AIDS was first clinically observed in 1981 in the United States. The initial cases were a cluster of injection drug users and gay men with no known cause of impaired immunity who showed symptoms of Pneumocystis pneumonia (PCP or PJP, the latter term recognizing that the causative agent is now called Pneumocystis jirovecii), a rare opportunistic infection that was known to occur in people with very compromised immune systems. Soon thereafter, researchers at the NYU School of Medicine studied gay men developing a previously rare skin cancer called Kaposi's sarcoma (KS). Many more cases of PJP and KS emerged, alerting U.S. Centers for Disease Control and Prevention (CDC) and a CDC task force was formed to monitor the outbreak. The earliest retrospectively described case of AIDS is believed to have been in Norway beginning in 1966.
In the beginning, the CDC did not have an official name for the disease, often referring to it by way of the diseases that were associated with it, for example, lymphadenopathy, the disease after which the discoverers of HIV originally named the virus. They also used Kaposi's Sarcoma and Opportunistic Infections, the name by which a task force had been set up in 1981. In the general press, the term GRID, which stood for gay-related immune deficiency, had been coined. The CDC, in search of a name and looking at the infected communities, coined "the 4H disease", as it seemed to single out homosexuals, heroin users, hemophiliacs, and Haitians. However, after determining that AIDS was not isolated to the gay community, it was realized that the term GRID was misleading and AIDS was introduced at a meeting in July 1982. By September 1982 the CDC started using the name AIDS.
In 1983, two separate research groups led by American Robert Gallo and French investigators Françoise Barré-Sinoussi and Luc Montagnier independently declared that a novel retrovirus may have been infecting AIDS patients, and published their findings in the same issue of the journal Science. Gallo claimed that a virus his group had isolated from a person with AIDS was strikingly similar in shape to other human T-lymphotropic viruses (HTLVs) his group had been the first to isolate. Gallo admitted in 1987 that the virus he claimed to have discovered in 1984 was in reality a virus sent to him from France the year before. Gallo's group called their newly isolated virus HTLV-III. Montagnier's group isolated a virus from a patient presenting with swelling of the lymph nodes of the neck and physical weakness, two classic symptoms of primary HIV infection. Contradicting the report from Gallo's group, Montagnier and his colleagues showed that core proteins of this virus were immunologically different from those of HTLV-I. Montagnier's group named their isolated virus lymphadenopathy-associated virus (LAV). As these two viruses turned out to be the same, in 1986 LAV and HTLV-III were renamed HIV.
Another group working contemporaneously with the Montagnier and Gallo groups was that of Jay A. Levy at the University of California, San Francisco. He independently discovered the AIDS virus in 1983 and named it the AIDS associated retrovirus (ARV). This virus was very different from the virus reported by the Montagnier and Gallo groups. The ARV strains indicated, for the first time, the heterogeneity of HIV isolates and several of these remain classic examples of the AIDS virus found in the United States.
Origins
Both HIV-1 and HIV-2 are believed to have originated in non-human primates in West-central Africa, and are believed to have transferred to humans (a process known as zoonosis) in the early 20th century.
HIV-1 appears to have originated in southern Cameroon through the evolution of SIVcpz, a simian immunodeficiency virus (SIV) that infects wild chimpanzees (HIV-1 descends from the SIVcpz endemic in the chimpanzee subspecies Pan troglodytes troglodytes). The closest relative of HIV-2 is SIVsmm, a virus of the sooty mangabey (Cercocebus atys atys), an Old World monkey living in littoral West Africa (from southern Senegal to western Côte d'Ivoire). New World monkeys such as the owl monkey are resistant to HIV-1 infection, possibly because of a genomic fusion of two viral resistance genes.
HIV-1 is thought to have jumped the species barrier on at least three separate occasions, giving rise to the three groups of the virus, M, N, and O.

There is evidence that humans who participate in bushmeat activities, either as hunters or as bushmeat vendors, commonly acquire SIV. However, SIV is a weak virus, and it is typically suppressed by the human immune system within weeks of infection. It is thought that several transmissions of the virus from individual to individual in quick succession are necessary to allow it enough time to mutate into HIV. Furthermore, due to its relatively low person-to-person transmission rate, it can only spread throughout the population in the presence of one or more high-risk transmission channels, which are thought to have been absent in Africa prior to the 20th century.
Specific proposed high-risk transmission channels, allowing the virus to adapt to humans and spread throughout the society, depend on the proposed timing of the animal-to-human crossing. Genetic studies of the virus suggest that the most recent common ancestor of the HIV-1 M group dates back to c. 1910. Proponents of this dating link the HIV epidemic with the emergence of colonialism and growth of large colonial African cities, leading to social changes, including different patterns of sexual contact (especially multiple, concurrent partnerships), the spread of prostitution, and the concomitant high frequency of genital ulcer diseases (such as syphilis) in nascent colonial cities. While transmission rates of HIV during vaginal intercourse are typically low, they are increased manyfold if one of the partners has a sexually transmitted infection resulting in genital ulcers. Early 1900s colonial cities were notable for their high prevalence of prostitution and genital ulcers to the degree that as of 1928 as many as 45% of female residents of eastern Leopoldville (currently Kinshasa) were thought to have been prostitutes and as of 1933 around 15% of all residents of the same city were infected by one of the forms of syphilis.
The earliest, well-documented case of HIV in a human dates back to 1959 in the Belgian Congo. The virus may have been present in the United States as early as the mid- to late 1960s, as a sixteen-year-old male named Robert Rayford presented with symptoms in 1966 and died in 1969.
An alternative and likely complementary hypothesis points to the widespread use of unsafe medical practices in Africa during years following World War II, such as unsterile reuse of single-use syringes during mass vaccination, antibiotic, and anti-malaria treatment campaigns. Research on the timing of most recent common ancestor for HIV-1 groups M and O, as well as on HIV-2 groups A and B, indicates that SIV has given rise to transmissible HIV lineages throughout the twentieth century. The dispersed timing of these transmissions to humans implies that no single external factor is needed to explain the cross-species transmission of HIV. This observation is consistent with both of the two prevailing views of the origin of the HIV epidemics, namely SIV transmission to humans during the slaughter or butchering of infected primates, and the colonial expansion of sub-Saharan African cities.
See also
- Antiviral drug
- Discovery and development of HIV-protease inhibitors
- HIV/AIDS denialism
- HIVToolbox
- World AIDS Day
References
- Weiss RA (May 1993). "How does HIV cause AIDS?". Science. 260 (5112): 1273–9. Bibcode:1993Sci...260.1273W. doi:10.1126/science.8493571. PMID 8493571.
- Douek DC, Roederer M, Koup RA (2009). "Emerging Concepts in the Immunopathogenesis of AIDS". Annual Review of Medicine. 60: 471–84. doi:10.1146/annurev.med.60.041807.123549. PMC 2716400. PMID 18947296.
- ^ Powell MK, Benková K, Selinger P, Dogoši M, Kinkorová Luňáčková I, Koutníková H, Laštíková J, Roubíčková A, Špůrková Z, Laclová L, Eis V, Šach J, Heneberg P (2016). "Opportunistic Infections in HIV-Infected Patients Differ Strongly in Frequencies and Spectra between Patients with Low CD4+ Cell Counts Examined Postmortem and Compensated Patients Examined Antemortem Irrespective of the HAART Era". PLOS ONE. 11 (9): e0162704. Bibcode:2016PLoSO..1162704P. doi:10.1371/journal.pone.0162704. PMC 5017746. PMID 27611681.
- UNAIDS, WHO (December 2007). "2007 AIDS epidemic update" (PDF). p. 16.
- ^ Rodger AJ, Cambiano V, Bruun T, Vernazza P, Collins S, Degen O, et al. (June 2019). "Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): final results of a multicentre, prospective, observational study". Lancet. 393 (10189): 2428–2438. doi:10.1016/S0140-6736(19)30418-0. PMC 6584382. PMID 31056293.
- ^ Eisinger RW, Dieffenbach CW, Fauci AS (February 2019). "HIV Viral Load and Transmissibility of HIV Infection: Undetectable Equals Untransmittable". JAMA. 321 (5): 451–452. doi:10.1001/jama.2018.21167. PMID 30629090. S2CID 58599661.
- Mabuka J, Nduati R, Odem-Davis K, Peterson D, Overbaugh J (2012). Desrosiers RC (ed.). "HIV-Specific Antibodies Capable of ADCC Are Common in Breastmilk and Are Associated with Reduced Risk of Transmission in Women with High Viral Loads". PLOS Pathogens. 8 (6): e1002739. doi:10.1371/journal.ppat.1002739. PMC 3375288. PMID 22719248.
- Hahn RA, Inhorn MC, eds. (2009). Anthropology and public health : bridging differences in culture and society (2nd ed.). Oxford: Oxford University Press. p. 449. ISBN 978-0-19-537464-3. OCLC 192042314.
- Mead MN (2008). "Contaminants in human milk: weighing the risks against the benefits of breastfeeding". Environmental Health Perspectives. 116 (10): A426–34. doi:10.1289/ehp.116-a426. PMC 2569122. PMID 18941560. Archived from the original on 6 November 2008.
-
 This article incorporates text from this source, which is in the public domain: "Preventing Mother-to-Child Transmission of HIV". HIV.gov. May 15, 2017. Retrieved December 8, 2017.
This article incorporates text from this source, which is in the public domain: "Preventing Mother-to-Child Transmission of HIV". HIV.gov. May 15, 2017. Retrieved December 8, 2017.
- Cunningham AL, Donaghy H, Harman AN, Kim M, Turville SG (August 2010). "Manipulation of dendritic cell function by viruses". Current Opinion in Microbiology. 13 (4): 524–9. doi:10.1016/j.mib.2010.06.002. PMID 20598938.
- Doitsh G, Galloway NL, Geng X, Yang Z, Monroe KM, Zepeda O, et al. (January 2014). "Cell death by pyroptosis drives CD4 T-cell depletion in HIV-1 infection". Nature. 505 (7484): 509–14. Bibcode:2014Natur.505..509D. doi:10.1038/nature12940. PMC 4047036. PMID 24356306.
- Garg H, Mohl J, Joshi A (November 2012). "HIV-1 induced bystander apoptosis". Viruses. 4 (11): 3020–43. doi:10.3390/v4113020. PMC 3509682. PMID 23202514.
- Kumar V (2012). Robbins Basic Pathology (9th ed.). Elsevier Health Sciences. p. 147. ISBN 978-1-4557-3787-1.
- International Committee on Taxonomy of Viruses (2002). "61.0.6. Lentivirus". National Institutes of Health. Archived from the original on October 14, 2006. Retrieved February 28, 2006.
- International Committee on Taxonomy of Viruses (2002). "61. Retroviridae". National Institutes of Health. Archived from the original on October 2, 2006. Retrieved February 28, 2006.
- Levy JA (November 1993). "HIV pathogenesis and long-term survival". AIDS. 7 (11): 1401–10. doi:10.1097/00002030-199311000-00001. PMID 8280406.
- Smith JA, Daniel R (May 2006). "Following the path of the virus: the exploitation of host DNA repair mechanisms by retroviruses". ACS Chemical Biology. 1 (4): 217–26. doi:10.1021/cb600131q. PMID 17163676.
- ^ Siliciano RF, Greene WC (September 2011). "HIV latency". Cold Spring Harbor Perspectives in Medicine. 1 (1): a007096. doi:10.1101/cshperspect.a007096. PMC 3234450. PMID 22229121.
- Gilbert PB, McKeague IW, Eisen G, Mullins C, Guéye-NDiaye A, Mboup S, Kanki PJ (February 28, 2003). "Comparison of HIV-1 and HIV-2 infectivity from a prospective cohort study in Senegal". Statistics in Medicine. 22 (4): 573–593. doi:10.1002/sim.1342. PMID 12590415. S2CID 28523977.
- ^ Reeves JD, Doms RW (2002). "Human Immunodeficiency Virus Type 2". Journal of General Virology. 83 (Pt 6): 1253–65. doi:10.1099/0022-1317-83-6-1253. PMID 12029140.
- McGovern SL, Caselli E, Grigorieff N, Shoichet BK (2002). "A common mechanism underlying promiscuous inhibitors from virtual and high-throughput screening". Journal of Medicinal Chemistry. 45 (8): 1712–22. doi:10.1021/jm010533y. hdl:11380/977912. PMID 11931626.
- Compared with overview in: Fisher B, Harvey RP, Champe PC (2007). Lippincott's Illustrated Reviews: Microbiology. Hagerstown, MD: Lippincott Williams & Wilkins. p. 3. ISBN 978-0-7817-8215-9.
- ^ Various (2008). HIV Sequence Compendium 2008 Introduction (PDF). Retrieved March 31, 2009.
- ^ Chan DC, Fass D, Berger JM, Kim PS (April 1997). "Core structure of gp41 from the HIV envelope glycoprotein" (PDF). Cell. 89 (2): 263–73. doi:10.1016/S0092-8674(00)80205-6. PMID 9108481. S2CID 4518241.
- Klein JS, Bjorkman PJ (May 2010). "Few and far between: how HIV may be evading antibody avidity". PLOS Pathogens. 6 (5): e1000908. doi:10.1371/journal.ppat.1000908. PMC 2877745. PMID 20523901.
- National Institute of Health (June 17, 1998). "Crystal structure of key HIV protein reveals new prevention, treatment targets" (Press release). Archived from the original on February 19, 2006. Retrieved September 14, 2006.
- Behrens AJ, Vasiljevic S, Pritchard LK, Harvey DJ, Andev RS, Krumm SA, et al. (March 2016). "Composition and Antigenic Effects of Individual Glycan Sites of a Trimeric HIV-1 Envelope Glycoprotein". Cell Reports. 14 (11): 2695–706. doi:10.1016/j.celrep.2016.02.058. PMC 4805854. PMID 26972002.
- Pritchard LK, Spencer DI, Royle L, Bonomelli C, Seabright GE, Behrens AJ, et al. (June 2015). "Glycan clustering stabilizes the mannose patch of HIV-1 and preserves vulnerability to broadly neutralizing antibodies". Nature Communications. 6: 7479. Bibcode:2015NatCo...6.7479P. doi:10.1038/ncomms8479. PMC 4500839. PMID 26105115.
- Pritchard LK, Harvey DJ, Bonomelli C, Crispin M, Doores KJ (September 2015). "Cell- and Protein-Directed Glycosylation of Native Cleaved HIV-1 Envelope". Journal of Virology. 89 (17): 8932–44. doi:10.1128/JVI.01190-15. PMC 4524065. PMID 26085151.
- Crispin M, Doores KJ (April 2015). "Targeting host-derived glycans on enveloped viruses for antibody-based vaccine design". Current Opinion in Virology. 11: 63–9. doi:10.1016/j.coviro.2015.02.002. PMC 4827424. PMID 25747313.
- Julien JP, Cupo A, Sok D, Stanfield RL, Lyumkis D, Deller MC, et al. (December 2013). "Crystal structure of a soluble cleaved HIV-1 envelope trimer". Science. 342 (6165): 1477–83. Bibcode:2013Sci...342.1477J. doi:10.1126/science.1245625. PMC 3886632. PMID 24179159.
- Lyumkis D, Julien JP, de Val N, Cupo A, Potter CS, Klasse PJ, et al. (December 2013). "Cryo-EM structure of a fully glycosylated soluble cleaved HIV-1 envelope trimer". Science. 342 (6165): 1484–90. Bibcode:2013Sci...342.1484L. doi:10.1126/science.1245627. PMC 3954647. PMID 24179160.
- Sanders RW, Derking R, Cupo A, Julien JP, Yasmeen A, de Val N, et al. (September 2013). "A next-generation cleaved, soluble HIV-1 Env trimer, BG505 SOSIP.664 gp140, expresses multiple epitopes for broadly neutralizing but not non-neutralizing antibodies". PLOS Pathogens. 9 (9): e1003618. doi:10.1371/journal.ppat.1003618. PMC 3777863. PMID 24068931.
- Pritchard LK, Vasiljevic S, Ozorowski G, Seabright GE, Cupo A, Ringe R, et al. (June 2015). "Structural Constraints Determine the Glycosylation of HIV-1 Envelope Trimers". Cell Reports. 11 (10): 1604–13. doi:10.1016/j.celrep.2015.05.017. PMC 4555872. PMID 26051934.
- de Taeye SW, Ozorowski G, Torrents de la Peña A, Guttman M, Julien JP, van den Kerkhof TL, et al. (December 2015). "Immunogenicity of Stabilized HIV-1 Envelope Trimers with Reduced Exposure of Non-neutralizing Epitopes". Cell. 163 (7): 1702–15. doi:10.1016/j.cell.2015.11.056. PMC 4732737. PMID 26687358.
- Ouellet DL, Plante I, Landry P, Barat C, Janelle ME, Flamand L, Tremblay MJ, Provost P (April 2008). "Identification of functional microRNAs released through asymmetrical processing of HIV-1 TAR element". Nucleic Acids Research. 36 (7): 2353–65. doi:10.1093/nar/gkn076. PMC 2367715. PMID 18299284.
- Klase Z, Winograd R, Davis J, Carpio L, Hildreth R, Heydarian M, Fu S, McCaffrey T, Meiri E, Ayash-Rashkovsky M, Gilad S, Bentwich Z, Kashanchi F (2009). "HIV-1 TAR miRNA protects against apoptosis by altering cellular gene expression". Retrovirology. 6 (1): 18. doi:10.1186/1742-4690-6-18. PMC 2654423. PMID 19220914.
- Vasudevan AA, Smits SH, Höppner A, Häussinger D, Koenig BW, Münk C (November 2013). "Structural features of antiviral DNA cytidine deaminases". Biological Chemistry (Submitted manuscript). 394 (11): 1357–70. doi:10.1515/hsz-2013-0165. PMID 23787464. S2CID 4151961.
- Garcia JV, Miller AD (April 1991). "Serine phosphorylation-independent downregulation of cell-surface CD4 by nef". Nature. 350 (6318): 508–11. Bibcode:1991Natur.350..508G. doi:10.1038/350508a0. PMID 2014052. S2CID 1628392.
- Schwartz O, Maréchal V, Le Gall S, Lemonnier F, Heard JM (March 1996). "Endocytosis of major histocompatibility complex class I molecules is induced by the HIV-1 Nef protein". Nature Medicine. 2 (3): 338–42. doi:10.1038/nm0396-338. PMID 8612235. S2CID 7461342.
- Stumptner-Cuvelette P, Morchoisne S, Dugast M, Le Gall S, Raposo G, Schwartz O, Benaroch P (October 2001). "HIV-1 Nef impairs MHC class II antigen presentation and surface expression". Proceedings of the National Academy of Sciences of the United States of America. 98 (21): 12144–9. Bibcode:2001PNAS...9812144S. doi:10.1073/pnas.221256498. PMC 59782. PMID 11593029.
- Arrildt KT, Joseph SB, Swanstrom R (March 2012). "The HIV-1 env protein: a coat of many colors". Current HIV/AIDS Reports. 9 (1): 52–63. doi:10.1007/s11904-011-0107-3. PMC 3658113. PMID 22237899.
- ^ Berger EA, Doms RW, Fenyö EM, Korber BT, Littman DR, Moore JP, Sattentau QJ, Schuitemaker H, Sodroski J, Weiss RA (1998). "A new classification for HIV-1". Nature. 391 (6664): 240. Bibcode:1998Natur.391..240B. doi:10.1038/34571. PMID 9440686. S2CID 2159146.
- ^ Coakley E, Petropoulos CJ, Whitcomb JM (2005). "Assessing ch vbgemokine co-receptor usage in HIV". Current Opinion in Infectious Diseases. 18 (1): 9–15. doi:10.1097/00001432-200502000-00003. PMID 15647694. S2CID 30923492.
- Deng H, Liu R, Ellmeier W, Choe S, Unutmaz D, Burkhart M, Di Marzio P, Marmon S, Sutton RE, Hill CM, Davis CB, Peiper SC, Schall TJ, Littman DR, Landau NR (1996). "Identification of a major co-receptor for primary isolates of HIV-1". Nature. 381 (6584): 661–6. Bibcode:1996Natur.381..661D. doi:10.1038/381661a0. PMID 8649511. S2CID 37973935.
- Feng Y, Broder CC, Kennedy PE, Berger EA (1996). "HIV-1 entry cofactor: functional cDNA cloning of a seven-transmembrane, G protein-coupled receptor". Science. 272 (5263): 872–7. Bibcode:1996Sci...272..872F. doi:10.1126/science.272.5263.872. PMC 3412311. PMID 8629022. S2CID 44455027.
- Knight SC, Macatonia SE, Patterson S (1990). "HIV I infection of dendritic cells". International Review of Immunology. 6 (2–3): 163–75. doi:10.3109/08830189009056627. PMID 2152500.
- Tang J, Kaslow RA (2003). "The impact of host genetics on HIV infection and disease progression in the era of highly active antiretroviral therapy". AIDS. 17 (Suppl 4): S51 – S60. doi:10.1097/00002030-200317004-00006. PMID 15080180.
- Zhu T, Mo H, Wang N, Nam DS, Cao Y, Koup RA, Ho DD (1993). "Genotypic and phenotypic characterization of HIV-1 patients with primary infection". Science. 261 (5125): 1179–81. Bibcode:1993Sci...261.1179Z. doi:10.1126/science.8356453. PMID 8356453.
- van't Wout AB, Kootstra NA, Mulder-Kampinga GA, Albrecht-van Lent N, Scherpbier HJ, Veenstra J, Boer K, Coutinho RA, Miedema F, Schuitemaker H (1994). "Macrophage-tropic variants initiate human immunodeficiency virus type 1 infection after sexual, parenteral, and vertical transmission". Journal of Clinical Investigation. 94 (5): 2060–7. doi:10.1172/JCI117560. PMC 294642. PMID 7962552.
- Zhu T, Wang N, Carr A, Nam DS, Moor-Jankowski R, Cooper DA, Ho DD (1996). "Genetic characterization of human immunodeficiency virus type 1 in blood and genital secretions: evidence for viral compartmentalization and selection during sexual transmission". Journal of Virology. 70 (5): 3098–107. doi:10.1128/JVI.70.5.3098-3107.1996. PMC 190172. PMID 8627789.
- Clevestig P, Maljkovic I, Casper C, Carlenor E, Lindgren S, Navér L, Bohlin AB, Fenyö EM, Leitner T, Ehrnst A (2005). "The X4 phenotype of HIV type 1 evolves from R5 in two children of mothers, carrying X4, and is not linked to transmission". AIDS Research and Human Retroviruses. 21 (5): 371–8. doi:10.1089/aid.2005.21.371. PMID 15929699.
- Moore JP (1997). "Coreceptors: implications for HIV pathogenesis and therapy". Science. 276 (5309): 51–2. doi:10.1126/science.276.5309.51. PMID 9122710. S2CID 33262844.
- Karlsson A, Parsmyr K, Aperia K, Sandström E, Fenyö EM, Albert J (1994). "MT-2 cell tropism of human immunodeficiency virus type 1 isolates as a marker for response to treatment and development of drug resistance". The Journal of Infectious Diseases. 170 (6): 1367–75. doi:10.1093/infdis/170.6.1367. PMID 7995974.
- Koot M, van 't Wout AB, Kootstra NA, de Goede RE, Tersmette M, Schuitemaker H (1996). "Relation between changes in cellular load, evolution of viral phenotype, and the clonal composition of virus populations in the course of human immunodeficiency virus type 1 infection". The Journal of Infectious Diseases. 173 (2): 349–54. doi:10.1093/infdis/173.2.349. PMID 8568295.
- Cheney K, McKnight A (2010). "HIV-2 Tropism and Disease". Lentiviruses and Macrophages: Molecular and Cellular Interactions. Caister Academic Press. ISBN 978-1-904455-60-8.
- ^ Chan DC, Kim PS (1998). "HIV entry and its inhibition". Cell. 93 (5): 681–4. doi:10.1016/S0092-8674(00)81430-0. PMID 9630213. S2CID 10544941.
- ^ Wyatt R, Sodroski J (1998). "The HIV-1 envelope glycoproteins: fusogens, antigens, and immunogens". Science. 280 (5371): 1884–8. Bibcode:1998Sci...280.1884W. doi:10.1126/science.280.5371.1884. PMID 9632381.
- ^ Arthos J, Cicala C, Martinelli E, Macleod K, Van Ryk D, Wei D, Xiao Z, Veenstra TD, Conrad TP, Lempicki RA, McLaughlin S, Pascuccio M, Gopaul R, McNally J, Cruz CC, Censoplano N, Chung E, Reitano KN, Kottilil S, Goode DJ, Fauci AS (2008). "HIV-1 envelope protein binds to and signals through integrin alpha(4)beta(7), the gut mucosal homing receptor for peripheral T cells". Nature Immunology. 9 (3): 301–9. doi:10.1038/ni1566. PMID 18264102. S2CID 205361178.
- ^ Pope M, Haase AT (2003). "Transmission, acute HIV-1 infection and the quest for strategies to prevent infection". Nature Medicine. 9 (7): 847–52. doi:10.1038/nm0703-847. PMID 12835704. S2CID 26570505.
- Haedicke J, Brown C, Naghavi MH (August 2009). "The brain-specific factor FEZ1 is a determinant of neuronal susceptibility to HIV-1 infection". Proceedings of the National Academy of Sciences. 106 (33): 14040–14045. Bibcode:2009PNAS..10614040H. doi:10.1073/pnas.0900502106. PMC 2729016. PMID 19667186.
- Daecke J, Fackler OT, Dittmar MT, Kräusslich HG (2005). "Involvement of clathrin-mediated endocytosis in human immunodeficiency virus type 1 entry". Journal of Virology. 79 (3): 1581–1594. doi:10.1128/jvi.79.3.1581-1594.2005. PMC 544101. PMID 15650184.
- Miyauchi K, Kim Y, Latinovic O, Morozov V, Melikyan GB (2009). "HIV Enters Cells via Endocytosis and Dynamin-Dependent Fusion with Endosomes". Cell. 137 (3): 433–444. doi:10.1016/j.cell.2009.02.046. PMC 2696170. PMID 19410541.
- Koch P, Lampe M, Godinez WJ, Müller B, Rohr K, Kräusslich HG, Lehmann MJ (2009). "Visualizing fusion of pseudotyped HIV-1 particles in real time by live cell microscopy". Retrovirology. 6: 84. doi:10.1186/1742-4690-6-84. PMC 2762461. PMID 19765276.
- Thorley JA, McKeating JA, Rappoport JZ (2010). "Mechanisms of viral entry: sneaking in the front door". Protoplasma. 244 (1–4): 15–24. doi:10.1007/s00709-010-0152-6. PMC 3038234. PMID 20446005.
- Permanyer M, Ballana E, Esté JA (2010). "Endocytosis of HIV: anything goes". Trends in Microbiology. 18 (12): 543–551. doi:10.1016/j.tim.2010.09.003. PMID 20965729.
- ^ Zheng YH, Lovsin N, Peterlin BM (2005). "Newly identified host factors modulate HIV replication". Immunology Letters. 97 (2): 225–34. doi:10.1016/j.imlet.2004.11.026. PMID 15752562.
- "IV. Viruses> F. Animal Virus Life Cycles > 3. The Life Cycle of HIV". Doc Kaiser's Microbiology Home Page. Community College of Baltimore County. January 2008. Archived from the original on July 26, 2010.
- Hiscott J, Kwon H, Génin P (2001). "Hostile takeovers: viral appropriation of the NF-kB pathway". Journal of Clinical Investigation. 107 (2): 143–151. doi:10.1172/JCI11918. PMC 199181. PMID 11160127.
- Keane SC, Heng X, Lu K, Kharytonchyk S, Ramakrishnan V, Carter G, Barton S, Hosic A, Florwick A, Santos J, Bolden NC (May 22, 2015). "Structure of the HIV-1 RNA packaging signal". Science. 348 (6237): 917–921. Bibcode:2015Sci...348..917K. doi:10.1126/science.aaa9266. ISSN 0036-8075. PMC 4492308. PMID 25999508.
- Keane SC, Van V, Frank HM, Sciandra CA, McCowin S, Santos J, Heng X, Summers MF (October 10, 2016). "NMR detection of intermolecular interaction sites in the dimeric 5′-leader of the HIV-1 genome". Proceedings of the National Academy of Sciences. 113 (46): 13033–13038. Bibcode:2016PNAS..11313033K. doi:10.1073/pnas.1614785113. ISSN 0027-8424. PMC 5135362. PMID 27791166.
- Ocwieja KE, Sherrill-Mix S, Mukherjee R, Custers-Allen R, David P, Brown M, et al. (November 2012). "Dynamic regulation of HIV-1 mRNA populations analyzed by single-molecule enrichment and long-read sequencing". Nucleic Acids Research. 40 (20): 10345–55. doi:10.1093/nar/gks753. PMC 3488221. PMID 22923523.
- Pollard VW, Malim MH (1998). "The HIV-1 Rev protein". Annual Review of Microbiology. 52: 491–532. doi:10.1146/annurev.micro.52.1.491. PMID 9891806.
- Butsch M, Boris-Lawrie K (April 2002). "Destiny of unspliced retroviral RNA: ribosome and/or virion?". Journal of Virology. 76 (7): 3089–94. doi:10.1128/JVI.76.7.3089-3094.2002. PMC 136024. PMID 11884533.
- Hellmund C, Lever AM (July 2016). "Coordination of Genomic RNA Packaging with Viral Assembly in HIV-1". Viruses. 8 (7): 192. doi:10.3390/v8070192. PMC 4974527. PMID 27428992.
- Soto-Rifo R, Limousin T, Rubilar PS, Ricci EP, Décimo D, Moncorgé O, et al. (March 2012). "Different effects of the TAR structure on HIV-1 and HIV-2 genomic RNA translation". Nucleic Acids Research. 40 (6): 2653–67. doi:10.1093/nar/gkr1093. PMC 3315320. PMID 22121214.
- Saad JS, Muriaux DM (July 28, 2015). Role of Lipids in Virus Assembly. Frontiers Media SA. ISBN 978-2-88919-582-4.
- Ricci EP, Herbreteau CH, Decimo D, Schaupp A, Datta SA, Rein A, et al. (July 2008). "In vitro expression of the HIV-2 genomic RNA is controlled by three distinct internal ribosome entry segments that are regulated by the HIV protease and the Gag polyprotein". RNA. 14 (7): 1443–55. doi:10.1261/rna.813608. PMC 2441975. PMID 18495939.
- ^ Hu WS, Temin HM (1990). "Retroviral recombination and reverse transcription". Science. 250 (4985): 1227–33. Bibcode:1990Sci...250.1227H. doi:10.1126/science.1700865. PMID 1700865.
- ^ Charpentier C, Nora T, Tenaillon O, Clavel F, Hance AJ (2006). "Extensive recombination among human immunodeficiency virus type 1 quasispecies makes an important contribution to viral diversity in individual patients". Journal of Virology. 80 (5): 2472–82. doi:10.1128/JVI.80.5.2472-2482.2006. PMC 1395372. PMID 16474154.
- Nora T, Charpentier C, Tenaillon O, Hoede C, Clavel F, Hance AJ (2007). "Contribution of recombination to the evolution of human immunodeficiency viruses expressing resistance to antiretroviral treatment". Journal of Virology. 81 (14): 7620–8. doi:10.1128/JVI.00083-07. PMC 1933369. PMID 17494080.
- Chen J, Powell D, Hu WS (2006). "High frequency of genetic recombination is a common feature of primate lentivirus replication". Journal of Virology. 80 (19): 9651–8. doi:10.1128/JVI.00936-06. PMC 1617242. PMID 16973569.
- ^ Bonhoeffer S, Chappey C, Parkin NT, Whitcomb JM, Petropoulos CJ (2004). "Evidence for positive epistasis in HIV-1". Science. 306 (5701): 1547–50. Bibcode:2004Sci...306.1547B. doi:10.1126/science.1101786. PMID 15567861. S2CID 45784964.
- Israël N, Gougerot-Pocidalo MA (1997). "Oxidative stress in human immunodeficiency virus infection". Cellular and Molecular Life Sciences. 53 (11–12): 864–70. doi:10.1007/s000180050106. PMC 11147326. PMID 9447238. S2CID 22663454.
- Michod RE, Bernstein H, Nedelcu AM (May 2008). "Adaptive value of sex in microbial pathogens" (PDF). Infection, Genetics and Evolution. 8 (3): 267–85. Bibcode:2008InfGE...8..267M. doi:10.1016/j.meegid.2008.01.002. PMID 18295550. Archived from the original (PDF) on May 16, 2017. Retrieved May 10, 2013.
- Hallenberger S, Bosch V, Angliker H, Shaw E, Klenk HD, Garten W (November 26, 1992). "Inhibition of furin-mediated cleavage activation of HIV-1 glycoprotein gp160". Nature. 360 (6402): 358–61. Bibcode:1992Natur.360..358H. doi:10.1038/360358a0. PMID 1360148. S2CID 4306605.
- Gelderblom HR (1997). "Fine structure of HIV and SIV" (PDF). In Los Alamos National Laboratory (ed.). HIV sequence compendium. Los Alamos National Laboratory. pp. 31–44.
- ^ Zhang C, Zhou S, Groppelli E, Pellegrino P, Williams I, Borrow P, Chain BM, Jolly C (2015). "Hybrid Spreading Mechanisms and T Cell Activation Shape the Dynamics of HIV-1 Infection". PLOS Computational Biology. 11 (4): e1004179. arXiv:1503.08992. Bibcode:2015PLSCB..11E4179Z. doi:10.1371/journal.pcbi.1004179. PMC 4383537. PMID 25837979.
- ^ Jolly C, Kashefi K, Hollinshead M, Sattentau QJ (2004). "HIV-1 cell to cell transfer across an Env-induced, actin-dependent synapse". Journal of Experimental Medicine. 199 (2): 283–293. doi:10.1084/jem.20030648. PMC 2211771. PMID 14734528.
- Sattentau Q (2008). "Avoiding the void: cell-to-cell spread of human viruses". Nature Reviews Microbiology. 6 (11): 815–826. doi:10.1038/nrmicro1972. PMID 18923409. S2CID 20991705.
- Duncan CJ, Russell RA, Sattentau QJ (2013). "High multiplicity HIV-1 cell-to-cell transmission from macrophages to CD4+ T cells limits antiretroviral efficacy". AIDS. 27 (14): 2201–2206. doi:10.1097/QAD.0b013e3283632ec4. PMC 4714465. PMID 24005480.
- Sewald X, Gonzalez DG, Haberman AM, Mothes W (2012). "In vivo imaging of virological synapses". Nature Communications. 3: 1320. Bibcode:2012NatCo...3.1320S. doi:10.1038/ncomms2338. PMC 3784984. PMID 23271654.
- Sigal A, Kim JT, Balazs AB, Dekel E, Mayo A, Milo R, Baltimore D (2011). "Cell-to-cell spread of HIV permits ongoing replication despite antiretroviral therapy". Nature. 477 (7362): 95–98. Bibcode:2011Natur.477...95S. doi:10.1038/nature10347. PMID 21849975. S2CID 4409389.
- ^ Robertson DL, Hahn BH, Sharp PM (1995). "Recombination in AIDS viruses". Journal of Molecular Evolution. 40 (3): 249–59. Bibcode:1995JMolE..40..249R. doi:10.1007/BF00163230. PMID 7723052. S2CID 19728830.
- Rambaut A, Posada D, Crandall KA, Holmes EC (January 2004). "The causes and consequences of HIV evolution". Nature Reviews Genetics. 5 (52–61): 52–61. doi:10.1038/nrg1246. PMID 14708016. S2CID 5790569.
- Perelson AS, Ribeiro RM (October 2008). "Estimating drug efficacy and viral dynamic parameters: HIV and HCV". Statistics in Medicine. 27 (23): 4647–57. doi:10.1002/sim.3116. PMID 17960579. S2CID 33662579.
- ^ Sodora DL, Allan JS, Apetrei C, Brenchley JM, Douek DC, Else JG, Estes JD, Hahn BH, Hirsch VM, Kaur A, Kirchhoff F, Muller-Trutwin M, Pandrea I, Schmitz JE, Silvestri G (2009). "Toward an AIDS vaccine: lessons from natural simian immunodeficiency virus infections of African nonhuman primate hosts". Nature Medicine. 15 (8): 861–865. doi:10.1038/nm.2013. PMC 2782707. PMID 19661993.
- Holzammer S, Holznagel E, Kaul A, Kurth R, Norley S (2001). "High virus loads in naturally and experimentally SIVagm-infected African green monkeys". Virology. 283 (2): 324–31. doi:10.1006/viro.2001.0870. PMID 11336557.
- Kurth R, Norley S (1996). "Why don't the natural hosts of SIV develop simian AIDS?". The Journal of NIH Research. 8: 33–37.
- Baier M, Dittmar MT, Cichutek K, Kurth R (1991). "Development of vivo of genetic variability of simian immunodeficiency virus". Proceedings of the National Academy of Sciences of the United States of America. 88 (18): 8126–30. Bibcode:1991PNAS...88.8126B. doi:10.1073/pnas.88.18.8126. PMC 52459. PMID 1896460.
- Daniel MD, King NW, Letvin NL, Hunt RD, Sehgal PK, Desrosiers RC (1984). "A new type D retrovirus isolated from macaques with an immunodeficiency syndrome". Science. 223 (4636): 602–5. Bibcode:1984Sci...223..602D. doi:10.1126/science.6695172. PMID 6695172.
- ^ Keele BF, Jones JH, Terio KA, Estes JD, Rudicell RS, Wilson ML, Li Y, Learn GH, Beasley TM, Schumacher-Stankey J, Wroblewski E, Mosser A, Raphael J, Kamenya S, Lonsdorf EV, Travis DA, Mlengeya T, Kinsel MJ, Else JG, Silvestri G, Goodall J, Sharp PM, Shaw GM, Pusey AE, Hahn BH (2009). "Increased mortality and AIDS-like immunopathology in wild chimpanzees infected with SIVcpz". Nature. 460 (7254): 515–519. Bibcode:2009Natur.460..515K. doi:10.1038/nature08200. PMC 2872475. PMID 19626114.
- Schindler M, Münch J, Kutsch O, Li H, Santiago ML, Bibollet-Ruche F, Müller-Trutwin MC, Novembre FJ, Peeters M, Courgnaud V, Bailes E, Roques P, Sodora DL, Silvestri G, Sharp PM, Hahn BH, Kirchhoff F (2006). "Nef-mediated suppression of T cell activation was lost in a lentiviral lineage that gave rise to HIV-1". Cell. 125 (6): 1055–67. doi:10.1016/j.cell.2006.04.033. PMID 16777597. S2CID 15132918.
- Thomson MM, Pérez-Alvarez L, Nájera R (2002). "Molecular epidemiology of HIV-1 genetic forms and its significance for vaccine development and therapy". The Lancet Infectious Diseases. 2 (8): 461–471. doi:10.1016/S1473-3099(02)00343-2. PMID 12150845.
- Carr JK, Foley BT, Leitner T, Salminen M, Korber B, McCutchan F (1998). "Reference sequences representing the principal genetic diversity of HIV-1 in the pandemic" (PDF). In Los Alamos National Laboratory (ed.). HIV sequence compendium. Los Alamos, New Mexico: Los Alamos National Laboratory. pp. 10–19.
- Osmanov S, Pattou C, Walker N, Schwardländer B, Esparza J (2002). "Estimated global distribution and regional spread of HIV-1 genetic subtypes in the year 2000". Journal of Acquired Immune Deficiency Syndromes. 29 (2): 184–190. doi:10.1097/00042560-200202010-00013. PMID 11832690. S2CID 12536801.
- Perrin L, Kaiser L, Yerly S (2003). "Travel and the spread of HIV-1 genetic variants". The Lancet Infectious Diseases. 3 (1): 22–27. doi:10.1016/S1473-3099(03)00484-5. PMID 12505029.
- ^ Plantier JC, Leoz M, Dickerson JE, De Oliveira F, Cordonnier F, Lemée V, Damond F, Robertson DL, Simon F (August 2009). "A new human immunodeficiency virus derived from gorillas". Nature Medicine. 15 (8): 871–2. doi:10.1038/nm.2016. PMID 19648927. S2CID 76837833.
- Smith L (August 3, 2009). "Woman found carrying new strain of HIV from gorillas". The Independent. Retrieved November 27, 2015.
- Sharp PM, Hahn BH (August 2010). "The evolution of HIV-1 and the origin of AIDS". Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences. 365 (1552): 2487–94. doi:10.1098/rstb.2010.0031. PMC 2935100. PMID 20643738.
- Keele BF, Van Heuverswyn F, Li Y, Bailes E, Takehisa J, Santiago ML, et al. (July 2006). "Chimpanzee reservoirs of pandemic and nonpandemic HIV-1". Science. 313 (5786): 523–6. Bibcode:2006Sci...313..523K. doi:10.1126/science.1126531. PMC 2442710. PMID 16728595.
- ^ Kumaranayake L, Watts C (2001). "Resource allocation and priority setting of HIV/AIDS interventions: addressing the generalized epidemic in sub-Saharan Africa". Journal of International Development. 13 (4): 451–466. doi:10.1002/jid.797.
- Kleinman S (September 2004). "Patient information: Blood donation and transfusion". Uptodate. Archived from the original on April 12, 2008.
- ^ Centers for Disease Control and Prevention (2001). "Revised guidelines for HIV counseling, testing, and referral". MMWR Recommendations and Reports. 50 (RR–19): 1–57. PMID 11718472.
- Celum CL, Coombs RW, Lafferty W, Inui TS, Louie PH, Gates CA, McCreedy BJ, Egan R, Grove T, Alexander S (1991). "Indeterminate human immunodeficiency virus type 1 western blots: seroconversion risk, specificity of supplemental tests, and an algorithm for evaluation". The Journal of Infectious Diseases. 164 (4): 656–664. doi:10.1093/infdis/164.4.656. PMID 1894929.
- "Country Comparison :: HIV/AIDS - Deaths". The World Factbook, Central Intelligence Agency. Archived from the original on April 30, 2017. Retrieved November 22, 2015.
- Chou R, Selph S, Dana T, Bougatsos C, Zakher B, Blazina I, Korthuis PT (November 2012). "Screening for HIV: systematic review to update the 2005 U.S. Preventive Services Task Force recommendation". Annals of Internal Medicine. 157 (10): 706–18. doi:10.7326/0003-4819-157-10-201211200-00007. PMID 23165662. S2CID 27494096.
- Chou R, Huffman LH, Fu R, Smits AK, Korthuis PT (July 2005). "Screening for HIV: a review of the evidence for the U.S. Preventive Services Task Force". Annals of Internal Medicine. 143 (1): 55–73. doi:10.7326/0003-4819-143-1-200507050-00010. PMID 15998755. S2CID 24086322.
- Tolle MA, Schwarzwald HL (July 2010). "Postexposure prophylaxis against human immunodeficiency virus". American Family Physician. 82 (2): 161–6. PMID 20642270. Archived from the original on November 28, 2023.
- "Quick Reference Guide—Laboratory Testing for the Diagnosis of HIV Infection: Updated Recommendations" (PDF). Centers for Disease Control and Prevention. New York State Department of Health. June 27, 2014. pp. 1–2. Archived from the original (PDF) on March 2, 2017. Retrieved April 13, 2017.
- "HIV Treatment: FDA-Approved HIV Medicines". AIDSinfo. Archived from the original on February 23, 2017. Retrieved October 7, 2016.
- Rodari A, Darcis G, Van Lint CM (September 29, 2021). "The Current Status of Latency Reversing Agents for HIV-1 Remission". Annual Review of Virology. 8 (1): 491–514. doi:10.1146/annurev-virology-091919-103029. ISSN 2327-056X. PMID 34586875.
- Swiss National AIDS Commission (October 15, 2016). "The Swiss statement". HIV i-Base. Retrieved April 2, 2019.
- Vernazza P, Bernard EJ (January 29, 2016). "HIV is not transmitted under fully suppressive therapy: The Swiss Statement—eight years later". Swiss Medical Weekly. 146: w14246. doi:10.4414/smw.2016.14246. PMID 26824882.
- The Lancet HIV (November 2017). "U=U taking off in 2017". Editorial. The Lancet. HIV. 4 (11): e475. doi:10.1016/S2352-3018(17)30183-2. PMID 29096785.
- "Can't Pass It On". Terrence Higgins Trust. 2019. Archived from the original on April 7, 2019. Retrieved April 2, 2019.
- Bavinton BR, Pinto AN, Phanuphak N, Grinsztejn B, Prestage GP, Zablotska-Manos IB, et al. (August 2018). "Viral suppression and HIV transmission in serodiscordant male couples: an international, prospective, observational, cohort study". The Lancet. HIV. 5 (8): e438 – e447. doi:10.1016/S2352-3018(18)30132-2. PMID 30025681. S2CID 51702998.
- Rodger AJ, Cambiano V, Bruun T, Vernazza P, Collins S, van Lunzen J, et al. (July 2016). "Sexual Activity Without Condoms and Risk of HIV Transmission in Serodifferent Couples When the HIV-Positive Partner Is Using Suppressive Antiretroviral Therapy". JAMA. 316 (2): 171–81. doi:10.1001/jama.2016.5148. PMID 27404185.
- Rodger A( (July 2018). Risk of HIV transmission through condomless sex in MSM couples with suppressive ART: The PARTNER2 Study extended results in gay men. AIDS2018: 22nd International AIDS Conference. Amsterdam, the Netherlands. Retrieved April 2, 2019.
- ^ Hoffman H (January 10, 2019). "The science is clear: with HIV, undetectable equals untransmittable" (Press release). National Institutes of Health. National Institute of Allergy and Infectious Diseases. Retrieved May 3, 2019.
NIAID Director Anthony S. Fauci, M.D., and colleagues summarize results from large clinical trials and cohort studies validating U=U. The landmark NIH-funded HPTN 052 clinical trial showed that no linked HIV transmissions occurred among HIV serodifferent heterosexual couples when the partner living with HIV had a durably suppressed viral load. Subsequently, the PARTNER and Opposites Attract studies confirmed these findings and extended them to male-male couples. ... The success of U=U as an HIV prevention method depends on achieving and maintaining an undetectable viral load by taking ART daily as prescribed.
- Cohen MS, Chen YQ, McCauley M, Gamble T, Hosseinipour MC, Kumarasamy N, et al. (September 2016). "Antiretroviral Therapy for the Prevention of HIV-1 Transmission". The New England Journal of Medicine. 375 (9): 830–9. doi:10.1056/NEJMoa1600693. PMC 5049503. PMID 27424812.
- Hodson M (November 17, 2017). U=U: Talking to patients about transmission risk (PDF). British HIV Association Autumn Conference 2017. Retrieved May 3, 2019. (abstract for presentation on behalf of NAM / Aidsmap)
- "Consensus statement: Risk of Sexual Transmission of HIV from a Person Living with HIV who has an Undetectable Viral Load". Prevention Access Campaign. July 21, 2016. Retrieved April 2, 2019. Note: When the statement and list of endorsements was retrieved, it had last been updated on 23 August 2018 and included "over 850 organizations from nearly 100 countries."
- Zhu J, Hladik F, Woodward A, Klock A, Peng T, Johnston C, et al. (August 2009). "Persistence of HIV-1 receptor-positive cells after HSV-2 reactivation is a potential mechanism for increased HIV-1 acquisition". Nature Medicine. 15 (8): 886–92. doi:10.1038/nm.2006. PMC 2723183. PMID 19648930.
- Looker KJ, Elmes JA, Gottlieb SL, Schiffer JT, Vickerman P, Turner KM, Boily MC (December 2017). "Effect of HSV-2 infection on subsequent HIV acquisition: an updated systematic review and meta-analysis". The Lancet. Infectious Diseases. 17 (12): 1303–1316. doi:10.1016/S1473-3099(17)30405-X. PMC 5700807. PMID 28843576.
- "On this day". News & Record. May 18, 2020. pp. 2A.
- Mandell GL, Bennett JE, Dolin R, eds. (2010). "Chapter 169". Mandell, Douglas, and Bennett's principles and practice of infectious diseases (7th ed.). Philadelphia: Churchill Livingstone/Elsevier. ISBN 978-0-443-06839-3.
- Gottlieb MS (2006). "Pneumocystis pneumonia—Los Angeles. 1981". American Journal of Public Health. 96 (6): 980–1, discussion 982–3. doi:10.2105/AJPH.96.6.980. PMC 1470612. PMID 16714472. Archived from the original on April 22, 2009.
- Friedman-Kien AE (October 1981). "Disseminated Kaposi's sarcoma syndrome in young homosexual men". Journal of the American Academy of Dermatology. 5 (4): 468–71. doi:10.1016/S0190-9622(81)80010-2. PMID 7287964.
- Hymes KB, Cheung T, Greene JB, Prose NS, Marcus A, Ballard H, William DC, Laubenstein LJ (September 1981). "Kaposi's sarcoma in homosexual men — a report of eight cases". The Lancet. 2 (8247): 598–600. doi:10.1016/S0140-6736(81)92740-9. PMID 6116083. S2CID 43529542.
- ^ Basavapathruni A, Anderson KS (December 2007). "Reverse transcription of the HIV-1 pandemic". The FASEB Journal. 21 (14): 3795–3808. doi:10.1096/fj.07-8697rev. PMID 17639073. S2CID 24960391.
- Lederberg J, ed. (2000). Encyclopedia of Microbiology (2nd ed.). Burlington: Elsevier. p. 106. ISBN 978-0-08-054848-7. Retrieved June 9, 2016.
- Centers for Disease Control (1982). "Persistent, generalized lymphadenopathy among homosexual males". Morbidity and Mortality Weekly Report. 31 (19): 249–251. PMID 6808340.
- ^ Barré-Sinoussi F, Chermann JC, Rey F, Nugeyre MT, Chamaret S, Gruest J, Dauguet C, Axler-Blin C, Vézinet-Brun F, Rouzioux C, Rozenbaum W, Montagnier L (1983). "Isolation of a T-lymphotropic retrovirus from a patient at risk for acquired immune deficiency syndrome (AIDS)". Science. 220 (4599): 868–871. Bibcode:1983Sci...220..868B. doi:10.1126/science.6189183. PMID 6189183. S2CID 390173.
- ^ Centers for Disease Control (1982). "Opportunistic infections and Kaposi's sarcoma among Haitians in the United States". Morbidity and Mortality Weekly Report. 31 (26): 353–354, 360–361. PMID 6811853.
- Altman LK (May 11, 1982). "New homosexual disorder worries health officials". The New York Times. Retrieved August 31, 2011.
- Gilman SL (1987). GilmanSL (ed.). "AIDS and Syphilis: The Iconography of Disease". October. 43: 87–107. doi:10.2307/3397566. JSTOR 3397566.
- "Making Headway Under Hellacious Circumstances" (PDF). American Association for the Advancement of Science. July 28, 2006. Archived from the original (PDF) on June 24, 2008. Retrieved June 23, 2008.
- Kher U (July 27, 1982). "A Name for the Plague". Time. Archived from the original on March 7, 2008. Retrieved March 10, 2008.
- Centers for Disease Control (1982). "Update on acquired immune deficiency syndrome (AIDS)—United States". Morbidity and Mortality Weekly Report. 31 (37): 507–508, 513–514. PMID 6815471.
- Gallo RC, Sarin PS, Gelmann EP, Robert-Guroff M, Richardson E, Kalyanaraman VS, Mann D, Sidhu GD, Stahl RE, Zolla-Pazner S, Leibowitch J, Popovic M (1983). "Isolation of human T-cell leukemia virus in acquired immune deficiency syndrome (AIDS)". Science. 220 (4599): 865–867. Bibcode:1983Sci...220..865G. doi:10.1126/science.6601823. PMID 6601823.
- "The 2008 Nobel Prize in Physiology or Medicine - Press Release". www.nobelprize.org. Retrieved January 28, 2018.
- Crewdson J (May 30, 1991). "GALLO ADMITS FRENCH DISCOVERED AIDS VIRUS". Chicago Tribune. Retrieved April 25, 2020.
- Aldrich R, Wotherspoon G, eds. (2001). Who's who in gay and lesbian history. London: Routledge. p. 154. ISBN 978-0-415-22974-6.
- Levy JA, et al. (1984). "Isolation of lymphocytopathic retroviruses from San Francisco patients with AIDS". Science. 225 (4664): 840–842. Bibcode:1984Sci...225..840L. doi:10.1126/science.6206563. PMID 6206563.
- Levy JA, Kaminsky LS, Morrow WJ, Steimer K, Luciw P, Dina D, Hoxie J, Oshiro L (1985). "Infection by the retrovirus associated with the acquired immunodeficiency syndrome". Annals of Internal Medicine. 103 (5): 694–699. doi:10.7326/0003-4819-103-5-694. PMID 2996401.
- Sharp PM, Hahn BH (2011). "Origins of HIV and the AIDS Pandemic". Cold Spring Harbor Perspectives in Medicine. 1 (1): a006841. doi:10.1101/cshperspect.a006841. PMC 3234451. PMID 22229120.
- Faria NR, Rambaut A, Suchard MA, Baele G, Bedford T, Ward MJ, Tatem AJ, Sousa JD, Arinaminpathy N, Pépin J, Posada D, Peeters M, Pybus OG, Lemey P (2014). "The early spread and epidemic ignition of HIV-1 in human populations". Science. 346 (6205): 56–61. Bibcode:2014Sci...346...56F. doi:10.1126/science.1256739. PMC 4254776. PMID 25278604.
- Gao F, Bailes E, Robertson DL, Chen Y, Rodenburg CM, Michael SF, Cummins LB, Arthur LO, Peeters M, Shaw GM, Sharp PM, Hahn BH (1999). "Origin of HIV-1 in the chimpanzee Pan troglodytes troglodytes". Nature. 397 (6718): 436–41. Bibcode:1999Natur.397..436G. doi:10.1038/17130. PMID 9989410. S2CID 4432185.
- Keele BF, Van Heuverswyn F, Li Y, Bailes E, Takehisa J, Santiago ML, Bibollet-Ruche F, Chen Y, Wain LV, Liegeois F, Loul S, Ngole EM, Bienvenue Y, Delaporte E, Brookfield JF, Sharp PM, Shaw GM, Peeters M, Hahn BH (2006). "Chimpanzee reservoirs of pandemic and nonpandemic HIV-1". Science. 313 (5786): 523–6. Bibcode:2006Sci...313..523K. doi:10.1126/science.1126531. PMC 2442710. PMID 16728595.
- Goodier JL, Kazazian HH (2008). "Retrotransposons revisited: the restraint and rehabilitation of parasites". Cell. 135 (1): 23–35. doi:10.1016/j.cell.2008.09.022. PMID 18854152. S2CID 3093360.
- Sharp PM, Bailes E, Chaudhuri RR, Rodenburg CM, Santiago MO, Hahn BH (2001). "The origins of acquired immune deficiency syndrome viruses: where and when?". Philosophical Transactions of the Royal Society B. 356 (1410): 867–76. doi:10.1098/rstb.2001.0863. PMC 1088480. PMID 11405934.
- Kalish ML, Wolfe ND, Ndongmo CB, McNicholl J, Robbins KE, Aidoo M, Fonjungo PN, Alemnji G, Zeh C, Djoko CF, Mpoudi-Ngole E, Burke DS, Folks TM (2005). "Central African hunters exposed to simian immunodeficiency virus". Emerging Infectious Diseases. 11 (12): 1928–30. doi:10.3201/eid1112.050394. PMC 3367631. PMID 16485481.
- ^ Marx PA, Alcabes PG, Drucker E (2001). "Serial human passage of simian immunodeficiency virus by unsterile injections and the emergence of epidemic human immunodeficiency virus in Africa". Philosophical Transactions of the Royal Society B. 356 (1410): 911–20. doi:10.1098/rstb.2001.0867. PMC 1088484. PMID 11405938.
- Worobey M, Gemmel M, Teuwen DE, Haselkorn T, Kunstman K, Bunce M, Muyembe JJ, Kabongo JM, Kalengayi RM, Van Marck E, Gilbert MT, Wolinsky SM (2008). "Direct evidence of extensive diversity of HIV-1 in Kinshasa by 1960". Nature. 455 (7213): 661–4. Bibcode:2008Natur.455..661W. doi:10.1038/nature07390. PMC 3682493. PMID 18833279.
- ^ de Sousa JD, Müller V, Lemey P, Vandamme AM (2010). Martin DP (ed.). "High GUD incidence in the early 20th century created a particularly permissive time window for the origin and initial spread of epidemic HIV strains". PLOS ONE. 5 (4): e9936. Bibcode:2010PLoSO...5.9936S. doi:10.1371/journal.pone.0009936. PMC 2848574. PMID 20376191.
- Zhu T, Korber BT, Nahmias AJ, Hooper E, Sharp PM, Ho DD (1998). "An African HIV-1 Sequence from 1959 and Implications for the Origin of the epidemic". Nature. 391 (6667): 594–7. Bibcode:1998Natur.391..594Z. doi:10.1038/35400. PMID 9468138. S2CID 4416837.
- Kolata G (October 28, 1987). "Boy's 1969 death suggests AIDS invaded U.S. several times". The New York Times. Retrieved February 11, 2009.
- Chitnis A, Rawls D, Moore J (January 2000). "Origin of HIV type 1 in colonial French Equatorial Africa?". AIDS Research and Human Retroviruses. 16 (1): 5–8. doi:10.1089/088922200309548. PMID 10628811. S2CID 17783758.
- McNeil D Jr (September 16, 2010). "Precursor to H.I.V. was in monkeys for millennia". The New York Times. Archived from the original on January 3, 2022. Retrieved September 17, 2010.
Dr. Marx believes that the crucial event was the introduction into Africa of millions of inexpensive, mass-produced syringes in the 1950s. ... suspect that the growth of colonial cities is to blame. Before 1910, no Central African town had more than 10,000 people. But urban migration rose, increasing sexual contacts and leading to red-light districts.
- ^ Wertheim JO, Worobey M (May 2009). "Dating the age of the SIV lineages that gave rise to HIV-1 and HIV-2". PLOS Computational Biology. 5 (5): e1000377. Bibcode:2009PLSCB...5E0377W. doi:10.1371/journal.pcbi.1000377. PMC 2669881. PMID 19412344.
Further reading
- Berlier W, Bourlet T, Lawrence P, Hamzeh H, Lambert C, Genin C, Verrier B, Dieu-Nosjean MC, Pozzetto B, Delézay O (2005). "Selective sequestration of X4 isolates by human genital epithelial cells: Implication for virus tropism selection process during sexual transmission of HIV". Journal of Medical Virology. 77 (4): 465–74. doi:10.1002/jmv.20478. PMID 16254974. S2CID 25762969.
- Joint United Nations Programme on HIV/AIDS (UNAIDS) (2011). Global HIV/AIDS Response, Epidemic update and health sector progress towards universal access (PDF). Joint United Nations Programme on HIV/AIDS.
- Muciaccia B, Padula F, Vicini E, Gandini L, Lenzi A, Stefanini M (2005). "Beta-chemokine receptors 5 and 3 are expressed on the head region of human spermatozoon". The FASEB Journal. 19 (14): 2048–50. doi:10.1096/fj.05-3962fje. hdl:11573/361629. PMID 16174786. S2CID 7928126.
External links
| Sexually transmitted infections (STI) | |
|---|---|
| Bacterial | |
| Protozoal | |
| Parasitic | |
| Viral | |
| General inflammation |
|
| Virus: Reverse transcribing viruses (Revtraviricetes) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Blubervirales |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ortervirales |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Endogenous | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Science Breakthroughs of the Year | |
|---|---|
| Science journal |
|
| Taxon identifiers | |
|---|---|
| HIV | |
